Patient Basics: Uterine Cancer
Originally published by Harvard Health.
What Is It?
Uterine cancer is the most common cancer of the female reproductive tract. There are two main types: endometrial cancer and uterine sarcoma.
Endometrial cancer is the most common type of uterine cancer. It occurs in the inner lining of the uterus, called the endometrium. The disease generally strikes women between the ages of 50 and 65. Its cause is not fully understood.
However, women who have high levels of the hormone estrogen that are not offset by the hormone progesterone are more likely to develop endometrial cancer. Since progesterone levels drop after menopause, postmenopausal women have a higher-than-normal risk of developing this cancer. Other women likely to have high levels of estrogen without enough progesterone include those who
- are obese
- have a history of infertility
- take long-term estrogen therapy.
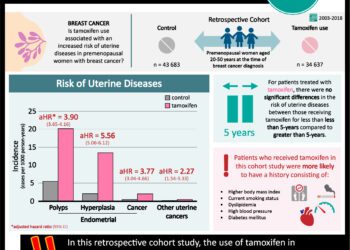
Other women who may also be at high risk of endometrial cancer include those with high blood pressure and diabetes, and women who take tamoxifen (Nolvadex) for the treatment of breast cancer.
Uterine sarcoma starts in the muscle and fibrous tissue that form the uterine wall. This cancer is rare. While its cause is unknown, uterine sarcoma occurs most often in middle-aged and elderly women. African American women and women who have had pelvic radiation to treat other cancers may be more likely to develop this cancer. Doctors aren’t sure why.
Symptoms
Nearly all women with uterine cancer experienced abnormal vaginal bleeding before the disease was diagnosed. For younger women, abnormal bleeding may include
- periods that are heavier than usual
- spotting (bleeding between periods)
- bleeding after sex.
For older women, bleeding that happens at the start of menopause or after it should be reported to a doctor. Don’t assume that abnormal bleeding is a normal part of menopause.
Other symptoms include painful or difficult urination and pain during sex.
A small percentage of women with uterine sarcoma feel pain before diagnosis. Some can feel a mass in their vagina.
Diagnosis
If you have signs and symptoms of uterine cancer, you should see a gynecologist. This specialist will ask about your medical history. He or she will then do a pelvic exam, which may include a Pap test. This test involves taking some cells from the cervix and upper vagina. However, it can’t detect uterine cancer unless it has spread outside the uterus.
Your doctor may also take a sample of endometrial tissue for testing. During this procedure, called an endometrial biopsy, your doctor inserts a very thin tube into the uterus through the cervix. A small bit of tissue can be removed through this tube. You may feel some cramps during this procedure. Afterward, the tissue sample will be checked for cancerous cells.
If the biopsy doesn’t result in a clear diagnosis, your doctor may perform dilation and curettage (D & C). During this outpatient procedure, the cervix is dilated (widened) and tissue is scraped from inside the uterus. Your doctor may also use a special instrument to view the inside of your uterus. You will be given general anesthesia or sedated during the procedure. Afterward, you will probably have some bleeding for a few days. However, few women complain of serious discomfort.
Imaging tests also may be used to look for uterine cancer. During a transvaginal sonogram, the doctor inserts a probe into the vagina. The probe emits sound waves that bounce off uterine tissue, creating pictures that help doctors locate cancer. During one type of transvaginal sonogram, saline put into the uterus through a catheter (tube) can help outline any problems.
If you are diagnosed with uterine cancer, your doctor will probably refer you to a gynecologic oncologist. This specialist is expert in treating cancers of the female reproductive system. The next step is to determine if, and how far, the cancer has spread. Blood tests usually are ordered along with other imaging tests, such as a computed tomography (CT) scan and a chest x-ray.
Expected Duration
The extent of the cancer determines its stage. The earlier the stage, the more likely a patient is to survive. Uterine cancer has four stages:
- Stage I. The cancer is limited to the uterus.
- Stage II. The cancer has spread from the uterus to the cervix.
