Pembrolizumab plus concurrent chemoradiation therapy associated with robust antitumor activity in patients with locally advanced, unresectable, stage III non-small cell lung cancer
1. Concomitant pembrolizumab plus chemoradiation therapy was associated with improved antitumor activity and safety profile in patients with previously untreated, locally advanced, stage III non-small cell lung cancer.
2. This treatment regimen represents a promising therapy in patients with previously untreated, locally advanced, stage III non-small cell lung cancer, regardless of tumor histologic type and molecular immunogenic marker characteristics.
Evidence Rating Level: 2 (Good)
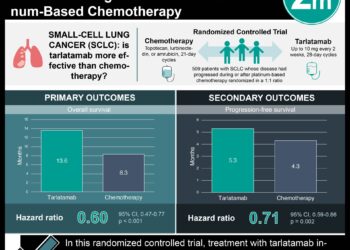
Study Rundown: In patients diagnosed with non-small cell lung cancer (NSCLC), approximately 25% will present with tumor stages IIIA to IIIC, a majority of which are surgically unresectable and treated using platinum-doublet chemotherapy concurrent with radiotherapy (cCRT). However, patients who begin cCRT often experience disease progression (PD) or toxic side effects and become unable to complete the prescribed course of cCRT. Furthermore, this substantial patient population (up to 30%) usually does not meet the criteria for consolidative therapy via newer monoclonal antibody treatments against programmed cell death ligand 1 (PD-L1) such as durvalumab. However, it has been hypothesized that the initial administration of concurrent anti-programmed cell death 1 (PD-1) therapy and cCRT could provide therapeutic benefits to a greater proportion of patients with locally advanced, unresectable, stage III NSCLC. In this case, the use of pembrolizumab has been proposed – a highly selective humanized monoclonal anti-PD-1 antibody that has demonstrated long-term survival and durable clinical benefit as first-line treatment in stage III NSCLC. The phase 2 KEYNOTE-799 study was designed as a 2-cohort nonrandomized, international study in order to evaluate treatment outcomes and safety of pembrolizumab plus cCRT in stage III NSCLC. In this study, coprimary end points were objective response rate per Response Evaluation Criteria in Solid Tumors (RECIST v1.1) via blinded independent central review and incidence of grade 3 to 5 pneumonitis. Among 216 eligible patients, pembrolizumab plus cCRT demonstrated objective response rates of 70.5% in cohort A (n = 112; squamous or nonsquamous) and 70.6% in cohort B (n = 102; nonsquamous). In addition, the incidence of grade 3 or higher pneumonitis in cohorts A and B were 8.0% and 6.9% respectively. These findings demonstrate that concomitant pembrolizumab plus cCRT produced robust antitumor activity, regardless of tumor histologic type and PD-L1 tumor proportion score (TPS), with manageable safety and toxicity profiles. Thus, this treatment regimen represents a promising therapy in patients with previously untreated, locally advanced, stage III NSCLC. A limitation of this study was that follow-up duration in cohort B was limited as many patients were still receiving study therapy. In general, longer follow-up will provide further information on the outcomes of overall survival and progression-free survival following study treatment.
Click to read the study in JAMA Oncology
In-Depth [prospective cohort]: This phase 2, multicenter, nonrandomized, open-label KEYNOTE-799 study enrolled patients between November 2018 and July 2020, from 52 academic facilities and community-based institutions across 10 countries. As of October 28, 2020, median (range) follow-up in cohorts A and B were 18.5 (13.6-23.8) months and 13.7 (2.9-23.5) months. Using the inclusion/exclusion criteria, 301 patients were screened, of which 216 eligible patients with previously untreated, unresectable, and pathologically/radiologically confirmed stage III NSCLC with measurable disease were enrolled in the study. In cohort A (squamous or nonsquamous; n = 112; 76 men [67.9%]; median [range] age, 66.0 [46-90] years; 66 patients [58.9%] with PD-L1 TPS ≥1%), patients received a three-week cycle of carboplatin, paclitaxel, and pembrolizumab, followed by carboplatin and paclitaxel once weekly for 6 weeks and 2 cycles of pembrolizumab plus standard thoracic radiotherapy. In cohort B (nonsquamous; n = 102; 62 men [60.8%]; median [range] age, 64.0 [35-81] years; 40 patients [39.2%] with PD-L1 TPS ≥1%), patients received 3 cycles of cisplatin, pemetrexed, and pembrolizumab every 3 weeks and thoracic radiotherapy in cycles 2 and 3. After cCRT, all patients received an additional 14 cycles of pembrolizumab every 3 weeks, for a total of 17 cycles (approximately 1 year). Overall, objective response rate in cohorts A and B were 70.5% (79/112; 95%CI, 61.2%-78.8%) and 70.6% (72/102; 95%CI, 60.7%-79.2%) respectively. Although the median duration of response was not reached in either cohort, 79.7% and 75.6% in cohorts A and B respectively, had a response duration of 12 months or longer. Lastly, grade 3 or higher pneumonitis occurred in 9 of 112 patients (8.0%) in cohort A and 7 of 102 (6.9%) in cohort B while grade 3 to 5 treatment-related adverse events occurred in 72 of 112 (64.3%) and 51 of 102 (50.0%) patients, respectively.
Image: PD
©2021 2 Minute Medicine, Inc. All rights reserved. No works may be reproduced without expressed written consent from 2 Minute Medicine, Inc. Inquire about licensing here. No article should be construed as medical advice and is not intended as such by the authors or by 2 Minute Medicine, Inc.





![Oral amoxicillin as effective as injectable benzylpenicillin-gentamicin for infants with infection in which referral not possible [AFRINEST Trial]](https://www.2minutemedicine.com/wp-content/uploads/2015/04/NOVAMOXIN_antibiotic-75x75.jpg)