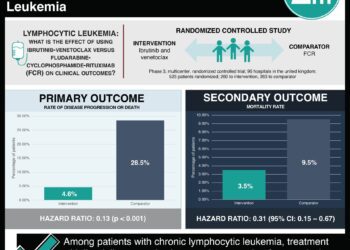
#VisualAbstract: Pirtobrutinib is safe and efficacious in the treatment of relapsed or refractory B-cell malignancies (BRUIN Trial)
1. Bruton’s tyrosine kinase inhibitor pirtobrutinib showed efficacy in the treatment of relapsed or refractory B-cell malignancies such as chronic lymphocytic leukemia, mantle cell lymphoma, Waldenstrom macroglobulinemia and marginal zone lymphoma.
2. Pirtobrutinib had a manageable safety profile, with few grade 3 or more adverse events.
Evidence Rating Level: 1 (Excellent)
Study Rundown: Covalent Bruton’s tyrosine kinase inhibitors (BTKi) are a cornerstone in the treatment of B-cell malignancies, including chronic lymphocytic leukemia (CLL), mantle cell lymphoma (MCL), Waldenstrom macroglobulinemia (WM), small lymphocytic lymphoma (SLL) and marginal zone lymphoma (MZL). However, recent data has shown that their efficacy is limited due to the development of resistance and intolerance. New in-class drugs, such as the BTKi, pirtobrutinib, are currently in development to produce agents with high selectivity and potency to overcome BTKi resistance. This first in-human, phase 1/2, open-label study sought to evaluate to safety and efficacy of the selective BTKi, pirtobrutinib. Overall, pirtobrutinib offered a good safety profile. No dose-limited toxicities were detected and the maximum tolerated dose was not reached. The majority of adverse events (87% of 1735 events) were grades 1-2. Amongst the grade 3 or higher adverse events that did occur, neutropenia was most common, and febrile neutropenia only occurred in five patients overall. No correlation was seen between pirtobrutinib exposure and frequency of grade 3 or higher adverse events. Amongst the patients evaluable for efficacy data, objective response rate (ORR) was 63% in those with CLL/SLL. The main limitation of this study is that the chronic, extended nature of some B-cell malignancies make it difficult to fully understand the long-term efficacy of pirtobrutinib. Similarly, this limits to assessment of its safety data when used for an extended period.
Click to read the study in The Lancet
Relevant Reading: Novel targeted agents and the need to refine clinical end points in chronic lymphocytic leukemia
In-Depth [randomized controlled trial]: This first-in-human, phase 1/2, open-label trial of the BTKi pirtobrutinib occurred in 27 sites across Australia, France, Italy, Poland, the UK and the USA. A total of 323 patients with refractory or relapsed B-cell malignancy were recruited in the safety population, and, amongst those, 269 in the efficacy population. Pirtobrutinib was administered once daily PO in 28-day cycles, at seven progressive dose levels: 25mg, 50mg, 100mg, 150mg, 200mg, 250mg and 300mg. The primary outcome for the phase 1 portion was determining the maximum tolerated dose of pirtobrutinib, while for phase 2 it was determining the ORR. Overall, no dose-limiting toxicities were observed (i.e., no maximum tolerated dose was reached). The majority of adverse events (87% of 1735) were grade 1/2. Neutropenia was the most common grade 3/4 adverse event, occurring in 10% of the 323 patients in this study. Only 5 patients (<1% of total) experienced febrile neutropenia. No correlation between pirtobrutinib exposure and adverse events was found. Atrial fibrillation/flutter, a serious safety concern in those taking BTKi’s, was seen in a total of two patients (<1% of total), and considered unrelated to study treatment. Among the 139 patients with either CLL or SLL, the ORR was 63% (95%CI 55-71). 88% of those patients remain on pirtobrutinib, with a median follow-up of 6 months (IQR 4-9). Of the 88 responders reported, only five discontinued treatment (four progressed and one electively discontinued). Amongst the 56 patients evaluable for efficacy with MCL, the ORR was 52% (38-65%). 57% of patients with MCL remain on pirtobrutinib, with a median follow-up of 6 months (IQR 3-9). In the 19 evaluable patients with WM, the ORR was 68%.
©2020 2 Minute Medicine, Inc. All rights reserved. No works may be reproduced without expressed written consent from 2 Minute Medicine, Inc. Inquire about licensing here. No article should be construed as medical advice and is not intended as such by the authors or by 2 Minute Medicine, Inc.