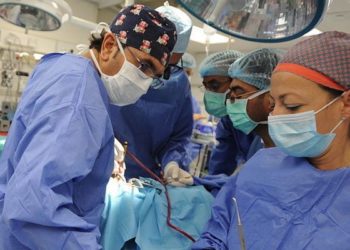
Single-site robotic cholecystectomy is safe, but technically challenging
Image: CC/Wiki
1. 87 of 95 patients completed single-site robotic cholecystectomy without conversion to traditional approaches.
2. Following single-site robotic cholecystectomy, 11.6% of patients required hospital admission and 6.3% required readmission.
3. 24% of patients suffered cholecystotomy during dissection, but without any measurable sequelae.
Evidence Rating Level: 2 (Good)
Study Rundown: This study demonstrated the feasibility and comparable safety profile seen with single-site robotic cholecystectomy (SSRC) versus traditional laparoscopic cholecystectomy. It functions as a proof of concept study and does not endorse claims of superiority of the procedure. The enrollment of a diverse patient population including many obese patients enhanced the authors’ argument that this procedure can be done effectively in just about any patient. Although single-site operation has the advantage of leaving behind only one scar, this benefit must be weighed against risks such as the increased rate of cholecystostomy which was reported at 24%. This study was limited by the lack of direct comparison with laparoscopic cholecystectomy outcomes as control data. The generalizability of these findings may also be limited by the particular experience of the authors with the da Vinci surgical system, which is only available at select institutions. Larger, multi-institution studies are needed to more effectively rule out confounding variables. Nonetheless, this study showed that the procedure can be done effectively in a broad patient population, including those with obesity or prior abdominal procedures.
Click to read the study in the Annals of Surgery
Relevant Reading: Systematic review and meta-analysis of randomized clinical trials comparing single-incision versus conventional laparoscopic cholecystectomy
In-Depth [prospective cohort study]: This prospective cohort study, carried out in one institution using the single-site da Vinci surgical platform to complete the procedures, included all patients requiring cholecystectomy that consented to participate in the trial. To fully measure the capabilities of this surgical platform across all patients, no exclusion critiera were used which contrasts prior studies. Of the 95 patients who participated in the trial, 87 completed their cholecystectomies through the single incision, 6 were converted to laparoscopic, 1 converted to open, and 1 case was aborted out of concern that the patient had cancer. The average operative time for the single-site procedure was 83.5 minutes (49-198 minutes). 43% of those patients were obese. While the total operative time decreased with experience, the only component of the procedure with a statistically significant drop in time was the setup time (P = 0.02). The presence of intra-abdominal adhesions significantly increased robotic time (47.1 vs. 37.5, P = 0.01) as did elevated BMI(P = 0.03). During the procedure, 24% of patients suffered a cholecystostomy, however no deaths or other measurable sequellae resulted. Although the standard protocol was to discharge patients home post-operatively, 11.6% required admission, and 6.3% of patients were readmitted to the hospital.
By David Mattos and Chaz Carrier
© 2013 2minutemedicine.com. All rights reserved. No works may be reproduced without written consent from 2minutemedicine.com. Disclaimer: We present factual information directly from peer reviewed medical journals. No post should be construed as medical advice and is not intended as such by the authors or by 2minutemedicine.com. PLEASE SEE A HEALTHCARE PROVIDER IN YOUR AREA IF YOU SEEK MEDICAL ADVICE OF ANY SORT. Content is produced in accordance with fair use copyrights solely and strictly for the purpose of teaching, news and criticism. No benefit, monetary or otherwise, is realized by any participants or the owner of this domain.