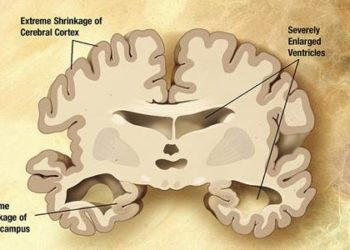
Periodontal disease associated with increased rate of cognitive decline in Alzheimer’s dementia
1. In a prospective cohort study of 60 adults with Alzheimer’s dementia, the presence of periodontitis was associated with a significant increase in the rate of cognitive decline compared to controls.
Evidence Rating Level: 2 (Good)
Study Rundown: Periodontitis is a disease characterized by gingival inflammation and is a major cause of tooth loss, particularly among the elderly population. Previous studies have demonstrated increasing prevalence of periodontitis in patients with Alzheimer’s disease due to the reduced ability to maintain proper oral hygiene. However, there has been no studies to date to analyze the potential pro-inflammatory effect of periodontitis on the natural history of Alzheimer’s dementia. The purpose of this prospective trial is to clarify this potential association.
The study prospectively followed 60 adults with Alzheimer’s dementia for six months and evaluated each patient for the presence of periodontitis, serum pro-inflammatory markers, and cognitive status. At the conclusion of the study, patients with baseline periodontitis is associated with a six-fold increase in the rate of cognitive decline compared to patients without periodontitis. This association was independent to baseline cognitive status of the participants. Additionally, patients with periodontitis demonstrated a trend towards higher serum levels of pro-inflammatory cytokines and reductions in anti-inflammatory cytokines compared to controls. The results of this study support the hypothesis that periodontitis may worsen cognitive decline in adults with Alzheimer’s dementia through a pro-inflammatory mechanism. However, the study is limited by the small sample size and lack of control of other important confounding variables such as compromised immune response leading to both worsening cognitive function and periodontitis. Additional large, prospective trials are needed to confirm this association.
Click to read the study in PLOS One
Relevant Reading: Alzheimer’s disease and peripheral infections: the possible contribution from periodontal infections, model and hypothesis
In-Depth [prospective cohort]: The study prospective recruited sixty participants with Alzheimer’s dementia with mild to moderate cognitive decline from the community in the United Kingdom. Each patient was assessed for dental health, cognitive function, and serum inflammatory biomarkers at baseline. Dental health was assessed by a trained dental hygienist and periodontitis was determine according to the Centre for Disease Control/American Academy of Periodontology (CDC/AAP) case definitions. Cognitive status was evaluated by the Alzheimer’s disease Assessment Scale (ADAS-cog). Inflammatory cytokine biomarkers, including serum C-reactive protein (CRP), tumor necrosis factor-alpha (TNF-α, and interleukin-10 (IL10), were collected following cognitive evaluation. After a six month follow-up period, patients who had periodontitis at baseline demonstrated a six-fold difference in change in cognitive decline compared to patients without periodontitis as determined by ADAS-cog (mean difference: 5.2; 95% CI: 1.7 to 8.8; p = 0.005). There was a trend in the patient group with periodontitis for increased serum CRP (p = 0.08) and decreased serum IL10 (p = 0.047).
Image: PD
©2015 2 Minute Medicine, Inc. All rights reserved. No works may be reproduced without expressed written consent from 2 Minute Medicine, Inc. Inquire about licensing here. No article should be construed as medical advice and is not intended as such by the authors or by 2 Minute Medicine, Inc.