2 Minute Medicine Rewind January 26 – February 1, 2015
In this section, we highlight the key high-impact studies, updates, and analyses published in medicine during the past week.
A Randomized Trial of Icatibant in ACE-Inhibitor-Induced Angiodema
Bradykinin inhibitors such as icatibant are used in the treatment of hereditary angioedema, and they may also be effective for ACE-inhibitor-induced angioedema resulting in decreased breakdown of bradykinin. In this multi-center, double-blind, randomized controlled trial, 30 patients suspected of ACE-inhibitor-induced angioedema were assigned to receive subcutaneous icatibant or prednisolone and clemastine (standard therapy) to compare the effect on time to symptom resolution. Patients in the icatibant group experienced symptom resolution earlier than those in the standard therapy group, after a median of 8.0 hours (IQR 3.0-16.0) compared to 27.1 hours (IQR 20.3-48.0; p=.002). Patients in the icatibant group also had faster onset of relief (2.0 vs 11.7 hours, p=.03), more patients had resolution of edema within 4 hours (38% vs 0%, p=.02), and none required rescue therapy compared to 3 people in the standard therapy group.
Hyperlipidemia in Early Adulthood Increases Long-Term Risk of Coronary Heart Disease
New cholesterol treatment guidelines focus on 10-year risk for coronary heart disease (CHD), resulting in treatment recommendation for fewer young adults with hyperlipidemia. In this prospective cohort study, investigators followed 1478 individuals from the Offspring cohort of the Framingham Heart Study who had no heart disease at approximately age 55 in order to determine the relative risk of long-term (20-year) hyperlipidemia exposure (non-HDL-C over 160mg/dL) on the development of CHD. At 15 years of follow-up, participants with 11-20 years of hyperlipidemia exposure at baseline had a greater risk of developing CHD compared to those with 1-10 years of hyperlipidemia and those with no prior hyperlipidemia at baseline (16.5% vs 8.1% vs 4.4%, log rank test p<.0001). After adjusting for other risk factors, every 10 years of hyperlipidemia exposure was estimated to increase the risk of CHD development by nearly 50% (HR 1.49, 95%CI 1.20-1.87 per decade). These results suggest that sustained, untreated hyperlipidemia as a young adult influences CHD risk later on in life, though this exposure is not taken to account in current statin therapy guidelines.
Less-Tight versus Tight Control of Hypertension in Pregnancy
Hypertension is a common disease in women of child-bearing age, however the optimal management of hypertension during pregnancy is not well understood. In this multicenter, international randomized control trial, 987 women between 14 weeks 0 days and 33 weeks 7 days were randomized to tight control (goal diastolic blood pressure < 85mmHg) or less-tight control (goal diastolic blood pressure < 100mmHg) and followed up to 6 months postpartum, with particular evaluation of peripartum complications and serious complications. In this cohort, 74.6% of patients had hypertension prior to pregnancy, and there was no statistically significant difference in pregnancy loss or need for intensive neonatal care (31.4% vs. 30.7%, OR 1.02, 95% CI 0.77 – 1.35). This was despite truly different in achieved blood pressure (mean difference in diastolic blood pressure 4.6mmHg, 95% CI 3.7 – 5.4) and more severe hypertension in the less-tight control arm (40.6% vs. 27.5%, p < 0.001). In this study, more aggressive blood pressure management during pregnancy did not result in improved maternal or fetal outcomes.
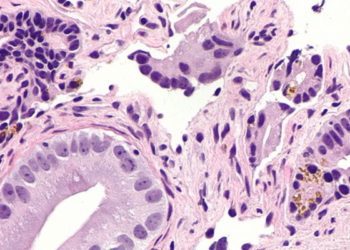
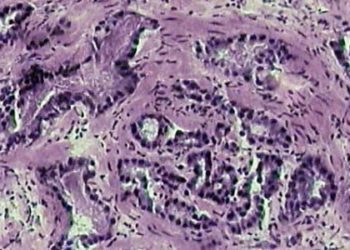
The optimal screening and surveillance for high risk prostate cancer is controversial, with urological society recommendations differing from the US preventive services task force guidelines. Targeted magnetic resonance/ultrasound fusion prostate biopsy has been suggested as a modality for more sensitive targeted biopsy in patients who screen positive for further evaluation. In this prospective cohort study, 1003 men with elevated prostate-specific antigen or abnormal digital rectal exam results underwent targeted and standard biopsy between 2007 and 2014 and the detection of high risk prostate cancer (Gleason score greater than or equal to 4+3). Targeted MR/US guided biopsy identified 461 cases of prostate cancer and conventional biopsy identified 469 cases, with agreement in results in 69% of cases. Targeted biopsy identified more high risk prostate cancers (173 vs. 122, p < 0.001) and fewer low risk cancers (213 vs. 258, p < 0.001). The addition of convention biopsy techniques to targeted biopsy primarily identified more low-risk prostate cancer (103 cases, 83% low risk, 12% intermediate risk, and 5% high risk). The optimal technique to identify high risk prostate cancer still requires more research, but targeted MR/US biopsy seems to increase the yield for high-risk prostate cancers.
The Deficit Reduction Act of 2005 allows states the option to impose co-payments for emergency room visits that were deemed to be nonurgent, however there has been little research on its effect on healthcare system, in particular emergency room, utilization. In this study, investigators compared eight states that require co-payment for nonurgent emergency room visits with ten states that did not require copayments between 2001 and 2010. Specifically, this study compared a cohort of 10555 adult Medicaid patients as identified by the Medical Expenditure Panel Survey. Their model did not identify any statistically significant difference in emergency room utilization between states with and without ED copayments (change 0.05, 95% CI -0.05 to 0.16) per Medicaid enrollee. Similarly, there was no difference in the rate of change of outpatient medical provider visits or inpatient hospitalization days. While the program helped increase flexibility in cost containment, there did not appear to be any difference in healthcare system utilization among Medicaid beneficiaries.
Image: PD
©2015 2 Minute Medicine, Inc. All rights reserved. No works may be reproduced without expressed written consent from 2 Minute Medicine, Inc. No article should be construed as medical advice and is not intended as such by the authors, editors, staff or by 2 Minute Medicine, Inc.



![Vaccines for predicted influenza strains may provide wide protection [PreClinical]](https://www.2minutemedicine.com/wp-content/uploads/2014/11/18156_lores-75x75.jpg)