Key factors for non-response to ranibizumab in macular degeneration identified
Image: PD
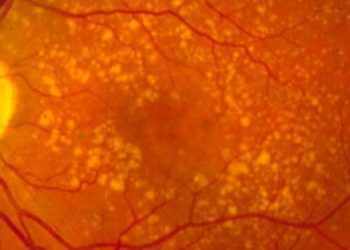
1. Fibrovascular pigment epithelial detachment (PED) and serous PED were associated with non-response to intravitreal ranibizumab treatment as determined by visual acuity testing.
2. Fibrovascular PED and type 1 choroidal neovascularization were associated with non-response as determined by fundus findings.
Evidence Rating Level: 2 (Good)
Study Rundown: For age-related macular degeneration (AMD), intravitreous ranibizumab is an effective treatment option for many patients. A small subset of patients however, do not respond to this treatment. In this study, patients with AMD were reviewed to identify and characterize non-responders to intravitreal ranibizumab treatment. The authors found that several factors were associated with non-response to the anti-VEGF treatment as determined by best-corrected visual acuity (BCVA) and fundus findings. These factors include initial fibrovascular pigment epithelial detachment (PED), serous PED, and type 1 choroidal neovascularization. An important strength of this study is a large patient sample size. Limitations in this study include the retrospective study design, which makes it difficult to establish a causal relationship, as well as the large 95% confidence intervals. Nonetheless, this study suggests that ophthalmologists should be aware of these potential predictive factors when treating AMD patients with intravitreal ranibizumab.
Click to read the study in British Journal of Ophthalmology
Relevant Reading: Intravitreal ranibizumab for neovascular age-related macular degeneration patients with good baseline visual acuity and the predictive factors for visual outcomes
In-Depth [retrospective cohort]: This study retrospectively reviewed the clinical records of 141 eyes in 141 AMD patients. All patients received a monthly intravitreal injection of ranibizumab for 3 months followed by PRN intravitreal injections for 9 months. Non-responders to the anti-VEGF treatment were defined as patients with worsened BCVA, increased exudative fundus findings and/or an increased central retinal thickness at 12 months. Logistic regression models were created to analyze non-responders’ initial characteristics. Initial fibrovascular PED (OR=22.9, 95%CI=2.61-201) and serous PED (OR=4.12, 95%CI=1.08-15.8) were associated with non-response to ranibizumab treatment as determined by BCVA. Initial fibrovascular PED (OR=33.5, 95%CI=2.95-381) and type 1 choroidal neovascularization (OR=6.46, 95%CI=1.39-30.0) were associated with non-response as determined by fundus findings.
©2012-2014 2minutemedicine.com. All rights reserved. No works may be reproduced without expressed written consent from 2minutemedicine.com. Disclaimer: We present factual information directly from peer reviewed medical journals. No post should be construed as medical advice and is not intended as such by the authors, editors, staff or by 2minutemedicine.com. PLEASE SEE A HEALTHCARE PROVIDER IN YOUR AREA IF YOU SEEK MEDICAL ADVICE OF ANY SORT.