Patient Basics: Cardiac Catheterization
Originally published by Harvard Health.
What Is It?
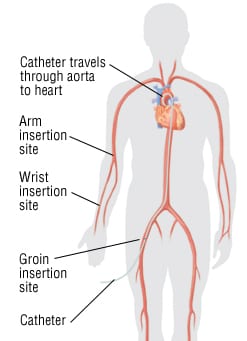
Cardiac catheterization is a procedure in which a heart specialist inserts a small tube (catheter) through a large blood vessel in the arm or leg, and then passes the tube into the heart. Once inside the heart, doctors use the catheter to evaluate how the heart is working by measuring pressure and oxygen levels within the heart’s chambers. Through the catheter, doctors inject a special dye that provides an X-ray image of the heart’s internal structure and blood flow patterns.
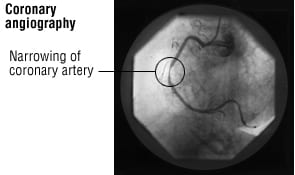
The procedure is often done to look for narrowed and blocked coronary arteries. The X-ray dye also is injected into each of the three largest coronary arteries. This is called coronary angiography.
What It’s Used For
Cardiac catheterization is used to evaluate patients who:
- May have suspected coronary artery disease
- Are having a heart attack or in immediate danger of having a heart attack
- Will be undergoing heart surgery, especially coronary artery bypass surgery
- Have heart valve problems, including abnormal narrowing (stenosis), leakage (insufficiency), or significant backflow of blood through a valve (regurgitation)
- May have cardiomyopathy (heart muscle damage causing symptoms of heart failure)
Heart specialists can use heart catheters to carry special instruments into the heart. These instruments can open narrowed and blocked coronary arteries (a procedure called coronary angioplasty) or correct certain congenital (inborn) heart defects in children.
Preparation
Before the procedure, the doctor will review your medical history, your current medications, and your allergy history. If you know you are allergic to X-ray dye, tell your doctor. He or she may need to use a newer X-ray dye that is less likely to trigger allergies, or give you medication to reduce the likelihood of an allergic reaction. Also, if there is any chance that you may be pregnant, tell the doctor before your cardiac catheterization.
Leave bracelets, necklaces and watches at home. Someone will have to drive you home from the hospital, so make arrangements beforehand. Follow your doctor’s instructions for when to stop eating and drinking before your catheterization.
How It’s Done
A nurse or aide will clean and shave the area of your arm or leg where the catheter will be inserted. You will lie on a flat table under a large X-ray machine. Several electrocardiogram (EKG) electrodes (small metal disks) will be put on your arms and legs. You will get medication will help you to relax. An intravenous (IV) line will be inserted into a vein in your arm to deliver fluids and medications.
After the catheter site is cleaned with antiseptic solution, the doctor will numb your skin and then make a small cut to reach a large blood vessel under the skin surface. The doctor inserts the catheter into the blood vessel and moves it through your circulatory system toward the heart. By using X-rays, the doctor can watch the catheter’s progress on a nearby monitor. Once the catheter is in your heart, it will measure pressures inside the heart, take blood samples, inject X-ray dye, or perform other functions.
After all the tests are finished, the catheter will be removed, and the insertion site will be closed with stitches. A special pressure dressing may be applied. You will have to stay in bed for six to eight hours with your arm or leg extended while a nurse monitors your vital signs and checks for bleeding at the catheter site. The nurse will also monitor the pulse, color and temperature of the arm or leg in which the catheter was inserted.
When you have recovered enough, you will be able to go home. Your doctor will tell you when you can start eating and drinking again.
Follow-Up
After your heart catheterization, you will need to avoid strenuous activity for at least 24 to 48 hours. Within five to seven days, you will return to your doctor’s office for a checkup.
Risks
Although heart catheterization is generally a safe procedure, there is some risk of the following complications:
- Heart attack or stroke
- Abnormal heartbeat (cardiac arrhythmia)
- Puncture of a blood vessel or of the heart
- Bleeding, blood clot, or infection at the catheter insertion site
- A blocked blood vessel in the arm or leg in which the catheter was inserted
- An allergic reaction to the X-ray dye
Because some of these problems may be life threatening, heart catheterization should always be done in a hospital that has the necessary equipment and personnel to deal with any complications immediately.
Certain patients have a higher-than-average risk of complications. These include infants younger than 1 month, people older than 80 years, people with very poor heart function, and people with certain chronic illnesses, such as kidney failure, insulin-dependent diabetes, and severe lung disease.
When To Call A Professional
Call your doctor immediately if the catheter insertion site becomes swollen, painful and red or if it oozes blood. Also call your doctor immediately if the arm or leg in which the catheter was inserted becomes painful, cold and pale, with a weak or absent pulse.
Additional Info
American Heart Association (AHA)
7272 Greenville Ave.
Dallas, TX 75231
Toll-Free: (800) 242-8721
Fax: (214) 706-2139
http://www.americanheart.org/
National Heart, Lung and Blood Institute (NHLBI)
6701 Rockledge Dr.
P.O. Box 30105
Bethesda, MD 20824-0105
Phone: (301) 592-8573
http://www.nhlbi.nih.gov/