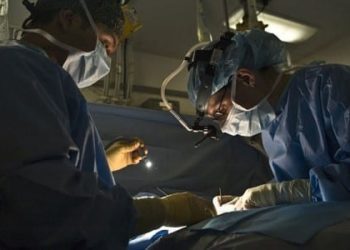
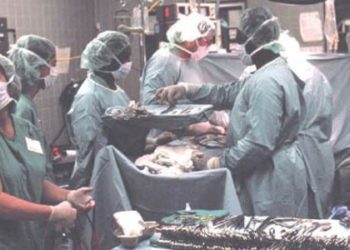
Utility superiority of mesh repair compared to primary repair for paraesophageal hernias is minimal
Feb 12th – Patients with paraesophageal hernias who underwent mesh repair instead of primary repair had higher utility scores (99.59 vs. 99.12).
[tabs tab1=”2MM Rundown” tab2= “2MM Full Report” tab3=”About the Authors”]
[tab]
Image: PD
1. Patients with paraesophageal hernias who underwent mesh repair instead of primary repair had higher utility scores (99.59 vs. 99.12).
2. The superior procedural choice is less clear during sensitivity analysis that varied independent variables such as recurrence and reoperation rates within previously reported ranges.
This study suggests that according to utility scores, mesh repair is slightly better than primary repair for paraesophageal hernias. The authors acknowledge that the difference is so small in this study, that the difference may be clinically inconsequential. With so much variability, this study is unlikely to settle the question as to which procedure is better, and likely is still highly dependent on the individual hospital experiences with each procedure. Limitations of this study include the inability of subcategorizing the outcomes based on what type of primary repair approach was used or different types of available mesh. Furthermore, the values used to calculate the overall utility score for each procedure were based on assumptions by the authors that may be inaccurate. Finally, the decision trees lacked definitive timelines, which would have been helpful for gauging the effects of specific complications on utility over time.
Click to read the study in Annals of Surgery
[/tab]
[tab]
Image: PD
1. Patients with paraesophageal hernias who underwent mesh repair instead of primary repair had higher utility scores (99.59 vs. 99.12).
2. The superior procedural choice is less clear during sensitivity analysis that varied independent variables such as recurrence and reoperation rates within previously reported ranges.
This [meta-analysis] created two utility score decision trees to evaluate the outcomes of primary repair vs. mesh repair to fix a paraesophageal hernia. Previously published systematic reviews were used to gather data about recurrences, complications, and other outcomes possible during each of the two procedures, and the results were used to create decision trees. The nodes of the decision tree for each procedure were given a likelihood of split each way based on previously reported data. The utility scores of different health states in each decision tree were then filled in, using previously reported quality of life data for some nodes, and creating assumptions about utility scores for some of the health states. It then weighed the utility scores of each end-state in each decision tree, and calculated a weighted utility score for each treatment based on the combination of these scores. In the end, mesh repair received a utility score of 99.59 and primary repair received a utility score of 99.12. During a sensitivity analysis that varied either recurrence rate or reoperation rate, both procedures were exactly equivalent when neither procedure was assumed to have a recurrence.
In sum: This study suggests that according to utility scores, mesh repair is slightly better than primary repair for paraesophageal hernias. The authors acknowledge that the difference is so small in this study, that the difference may be clinically inconsequential. With so much variability, this study is unlikely to settle the question as to which procedure is better, and likely is still highly dependent on the individual hospital experiences with each procedure. Limitations of this study include the inability of subcategorizing the outcomes based on what type of primary repair approach was used or different types of available mesh. Furthermore, the values used to calculate the overall utility score for each procedure were based on assumptions by the authors that may be inaccurate. Finally, the decision trees lacked definitive timelines, which would have been helpful for gauging the effects of specific complications on utility over time.
Click to read the study in Annals of Surgery
By David Mattos and Allen Ho
© 2013 2minutemedicine.com. All rights reserved. No works may be reproduced without written consent from 2minutemedicine.com. Disclaimer: We present factual information directly from peer reviewed medical journals. No post should be construed as medical advice and is not intended as such by the authors or by 2minutemedicine.com. PLEASE SEE A HEALTHCARE PROVIDER IN YOUR AREA IF YOU SEEK MEDICAL ADVICE OF ANY SORT. Content is produced in accordance with fair use copyrights solely and strictly for the purpose of teaching, news and criticism. No benefit, monetary or otherwise, is realized by any participants or the owner of this domain.
[/tab]
[/tabs]