Proton pump inhibitor use associated with development of chronic kidney disease
1. Amongst two prospective cohorts, use of proton pump inhibitors (PPIs) was associated with a 20 – 50% higher risk of developing chronic kidney disease (CKD). This same risk was not present with the use of H2-antagonists, which are prescribed for the same indications as PPIs.
2. Given the high prevalence of PPI use, often without an indication or for longer than indicated, this association has important implications given the morbidity and mortality related to CKD.
Evidence Rating Level: 2 (Good)
Study Rundown: Chronic kidney disease (CKD) leads to significant morbidity and mortality amongst the American population, and is a major economic burden. While co-morbid conditions such as diabetes and hypertension are known to cause and exacerbate CKD, polypharmacy has also been implicated. Proton pump inhibitors (PPIs), which are one of the most prescribed medications, often without a strong indication, have been linked to acute kidney injury (AKI). The theory is that recurrent bouts of AKI may lead to CKD. This study, which used data from two prospective cohorts, was conducted to evaluate the link between PPIs and incident CKD. The results of the study showed that use of proton pump inhibitors (PPIs) was associated with about 20 – 50% higher risk of developing chronic kidney disease (CKD). This same risk was not present with the use of H2-antagonists, which are prescribed for the same indications as PPIs.
The strength of this study was the use of two prospective cohorts to evaluate the relationship between PPIs and CKD, which strengthens the validity of the results. Drawbacks are the observational nature of the study, which has inherent problems with assigning causality. Also, one of the cohorts uses ICD9 codes to identify CKD, which may have led to misdiagnosis.
Click to read the study, published today in JAMA Internal Medicine
Relevant Reading: Proton pump inhibitors and the risk of acute kidney injury in older patients: a population-based cohort study
In-Depth [prospective cohort]: The purpose of this study was to evaluate a possible link between use of PPIs and development of CKD. This study comprised of two prospective cohorts: Atherosclerosis Risk in Communities (ARIC) cohort and Geisinger Health System cohort. The former was a population-based cohort from four states, and the latter was a cohort from a rural health care system. In addition to demographic and co-morbid characteristics, the study characteristics were use of PPIs (and H2-antagonists as a comparator) and incident CKD, based on health care documentation.
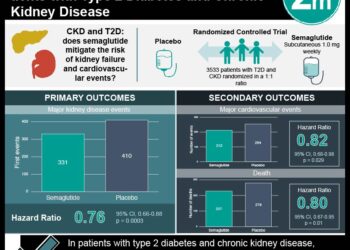
The study showed that in the ARIC cohort, after adjustment of potential confounders, users of PPI had a higher risk of incident CKD compared to non-users of PPIs (HR 1.50; 95% CI, 1.14 – 1.96). A similar finding was present in the Geisinger cohort (HR 1.17; 95% CI, 1.12 – 1.23). The risk developing AKI was even higher amongst patients using PPIs in the ARIC (HR 1.64; 95% CI, 1.22 – 2.21) and the Geisinger cohort (HR 1.31; 95% CI, 1.22 – 1.42). When comparing PPI use to H2-antagonist use, the former was associated with a higher risk of developing CKD in both the ARIC cohort (HR 1.39; 95% CI, 1.01 – 1.91) and the Geisinger cohort (HR 1.29; 95% CI, 1.19 – 1.4). The use of H2-antagonists was not associated with developing CKD.
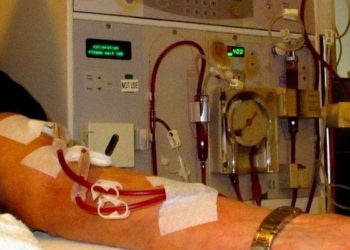
Image: CC/Wiki/Nephron
©2015 2 Minute Medicine, Inc. All rights reserved. No works may be reproduced without expressed written consent from 2 Minute Medicine, Inc. Inquire about licensing here. No article should be construed as medical advice and is not intended as such by the authors or by 2 Minute Medicine, Inc.