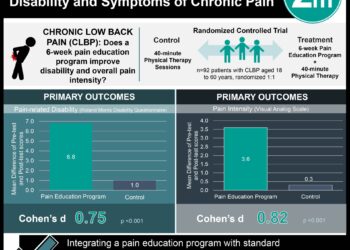
#VisualAbstract: Therapeutic aquatic exercise is superior at improving disability and severity of low back pain compared to physical therapy
1. This single-blind, randomized controlled trial found that disability and severity of low back pain significantly improved in the aquatic exercise therapy group compared to the physical therapy group at 12-months after completion of therapy.
2. A smaller percentage of people in the aquatic therapy group experienced the adverse effect of increased low back pain compared to those in physical therapy.
Evidence Rating Level: 1 (Excellent)
Study Rundown: Low back pain (LBP) is an extremely common condition that occurs at a worldwide incidence rate of 84%. Current clinical guidelines recommend exercise and physical therapy as the mainstays of treatment for LBP to decrease the pain intensity and improve disability. Therapeutic aquatic exercise, a type of water-based exercise, is commonly prescribed based some supporting evidence from systematic reviews. However, there does not currently exist evidence regarding the long-term effects of therapeutic aquatic exercise for the treatment of LBP. This single-blind, randomized controlled trial compared the disability and pain severity ratings of patients with LBP after 3 months of therapeutic aquatic exercise or physical therapy at the long-term follow up time of 12-months post-therapy. Disability and pain severity were better improved in the aquatic therapy group compared to the physical therapy group both immediately after the intervention and at long-term follow-up. The aquatic therapy group demonstrated superior improvements on the Short-form Health Survey, Pittsburgh Sleep Quality Index, Tampa Scale for Kinesiophobia, and Fear-Avoidance Beliefs Questionnaire than the physical therapy group at long-term follow-up. Fewer people in the aquatic therapy group experienced LBP caused by therapy than those in the physical therapy group. One strength of this study involved how the control group was the current gold-standard active treatment, rather than a wait-list control group. Additionally, important factors like the duration and intensity of LBP were considered as covariates in the statistical analysis. Finally, a power analysis suggested that the sample size was large enough to detect even minimal clinically significant effects. A limitation of this study is that it was largely composed of young adults with low LBP severity, so it may not be generalizable to all ages or severities. While the physical therapy group was the gold standard evidence-based treatment, it did not actually feature active exercise, so it is unclear if the superior effects from this study are due to aquatic therapy or just active exercise. Finally, it is unclear from this study alone if the effects of aquatic therapy are additive to physical therapy because a combined treatment group was not included.
Click to read the study in JAMA Network Open
Relevant Reading: Therapeutic aquatic exercise in the treatment of low back pain: a systematic review
In-Depth [randomized controlled trial]: Participants were adults with pain anywhere from the buttocks band to the rib arch that was at least a 3/10 for at least 3 months. Participants with a mental illness, cognitive impairment, or pregnancy were excluded. In this assessor-blinded randomized clinical trial, participants received aquatic or physical therapy twice a week for 12 weeks. The therapeutic aquatic exercise involved a 10-minute warm-up and cool-down surrounding a 40 minute 60-80% training intensity workout. Physical therapy consisted of 30 minutes each of transcutaneous electrical nerve stimulation and infrared ray thermal therapy. The participants were followed for an additional 12-months to compare the effects on chronic LBP of these interventions. At baseline, after the intervention, at 6-month and at 12-month follow-up, outcomes were measured, including the Roland-Morris Disability Questionnaire for chronic LBP disability and a rating of pain intensity from 0 – 10. Additionally, participants completed questionnaires on sleep, fear, perceived effect, adverse events, and whether they would recommend the intervention. Patients in the aquatic exercise (n=56) and physical therapy (n=57) group were on average younger than the mid-point of the eligible age range of 18 to 65 (average age = 31.0±11.5 years, 47.8% male). 86.7% of participants completed the entire study. The aquatic therapy group had superior improved disability compared to the physical therapy group immediately after the intervention (score difference = -1.77, 95% CI = -3.02 −-0.51) and 12-months after the intervention (score difference = -3.61, 95% CI = -5.63−-1.58, P < 0.001 for group × time interaction). The aquatic therapy group showed superior improvement of pain severity compared to the physical therapy group in post-intervention (score difference = -0.79, 95% CI = -1.31−-0.27) and 12-month follow-up (score difference = -2.04, 95% CI = -2.75−-1.34; p <0.001). The minimal clinically important difference was pre-determined to be a 2-point difference on the severity scale, which occurred in the aquatic therapy group compared to the physical therapy group at post-intervention (odds ratio [OR] = 5.24, P = 0.001) and 12-month follow-up (OR = 4.24, P < 0.001). The aquatic therapy group also had superior improvements on the Short-form Health Survey (P = 0.003), Pittsburgh Sleep Quality Index (P = 0.02), Tampa Scale for Kinesiophobia (P < 0.001), and Fear-Avoidance Beliefs Questionnaire (P = 0.04) compared with the participants in the physical therapy group. 3.6% of the aquatic therapy and 7.0% of the physical therapy group experienced LBP related to the intervention. 73.2% of the aquatic therapy and 64.9% of the physical therapy group reported subjective improvement of LBP. The global perceived effect was superior in the aquatic therapy group compared to the physical therapy group (χ2 = 11.7, P = 0.03). Significantly more participants from the aquatic therapy than the physical therapy group would recommend their intervention to a patient with LBP (92.9% vs 77.2%, χ2 = 9.5, P = 0.01). These results were consistent when factoring in the covariates of age, sex, LBP duration and intensity. Additionally, these results were consistent with those from an intention-to-treat analysis.
©2022 2 Minute Medicine, Inc. All rights reserved. No works may be reproduced without expressed written consent from 2 Minute Medicine, Inc. Inquire about licensing here. No article should be construed as medical advice and is not intended as such by the authors or by 2 Minute Medicine, Inc.