2 Minute Medicine Rewind November 3 – November 9, 2014
In this section, we highlight the key high-impact studies, updates, and analyses published in medicine during the past week.
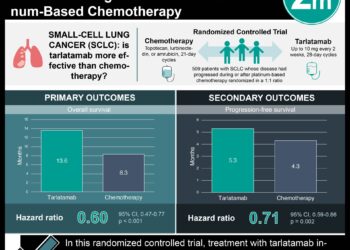
Cost-Effectiveness of CT Screening in the National Lung Screening Trial
The National Lung Screening Trial, a randomized controlled trial, demonstrated that lung cancer screening with low-dose computed tomography (CT) resulted in decreased lung cancer mortality compared to screening with chest radiography in high-risk patients, but the cost-effectiveness of these methods is of additional concern to policymakers. In this study, researchers modeled the cost-effectiveness of low-dose CT compared to chest x-ray and no screening, with a primary outcome of cost per life-year and quality-adjusted life-year (QALY) gained. Of 53,302 study participants analyzed, 1076 and 978 were diagnosed with lung cancer in the CT and radiography groups respectively. CT screening resulted in 0.03 life-years of incremental life expectancy gained compared to radiography, and 0.02 QALYs gained, with a cost of $52,000 (95% CI: $34,000-106,000) per life-year gained and $81,000 (95% CI: $52,000-186,000) per QALY gained based on Medicare reimbursement rates. Though these amounts fall below the typically recommended threshold $100,000 per QALY gained, the estimates varied significantly $40,000 to $171,000 in alternative scenarios with different assumptions.
Treatment of cervical intraepithelial neoplasia (CIN) with loop excision is believed to subsequently predispose women to preterm delivery, though the relationship between depth of excision and preterm delivery is not well characterized. In this nested case-control study from a cohort of 11,471 women who had undergone colposcopy, the authors matched 1313 women who had preterm birth with 1313 women who had term births to determine the risk of preterm birth according to the depth of CIN excision. Women who had undergone any excision were more likely to have preterm birth than those who had a punch biopsy (RR 1.38, 95% CI: 1.10-1.72), and increased depth of excision was associated with increasing risk of preterm birth (p<.001 for trend). However, women who underwent only small (<10mm) excisional treatment were not at increased risk of preterm birth compared to those who received a punch biopsy (absolute risk 7.5% vs 7.2%, respectively; RR 1.04, 95% CI: 0.79-1.37). By comparison, those who underwent very large (>20mm deep) excision were at significantly increased risk of preterm birth (absolute risk 18.0%, RR 2.40, 95% CI: 1.53-3.75 compared to small excision).
Changes in Medical Errors after Implementation of a Handoff Program
Improving patient handoffs are a current focus for potentially reducing medical errors. In this prospective intervention study, a standardized handoff system known as I-PASS (illness severity, patient summary, action list, situation awareness, and synthesis by receiver) was implemented at 9 pediatric residency training sites (875 residents) to study the effect on medical errors and preventable adverse events as measured in the 6 months before and after the intervention. Analyzing 10,740 patient admissions, standardization of patient handoff was associated with a 23% relative reduction in medical errors overall (24.5 vs 18.8 errors per 100 admissions, p<.001) and a 30% relative reduction in preventable adverse events (4.7 vs 3.3 per 100 admissions, p<.001). However, there was no significant reduction in error rate at 3 of the 9 study sites.The rate of diagnostic errors decreased overall (3.3 vs 2.1 per 100 admissions, p<.001) as did the number of near misses (19.7 vs 15.5 per 100 admissions, p<.001). An analysis of workflow showed no significant change in oral handoff duration or time spent working on the handoff document.
Nonobstructive Coronary Artery Disease and Risk of Myocardial Infarction
Nonobstructive coronary artery disease (CAD), defined as the presence of stenosis ≥20% but <70%, is common but its clinical significance is controversial. In this retrospective cohort study, investigators analyzed data from 37,674 veterans without prior known CAD who underwent coronary angiography in order to study the risk of no apparent CAD (<20% stenosis), nonobstructive CAD, and obstructive CAD (≥70% stenosis) on hospitalization for myocardial infarction (MI) at 1 year after angiography. In unadjusted analyses, increased CAD extent was associated with increased 1-year MI risk, from 0.11% among those with no apparent CAD to 2.47% among those with 3-vessel obstructive CAD. After adjustment for risk factors, increased CAD extent was associated with increased risk for MI and all-cause mortality at 1 year among those with 3-vessel nonobstructive CAD (HR 1.8, 95% CI: 1.2-2.7) or greater (up to HR 4.5, 95% CI: 3.5-5.7 for 3-vessel obstructive CAD) compared with those who had no apparent CAD on angiography. Patients with 1- or 2-vessel nonobstructive CAD had a nonsignificant increase in composite 1-year MI and all-cause mortality (HR 1.4, 95% CI: 1.0-2.0 and HR 1.2, 95% CI: 0.9-1.7, respectively). These results suggest the clinical importance of nonobstructive CAD in predicting myocardial infarction risk.
Despite randomized trial data demonstrating that low-molecular-weight heparin (LMWH) to be superior to unfractionated heparin (UFH) in reducing pulmonary embolism and heparin-induced thrombocytopenia and equally efficacious in preventing venous thromboembolism, the higher cost of LMWH may hinder widespread adoption. In this prospective economic evaluation, investigators simulated the cost-effectiveness of LMWH (base cost $8) compared to UFH (base cost $3) in 2,344 critically ill patients randomized to LMWH or UFH using 10,000 pairs of differences in cost and event rate. Patients in the LMWH group experienced significantly fewer pulmonary embolism events compared to those on UFH (24 vs 43, p=.01), and per-patient cost was nonsignificantly lower in the LMWH group ($39,508 vs $40,805, p=.41). In simulations, varying the difference in cost between the two strategies favored LMWH in 78% of cases, until the cost of LMWH exceeded $179. This suggests that LMWH is more cost-effective than UFH in critically ill patients even after accounting for a significantly increased relative price.
Image: PD
©2012-2014 2minutemedicine.com. All rights reserved. No works may be reproduced without written consent from 2minutemedicine.com. Disclaimer: We present factual information directly from peer reviewed medical journals. No post should be construed as medical advice and is not intended as such by the authors or by 2minutemedicine.com. PLEASE SEE A HEALTHCARE PROVIDER IN YOUR AREA IF YOU SEEK MEDICAL ADVICE OF ANY SORT.