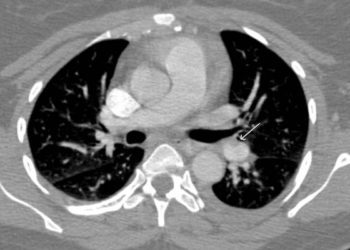
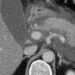
Reduced venous recanalization after acute deep vein thrombosis associated with post-thrombotic syndrome
1. In a prospective observational trial of 100 patients with a history of acute deep venous thrombosis (DVT) managed with compression therapy or anticoagulants, 34% developed post-thrombotic syndrome (PTS) after 12 to 36 months.
2. PTS was associated with older age, recurrent DVT, and insufficient recanalization post DVT.
Evidence Rating Level: 2 (Good)
Study Rundown: PTS is a common complication of DVT that manifests as pain, venous dilatation, edema, hyperpigmentation, and venous ulceration. It is hypothesized that PTS is caused by damaged valves and residual thrombus load, which contribute to venous hypertension. Recanalization is the natural process through which the thrombus is reorganized and reduced after acute DVT, such that the lumen of the vein is reestablished. Previous studies have demonstrated that less efficient recanalization and residual thrombus is associated with increased recurrence of DVT. The objective of this study was to elucidate the association between the extent of recanalization after acute DVT and the development of PTS.
This study prospectively evaluated the association between recanalization status of thrombosed veins and the development of PTS in 100 patients that were treated for acute DVT. At the conclusion of the study, PTS was significantly associated with older age, recurrent DVT, and reduced recanalization status. These findings suggest that recanalization via catheter-directed local thrombolysis may lower the risk of PTS. Strengths of this study include its prospective design, the exclusion of patients with malignancies and systemic inflammatory disorders, and the exclusion of patients who were managed with thrombolytics. This study is limited by its single center design, small study population, the use of a single ultrasound operator, and short-term follow-up duration. Larger, multicenter observational studies that assess the development of PTS over longer duration are necessary to definitely clarify this relationship.
Click to read the study in JVIR
Relevant Reading: Guidance for the prevention and treatment of the post-thrombotic syndrome
In-Depth [prospective cohort]: This study prospectively evaluated the prevalence of PTS and the association between the extent of recanalization and the development of PTS in 100 patients with acute DVT that were managed with anticoagulation or compression therapy at a single outpatient clinic in Slovenia. Patients were followed for 12-36 months and PTS was assessed via the Villalta score. Recanalization status was evaluated via ultrasonography and defined as complete (totally compressible vein to no more than 2 mm); partial (partially compressible vein), or absent (occluded and incompressible vein). At the conclusion of the trial, PTS developed in 34% of patients, and was associated with older age (p=0.007) and recurrent DVT (p=0.03). When compared to patients with complete recanalization, patients with absent or partial recanalization demonstrated an odds ratio of 6.0 for development of PTS. There was no statistically significant difference in venous reflux between the PTS and the non-PTS group (p=0.35).
Image: CC/Wiki/James Heilman, MD
©2017 2 Minute Medicine, Inc. All rights reserved. No works may be reproduced without expressed written consent from 2 Minute Medicine, Inc. Inquire about licensing here. No article should be construed as medical advice and is not intended as such by the authors or by 2 Minute Medicine, Inc.