Homozygous complement component CD55 mutations cause novel gastrointestinal syndrome
1. Researchers used whole-exome sequencing to define the novel CHAPLE syndrome, characterized by a homozygous CD55 mutation with hyperactivation of complement, angiopathic thrombosis, and protein-losing enteropathy.
2. Eculizumab, an antibody against complement component C5a, reduced C5a levels in T-cell cultures from patients with CHAPLE syndrome and may be a potential therapeutic option for CHAPLE syndrome warranting further investigation.
Evidence Rating Level: 3 (Average)
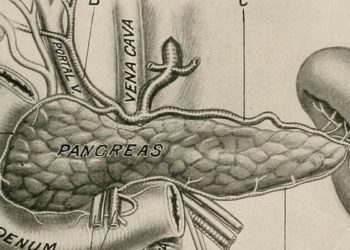
Study Rundown: Genetic variants in CD55, a cell surface glycoprotein that attenuates activation of the complement system, is associated with paroxysmal nocturnal hemoglobinuria (PNH), atypical hemolytic uremic syndrome (aHUS), C3 glomerulopathy, and age-related macular degeneration. In this study, investigators sequenced the CD55 gene and defined five variations associated with a novel condition designated as CHAPLE syndrome (CD55 deficiency, hyperactivation of complement, angiopathic thrombosis, and protein-losing enteropathy). Based on this data, the researchers demonstrated reduced complement levels in CHAPLE syndrome patients treated with the complement inhibitor eculizumab.
This was a case controlled study that characterized the phenotype and specific genetic variations of patients with a diagnosis of early-onset protein-losing enteropathy and biallelic CD55 mutations. Though the sample size was small, defining the genetics of this rare syndrome provides a better understanding of immune system regulation and opens the door for development of potential targeted therapies.
Click to read the study, published in NEJM
Relevant Reading: Loss of CD55 in eculizumab-responsive protein-losing enteropathy
In-Depth [case control study]: The authors enrolled 11 patients from eight consanguineous families diagnosed with persistent protein-losing enteropathy found to have biallelic loss-of-function mutations in the CD55 gene. They also investigated two deceased family members with similar symptoms. Whole-exome sequencing was performed to define the specific variations in the CD55 gene, and complement assays determined the degree of complement expression produced by patient T-cells. Researchers used the Exome Aggregation Consortium (ExAC) database to screen CD55 genes in over 60 000 unrelated persons without protein-losing enteropathy. Finally, the complement inhibitor eculizumab was incubated with T-cells from patients with CHAPLE syndrome to determine effect on complement production.
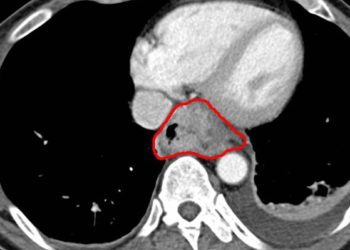
Based on the 11 individuals with defined biallelic loss-of-function mutations in CD55, the most common phenotypic features of CHAPLE syndrome were hypoalbuminemia (10/11), hypogammaglobinemia (11/11), and malabsorption (11/11). Histopathologic assessment of biopsy samples demonstrated variable degrees of lymphangiectasia (5/11), suggesting the diagnosis of primary intestinal lymphangiectasia in a subset of patients. Other characteristics displayed variable expressivity in patients, including bowel inflammation, edema (9/11), thrombotic disease (3/11), recurrent respiratory infections (5/11), and finger clubbing (5/11). Whole-exome sequencing revealed five distinct loss-of-function variants in the CD55 gene. Using the ExAC database, six individuals with early-onset protein-losing enteropathy were found to be homozygous for deleterious mutations in CD55. Of the over 60,000 individuals without protein-losing enteropathy 53 were found heterozygous for CD55 mutations, indicating heterozygous loss-of-function mutations are likely benign. Eculizumab was found to decrease complement production in T-cells of patients with CHAPLE syndrome.
Image: PD
©2017 2 Minute Medicine, Inc. All rights reserved. No works may be reproduced without expressed written consent from 2 Minute Medicine, Inc. Inquire about licensing here. No article should be construed as medical advice and is not intended as such by the authors or by 2 Minute Medicine, Inc.