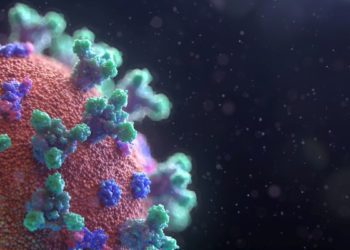
Low seroprevalence of anti-SARS-CoV-2 antibodies seen in a cross-sectional sample of residents from Wuhan, China
1. A cross-sectional sample of residents from Wuhan, China showed low overall seroprevalence (6.92%) of anti-SARS-CoV-2 antibodies in April 2020.
2. Adjusted seroprevalence was lower amongst self-reported asymptomatic individuals than those with symptoms.
Evidence Rating Level: 2 (Good)
Study Rundown: Over a year after the novel coronavirus SARS-CoV-2 (COVID-19) was characterized as a pandemic by the World Health Organization, it continues to ravage health systems worldwide. As vaccine efforts progress and increasing numbers of populations are vaccinated, it is important to analyze epidemiological trends to assess whether those have previously contracted COVID-19 are immune from further infection. This longitudinal, cross-sectional study enrolled participants from Wuhan, China, largely considered the early epicenter of the pandemic, to assess for seroprevalence of anti-SARS-CoV-2 antibodies amongst previously infected and non-infected individuals. Overall, 532 of 9542 (5.6%) enrolled participants were seropositive for pan-immunoglobulins against SARS-CoV-2. The vast majority of those who tested positive self-reported as having been asymptomatic at the time. Seroprevalence was higher amongst those with symptoms than those without. Of those positive for pan-immunoglobulins, a bit under half (39.8%) had neutralizing antibodies against SARS-CoV-2. The proportion of individuals who were positive for these antibodies did not change at the two follow-up visits in June and October-December 2020. Overall, this study presents an important step in monitoring the longitudinal impact of the COVID-19 pandemic; its basis on a major epicenter of the initial outbreak makes it particularly significant. Importantly, however, there are several limitations. Namely, this study relied largely on individuals self-reporting their COVID-19 status and symptoms, as many were not confirmed cases at the time of infection. Not only does this potentially confound the number of truly asymptomatic patients, it also prevents determining when exactly these antibodies were produced.
Click to read the study in The Lancet
Relevant Reading: Seroprevalence of immunoglobulin M and G antibodies against SARS-CoV-2 in China
In-Depth [cross-sectional study]: This longitudinal, cross-sectional study randomly sampled participants to enroll within 13 districts of Wuhan, China, a main epicenter in the beginning of the COVID-19 global pandemic. Participants having lived in Wuhan for 14 days or more since December 1, 2019 were contacted regardless of previous COVID-19 infection or not and given a standardized questionnaire regarding self-reported COVID-19 status and symptoms. A total of 9542 participants from 3556 families were enrolled. The primary goal of this study was to gather seroepidemiological data regarding the prevalence of anti-SARS-CoV-2 antibodies at a populational level over a long period of time.
Overall, among the 3556 families included, 391 families had at least one COVID-19-positive member recorded, for a total of 569 participants. Among the individuals having self-reported as previously COVID-positive, 532 were positive for pan-immunoglobulins against SARS-CoV-2 at the time of enrollment (adjusted seroprevalence = 6.92% [95% CI 6.41-7.43]). In general, seroprevalence was lower in male participants and in the 12-17 year-old age group. Notably, adjusted seroprevalence amongst self-reported asymptomatic individuals was much lower than amongst those with symptoms (5.99% [95% CI 5.50-6.48] vs. 26.13% [95% CI 21.95-30.31]). At baseline, all participants positive for pan-immunoglobulins were positive for IgG (100%), 69 for IgM (13.0%), 84 for IgA (15.8%) and 212 for neutralizing antibodies against SARS-CoV-2 (39.8%). Of the individuals who had neutralizing antibodies at baseline, the level of titres did not significantly decrease over the study period of approximately nine months (median 1/5.6 [IQR 1/2.0 to 1/14.0] at baseline vs. 1/5.6 [1/4.0 to 1/11.2] at first follow-up; p=1·0, and 1/6.3 [1/2.0 to 1/12.6] at second follow-up; p=0·29). There was no association between longitudinal concentration of antibodies in relation to age or sex.
Image: PD
©2020 2 Minute Medicine, Inc. All rights reserved. No works may be reproduced without expressed written consent from 2 Minute Medicine, Inc. Inquire about licensing here. No article should be construed as medical advice and is not intended as such by the authors or by 2 Minute Medicine, Inc.