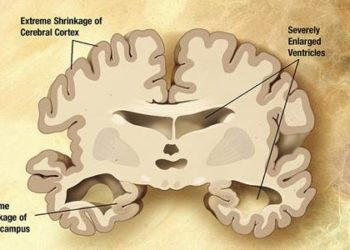
Increased orexin levels linked with poor sleep quality in Alzheimer Disease
1. In Alzheimer disease (AD), increased cerebrospinal fluid (CSF) orexin levels were associated with diminished sleep quality, and increased cognitive decline.
2. CSF orexin levels appeared to be increased in patients with moderate-severe AD, as compared with healthy controls.
Evidence Rating Level: 3 (Average)
Study Rundown: Alzheimer disease (AD) is characterized by progressive loss of memory and executive function. A less discussed symptom of the disease is sleep dysregulation, which can have significant detrimental effects on quality of life. Sleep is also important for maintaining optimal cognition and memory consolidation. Essential to the regulation of sleep-wake cycles is a neurotransmitter called orexin A (or hypocretin 1), which increases arousal and wakefulness. This study recorded CSF orexin levels in 48 patients with AD and 29 age-matched controls, comparing these data points with metrics of sleep health.
Orexin was increased in patients with moderate to severe AD, and correlated with the number of tau proteins in the brain, which are the pathologic hallmarks of the disease. There also was a correlation between degree of cognitive impairment measured by the Mini Mental Status Exam (MMSE) and the severity of sleep dysfunction that patients experienced. The study therefore suggests that changes in the orexigenic system are involved in the pathogenesis of AD and result in these sleep disturbances. However, when all the patients with AD were pooled there was no significant difference in CSF orexin levels between them and controls, nor was there a difference between mild AD patients and the controls.
Click to read the study, published today in JAMA Neurology
Click to read an accompanying editorial in JAMA Neurology
Relevant Reading: Amyloid-β Dynamics are Regulated by Orexin and the Sleep-Wake Cycle
In-Depth [case-control study]: This study was performed in Italy. All subjects underwent history and physicals, neurologic examinations, neuropsychiatric evaluations, electroencephalogram, polysomnography, MRI of the brain, and lumbar puncture. AD patients were divided into two subgroups (mild, and moderate-severe) based on the severity of cognitive impairment measured by the MMSE. Serving as control patients were inpatients without dementia that underwent the above tests for other reason, such as suspected subarachnoid hemorrhage or polyneuropathy. Polysomnography was used to assess sleep quality, and the following variables were studied: time in bed, sleep onset latency, total sleep time, sleep efficiency, rapid eye movement (REM) sleep latency, REM sleep, and wakefulness after sleep onset.
CSF samples obtained by LP were analyzed for levels of amyloid beta1-42, t-tau, p-tau, and orexin. Patients with moderate-severe AD had higher mean orexin levels compared with controls (154.36 [SD 28.16] vs. 131.03 [SD 26.55]; P< 0.01) and worse quality sleep. For AD patients, levels of CSF orexin correlated directly with sleep onset latency (r=0.41; P=0.004) and stage 1 non-REM sleep (r=0.43; P=0.002). Moreover, CSF orexin levels were correlated with decreased sleep efficiency (r=−0.38; P=0.007), stage 3 non-REM sleep (r=−0.32; P=0.027), and REM sleep (r=−0.31; P=0.03). In the total AD cohort, orexin levels were correlated with total tau protein levels (r=0.32; P=0.03). There were no significant differences in orexin levels when comparing all patients with AD and controls.
More from this author: Glatiramer acetate (Copaxone) therapy may alter B cell function in multiple sclerosis, Dementia patients frequently on medications with minimal benefit, Walk test linked to quality of life in multiple sclerosis
Image: PD
©2012-2014 2minutemedicine.com. All rights reserved. No works may be reproduced without expressed written consent from 2minutemedicine.com. Disclaimer: We present factual information directly from peer reviewed medical journals. No post should be construed as medical advice and is not intended as such by the authors, editors, staff or by 2minutemedicine.com. PLEASE SEE A HEALTHCARE PROVIDER IN YOUR AREA IF YOU SEEK MEDICAL ADVICE OF ANY SORT.