Pasireotide effective in reducing postoperative pancreatic surgery complications
Image: PD
1. Pasireotide was effective at reducing the rate of post-pancreatectomy fistulas, leaks and abscesses until 60 days post-op.
Evidence Rating Level: 1 (Excellent)
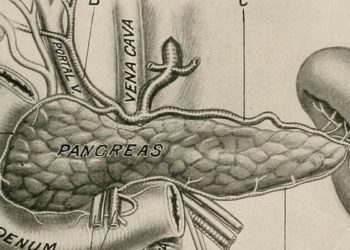
Study Rundown: Postoperative morbidity such as fistulas, leaks and abscesses are common complications after pancreatectomy, affecting 30-50% of patients. Exocrine secretion from remnant pancreatic tissue is thought to contribute towards the development of fistulas and subsequent complications. Somatostain analogues (ie. octreotide) have been used to reduce these secretions.
This phase 3, single-center, randomized, double-blind study evaluated a new somatostatin analogue, pasireotide. Earlier studies have shown that pasireotide has a longer half-life as well as a broader receptor binding profile to somatostatin receptors when compared with octreotide.
In this study, pasireotide achieved the primary endpoint of successfully reducing the rates of fistulas, leaks and abscesses at 60 days post-op. While both pasireotide and placebo groups were well-matched for baseline characteristics, more patients in the pasireotide group did not finish the full course of treatment, thus treatment duration remains unknown. Further limitations include the short follow up time in this study in order to comment on whether the benefits of pasireotide are preserved. Nevertheless, the results of this study show a promising pre- and post-operatively role for pasireotide and future studies will provide more information regarding its long-term safety profile.
Click to read the study, published today in NEJM
Relevant Reading: A Meta-analysis of Outcomes Following Use of Somatostatin and Its Analogues for the Management of Enterocutaneous Fistulas
In-Depth [randomized controlled trial]: This study randomized 300 patients undergoing pancreatectomy (for various indications) into two groups: 900mcg of pasireotide versus placebo given subcutaneously twice daily for 7 days starting on the day of the surgery. The baseline and operative characteristics of both groups were well-matched, however, there was a statistical difference in the number of patients who received all 14 doses (pasireotide v. placebo, 75.7% v. 86.5%, p=0.02) and readmission (pasireotide v. placebo, 17.1% v. 29.1%, p=0.02). The primary endpoint of postoperative fistulas, leaks and abscesses (which required draining) at day 60 was 9.2% versus 20.9%, pasireotide versus placebo respectively (p=0.006). Primary endpoint was also lower for all pasireotide-treated patients in subgroup analysis based on procedure type (pancreaticoduodenectomy, distal pancreatectomy) and technique (dilated duct, nondilated duct). Furthermore, post-hoc analysis demonstrated that patients with surgical drains had a higher risk of reaching the primary end point (drain v. no drain, 25% v. 11%, p=0.003) but the benefits of pasireotide was still preserved in the subgroup of patients with surgical drains (pasireotide v. placebo, 9% v. 44%, p<0.001). Severe adverse events in the pasireotide group included hyperglycemia (50.0%) and nausea/vomiting (2.7%).
More from this author: Idelalisib plus rituximab improves progression-free survival in relapsed CLL, SSRI use during pregnancy not linked to increased risk of autism,Combo antifungal therapy most effective treatment for cryptococcal meningitis
©2012-2014 2minutemedicine.com. All rights reserved. No works may be reproduced without expressed written consent from 2minutemedicine.com. Disclaimer: We present factual information directly from peer reviewed medical journals. No post should be construed as medical advice and is not intended as such by the authors, editors, staff or by 2minutemedicine.com. PLEASE SEE A HEALTHCARE PROVIDER IN YOUR AREA IF YOU SEEK MEDICAL ADVICE OF ANY SORT.