Low-dose aspirin reduces incidence of preterm preeclampsia in high-risk pregnancies: The ASPRE trial
1. Low-dose aspirin significantly reduced the incidence of preterm preeclampsia in women identified as high-risk for preeclampsia using a screening protocol that combined maternal factors with biochemical measurements at 11-13 weeks of gestation.
2. No significant differences in adverse outcomes were found in women given low-dose aspirin compared to placebo.
Evidence Rating Level: 1 (Excellent)
Study Rundown: Preeclampsia is a morbid condition of pregnancy which can lead to preterm birth. Prior research has shown aspirin to be associated with lower incidence of preeclampsia in some study populations, leading to low-dose aspirin now being standard of care for high-risk pregnancies, though early identification of such pregnancies remains a challenge. The Combined Multimarker Screening and Randomized Patient Treatment with Aspirin for Evidenced-Based Preeclampsia Prevention (ASPRE) trial examined whether prophylactic low-dose aspirin starting near the end of the first-trimester reduced the risk of preeclampsia in women identified as high-risk based on a priori maternal factors and biochemical measurements assessed at 11 to 13 weeks of gestation. The primary endpoint, delivery with preeclampsia before 37 weeks of gestation, was significantly reduced in high-risk women taking low-dose aspirin compared to those treated with placebo. No significant differences in secondary endpoints identifying adverse outcomes, such as death and neonatal complications, neonatal therapy, and poor fetal growth at various times during gestation, were demonstrated between study groups. This study indicates the benefit of low-dose aspirin in women determined to be at high-risk of preeclampsia in reducing incidence of preeclampsia.
This is a large, double-blind, randomized, multicenter trial examining the prophylactic use of aspirin in a cohort of women screened for preterm preeclampsia. The multi-metric screening approach helped overcome the current obstetric challenge of identifying women at high risk for preterm preeclampsia. Screening and aspirin treatment were performed and begun, respectively, near the end of the first-trimester, which allowed for the maximum benefit of aspirin as suggested by prior studies. Limitations include the lack of follow-up past the early postnatal phase.
Click to read the study, published in NEJM
Relevant Reading: Primary, secondary, and tertiary prevention of pre-eclampsia
In-Depth [randomized controlled trial]: This double-blind trial screened 26 941 women with singleton pregnancies, and 2971 (11.0%) were determined to be at high risk for preterm preeclampsia. Of these woman, 1776 were eligible for the study and randomized in a 1:1 ratio to groups receiving 150 mg aspirin (n = 798; 78 withdrew and 2 lost to follow-up) or placebo (n = 822; 72 withdrew and 2 lost to follow-up). Inclusion criteria were age of 18 years or more, singleton pregnancy, live fetus at 11-13 weeks of gestation, and being high-risk (>1 in 100) for preterm preeclampsia. The screening test for preeclampsia risk combined maternal factors, mean arterial pressure, uterine-artery pulsatility index, maternal serum pregnancy-associated plasma protein A, and placental growth factor measured at 11-13 weeks of gestation. The primary outcome was delivery with preeclampsia before 37 weeks of gestation. Secondary outcomes included multiple adverse events of pregnancy before 34 weeks, before 37 weeks, and at or after 37 weeks of gestation, including stillbirth or neonatal death, neonatal complications or therapy, and poor fetal growth.
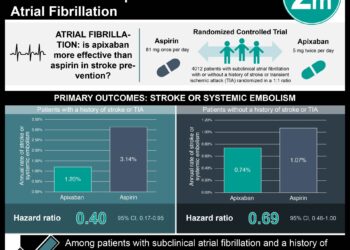
Preterm preeclampsia occurred in 13 of 798 women (1.6%) in the aspirin group and 35 of 822 (4.3%) of women in the placebo group (odds ratio [OR] of aspirin group, 0.38; 95% confidence interval [CI], 0.20-0.74; p = 0.004). No significant differences were found among any of the secondary outcomes, including adverse outcomes before 34 weeks (OR, 0.62; 95% CI, 0.34-1.14), before 37 weeks (OR, 0.69; 95% CI, 0.46-1.03), or equal to or after 37 weeks of gestation (OR, 1.12; 95% CI, 0.82-1.54). In the aspirin group, serious or any adverse event occurred in 13 (1.6%) and 207 (25.9%) of women, respectively, compared to 26 (3.2%) and 210 (25.5%) of those in the placebo group.
Image: PD
©2017 2 Minute Medicine, Inc. All rights reserved. No works may be reproduced without expressed written consent from 2 Minute Medicine, Inc. Inquire about licensing here. No article should be construed as medical advice and is not intended as such by the authors or by 2 Minute Medicine, Inc




![Nanoparticle delivery of aurora kinase inhibitor may improve tumor treatment [PreClinical]](https://www.2minutemedicine.com/wp-content/uploads/2016/02/20541_lores-75x75.jpg)