- Stage III. The cancer has spread beyond the uterus but is still confined to pelvis.
- Stage IV. The cancer has spread to the bladder or rectum. This stage may also indicate that the cancer has moved into the lymph nodes in the groin, or into distant organs, such as the lungs.
Prevention
Because experts don’t know what causes uterine cancer, there are no clear guidelines for preventing it. However, doctors recommend a healthy diet and exercise to help control weight and blood pressure.
Women who use oral contraceptives (birth control pills) have a lower risk of developing uterine cancer. While this is an added benefit for women who take birth control pills, oral contraceptives are not prescribed solely for cancer prevention.
If you are undergoing estrogen replacement therapy, ask your doctor about taking it with progesterone. Also, ask how often you should have a pelvic exam.
Treatment
If you have uterine cancer, you will most likely have some form of surgery. The procedure your doctor chooses depends on the stage, type, and grade of the cancer. Your general health may also be a factor. Surgical complications are rare.
The most common surgery involves removing the uterus, ovaries, and fallopian tubes. Because these are reproductive organs, you will not be able to get pregnant after surgery. Your doctor may also remove nearby lymph nodes to see if they contain cancer. If cancer cells are in the lymph nodes, the disease may have spread to other parts of the body.
Some women, such as those who cannot have surgery, will have radiation. But women who have surgery may also have radiation.
Radiation is sometimes given before surgery if the cancer is very large. Radiation can shrink the size of the cancer to make it easier for the surgeon to remove the cancer.
In other cases, radiation does not start until after surgery to kill any cancer cells that might remain.
Two types of radiation therapy are used to treat uterine cancer. During external beam radiation, focused beams of radiation are aimed at the tumor from outside the body. Radiation is usually given five days a week for several weeks.
In some cases, a type of radiation called brachytherapy will be used. During this therapy, a doctor inserts a pellet of radioactive material in your body, near the tumor. The pellet is left in place for a few days and then removed.
Both types of radiation can cause side effects. These include
- fatigue
- skin irritation
- burning during urination
- diarrhea.
Most side effects go away after treatment ends.
If the cancer has spread beyond the uterus, your doctor may recommend chemotherapy. Chemotherapy is the use of drugs to kill cancer cells. You may take the drugs by mouth, or they may be injected into a vein.
Hormone therapy using progesterone is a possible treatment option for women who
- are unable to have surgery or radiation therapy
- have uterine cancer that has spread to distant organs, such as the lungs
- have cancer come back following treatment.
Progesterone is most effective when the cancer tissue tests positive for certain proteins on the surface of the cancer cells. These proteins are progesterone receptors.
When To Call a Professional
Call a doctor immediately if you have abnormal vaginal bleeding. You also should consult a doctor if you have pelvic pain or pain during urination or sex. Uterine cancer usually is not the cause of these symptoms.
Prognosis
The earlier the cancer is treated, the better the outlook. In general, more than three-quarters of women with uterine cancer live five years or longer. Even if the cancer is treated successfully, it can come back. Be sure to keep follow-up appointments with your doctor.
Additional Information
American Cancer Society (ACS)
1599 Clifton Road, NE
Atlanta, GA 30329-4251
Toll-Free: 1-800-227-2345
http://www.cancer.org/
National Cancer Institute (NCI)
U.S. National Institutes of Health
Public Inquiries Office
Building 31, Room 10A03
31 Center Drive, MSC 8322
Bethesda, MD 20892-2580
Phone: 301-435-3848
Toll-Free: 1-800-422-6237
http://www.nci.nih.gov/
National Women’s Health Information Center (NWHIC)
8550 Arlington Blvd.
Suite 300
Fairfax, VA 22031
Toll-Free: 1-800-994-9662
TTY: 1-888-220-5446
http://www.4woman.org/
Society for Women’s Health Research
1025 Connecticut Ave., NW
Suite 701
Washington, DC 20036
Phone: 202-223-8224
Fax: 202-833-3472
http://www.womenshealthresearch.org/