2 Minute Medicine Rewind November 23 – November 30, 2014
In this section, we highlight the key high-impact studies, updates, and analyses published in medicine during the past week.
Association of Sickle Cell Trait With Chronic Kidney Disease and Albuminuria in African Americans
Sickle cell trait (SCT), inheritance of a single copy of the sickle hemoglobin mutation, affects 1 in 12 African Americans. Patients with sickle cell disease (2 copies of the same mutation) often suffer from impaired urinary concentrating ability, hematuria, chronic kidney disease (CKD), albuminuria, and end-stage renal disease (ESRD); the relationship between SCT and renal disease, however, is less understood. This study congregated data from 5 large prospective studies. Out of the 15,975 African Americans whose health data were analyzed, 1,248 were SCT carriers while 14,727 were SCT noncarriers. Carriers had an increased rate of CKD (19.2% vs. 13.5%; OR 1.57, 95%CI 1.34-1.84), incident CKD (20.7% vs. 13.7%; OR 1.79, 95%CI 1.45-2.20), decline in eGFR (22.6% vs. 19.0%; OR 1.32, 95%CI 1.07-1.61) and albuminuria (31.8% vs. 19.6%; OR 1.86, 95%CI 1.49-2.31) compared to noncarriers. This study therefore supports a link between SCT and renal disease; hence, careful monitoring of renal function is crucial in these patients.
Levofloxacin for BK Virus Prophylaxis Following Kidney Transplantation
Kidney transplantation is often limited by the side-effects and complications of the immunosuppression required to prevent rejection of the new host. One important potential complication is the activation of the BK virus (present in most of the population) in some patients. The infection starts as a viruria and ultimately progresses to a nephropathy that can lead to transplant failure in 10-100% of those patients. With no current effective treatments for BK virus infections, efforts to research a new therapy are crucial. In this Canadian randomized controlled study in 7 transplant centers, 154 kidney transplant patients were randomized to a 3-month prophylactic course of levofloxacin or placebo at the time of transplantation. There was no significant difference in the rates of BK viruria in the levofloxacin and placebo groups (29% vs. 33.3%; HR 0.91; 95%CI 0.51-1.63; P = 0.58). In addition, the levofloxacin group saw an increase in resistant bacterial infections compared to the placebo group (58.3% vs. 33.3%; RR 1.75; 95%CI 1.01-2.98). Thus, this study does not support levofloxacin prophylaxis for prevention of BK virus infections in kidney transplant patients.
Combined Rasagiline and Antidepressant Use in Parkinson Disease in the ADAGIO Study
Given more than 35% of patients with early parkinsonism have symptoms of depression (likely related to dopamine deficiency in limbic system pathways), antidepressants are commonly prescribed in this population. Used to treat the motor symptoms of Parkinson’s Disease (PD), monoamine oxidase B (MAO-B) inhibitors have also been used in the treatment of depression and thus have the potential to further help with depression symptoms in PD patients. However, because of the risk of potentially fatal serotonin syndrome, MAO-B inhibitors are rarely used in conjunction with antidepressants. In this randomized controlled study, 191 patients with idiopathic PD already taking antidepressant were randomized to rasagiline or placebo. Patients in the rasagiline group had significantly less worsening compared with patients in the placebo group in all three measured scales, namely the Movement Disorder Society–sponsored revision of the Unified Parkinson’s Disease Rating Scale Nonmotor Experiences of Daily Living (MDS-UPDRS), the original Unified Parkinson’s Disease Rating Scale (UPDRS), and the Parkinson Fatigue Scale (PFS). The mean [SE] combined rasagiline-placebo difference for these scales were −0.24 [0.11] points (P = 0.03), and −0.19 [0.10] points (P = 0.048), and −0.17 [0.09] points (P = 0.07), respectively. Given a reduced worsening of non-motor symptoms and a lack of adverse events suggestive of serotonin syndrome in the combined rasagiline-antidepressant group, there may be a role for combination therapy when treating depression in patients with PD.
The 30-day fatality rate after a stroke is about 20%, and one fourth of those deaths can be attributed to a venous thromboembolism. Recently, the CLOTS 3 trial, a trial of 2876 patients in 94 UK hospitals randomized to intermittent pneumatic compression (IPC) or no IPC, showed that IPC reduced the risk of deep vein thrombosis (DVT) and death over the first 6 months. In this follow-up study from the CLOTS 3 trial, the patients were contacted at 6 months. Using the Oxford Handicap Scale (OHS), researchers found no significant differences in disability (OHS 0-2 vs 3-6; OR 0.98; 95%CI 0.80-1.19; P=0.83). There was also no difference in whether patients lived in institutional care or not (OR 1.11; 95%CI 0.89-1.37; P=0.358) and health-related quality of life based on the EQ5D-3L questionnaire. A cost analysis showed that the cost of preventing a deep vein thrombosis and death were £1282 (95%CI 785-3077) and £2756 (1346 to not estimable). Thus, IPC prevents DVT and death but does not alter functional outcomes or improve long-term quality-adjusted survival. IPC are relatively inexpensive and without adverse effects; doctors should continue to take all these into account when deciding whether to treat patients with IPC.
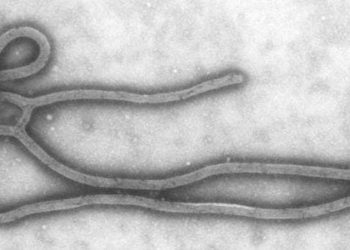
Chimpanzee Adenovirus Vector Ebola Vaccine — Preliminary Report
With the recent Ebola virus disease (EVD) epidemic counting more cases of EVD than all prior EVD outbreaks combined, the World Health Organization declared the epidemic a public health emergency of international concern and a need for prevention tools such as an effective vaccine. This accelerated the investigation of the replication-defective recombinant chimpanzee adenovirus type 3–vectored ebolavirus vaccine (cAd3-EBO) whose clinical development began in 2011. In this Phase 1 open-label trial, 20 healthy adults received one of 2 doses (2×1010 particle units or 2×1011 particle units) of the cAd3-EBO vaccine with the goal of determining its safety, side-effect profile, and immunogenicity. Reactogenicity to the vaccine was dose-dependent, with the glycoprotein-specific antibodies titers being greater in the 2×1011 particle-unit dose group (2037) than in the 2×1010 particle-unit dose group (331) (P=0.001). Similarly, immune response was also dose-dependent, with CD4 and CD8 responses being more frequent in the 2×1011 particle-unit dose group (100% and 70%, respectively) than in the the 2×1010 particle-unit dose group (30% and 20%, respectively) (P=0.004 and P=0.07). Given the only health side effects were a transient fever in 2 participants the day after vaccination, cAd3-EBO trials will be ongoing.
Image: PD
©2014 2 Minute Medicine, Inc. All rights reserved. No works may be reproduced without expressed written consent from 2 Minute Medicine, Inc. No article should be construed as medical advice and is not intended as such by the authors, editors, staff or by 2 Minute Medicine, Inc.






![Tumor-specific mutant antigens are potential targets for cancer therapy [PreClinical]](https://www.2minutemedicine.com/wp-content/uploads/2014/12/mouse-e1417555547919-75x75.jpg)