Teen asthma controller medication adherence affected by risk tolerance
[tabs tab1=”2MM Rundown” tab2= “2MM Full Report”]
[tab]
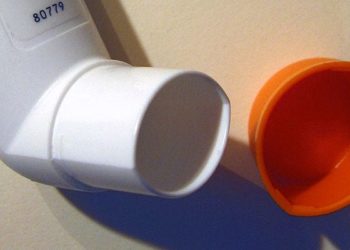
Image: PD
1. Teens with persistent asthma symptoms and a high risk tolerance have low controller medication adherence.
2. Those with a preference for immediate gratification are less likely to employ controller medications.
3. Concerns about drug dependence and side effects affect teen compliance with asthma controller medications
This study attempts to elucidate factors contributing to poor controller medication adherence among college-aged teens with severe asthma. Historically, this group has had worse health outcomes than age-matched peers without asthma, a finding that may be related to poor compliance with medication. Factors examined in this study include personal beliefs about asthma and asthma medications as well as personality variables such as risk aversion and time preference. The findings of this study suggest that emphasizing the safety of asthma medications would increase the number of adhering individuals from 2 to 50, and that reducing embarrassment use would increase adhering individuals from 12 to 35. Most significantly, the data presented suggest that current asthma teaching that focuses on long-term outcomes is ineffective in teens with high risk tolerance and time preference. For these individuals, the authors suggest that a strategy of employing immediate incentives for adherence would be most effective. Of note, this study is limited in that it examined only a limited number of patients, and therefore may not be representative of all college-age patients with asthma.
Click to read the study in Pediatrics
[/tab]
[tab]
Image: PD
1. Teens with persistent asthma symptoms and a high risk tolerance have low controller medication adherence.
2. Those with a preference for immediate gratification are less likely to employ controller medications.
3. Concerns about drug dependence and side effects affect teen compliance with asthma controller medications
This [case-control] study examined factors contributing to medication non-adherence among college-aged teens with persistent asthma. The study employed a web-based survey that identified college students with asthma, and evaluated their adherence with prescribed controller medications. The survey also evaluated patient beliefs about asthma, risk tolerance, and time preference. Of the 1500 people screened, 47 had severe, persistent asthma requiring controller medications. 44% of respondents believed that they could become dependent on their asthma medications, 26% felt that taking asthma medication regularly was embarrassing, and 25% of respondents believed that controller medication should be taken as needed. Respondents were less likely to be compliant with controller medication if they had concerns about medication dependence (p=0.04), a preference for immediate gratification (p=0.03), high risk tolerance were less likely to be compliant (p= 0.02), or received federal financial aid (p=0.03).
In sum: This study attempts to elucidate factors contributing to poor controller medication adherence among college-aged teens with severe asthma. Historically, this group has had worse health outcomes than age-matched peers without asthma, a finding that may be related to poor compliance with medication. Factors examined in this study include personal beliefs about asthma and asthma medications as well as personality variables such as risk aversion and time preference. The findings of this study suggest that emphasizing the safety of asthma medications would increase the number of adhering individuals from 2 to 50, and that reducing embarrassment use would increase adhering individuals from 12 to 35. Most significantly, the data presented suggest that current asthma teaching that focuses on long-term outcomes is ineffective in teens with high risk tolerance and time preference. For these individuals, the authors suggest that a strategy of employing immediate incentives for adherence would be most effective. Of note, this study is limited in that it examined only a limited number of patients, and therefore may not be representative of all college-age patients with asthma.
Click to read the study in Pediatrics
By Emilia Hermann and Devika Bhushan
More from this author: AAP urges bottle feeding over breastfeeding in mothers with HIV, Pediatric influenza burden remains high despite new vaccination recommendations, Community hospitals rely on greater CT use to diagnose pediatric appendicitis, Cow’s milk consumption linked to increased vitamin D and decreased iron stores in early childhood, Delayed growth seen in children with congenital heart disease, No association found between maternal NSAID use and newborn pulmonary hypertension
© 2013 2minutemedicine.com. All rights reserved. No works may be reproduced without written consent from 2minutemedicine.com. Disclaimer: We present factual information directly from peer reviewed medical journals. No post should be construed as medical advice and is not intended as such by the authors or by 2minutemedicine.com. PLEASE SEE A HEALTHCARE PROVIDER IN YOUR AREA IF YOU SEEK MEDICAL ADVICE OF ANY SORT. Content is produced in accordance with fair use copyrights solely and strictly for the purpose of teaching, news and criticism. No benefit, monetary or otherwise, is realized by any participants or the owner of this domain.
[/tab]
[/tabs]