2 Minute Medicine Rewind October 16, 2017
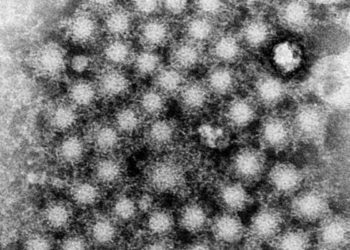
Phase 2 Placebo-Controlled Trial of Two Vaccines to Prevent Ebola in Liberia
In 2014, two candidate Ebola virus (EBOV) vaccines in phase 1 testing were studied in a phase 3 trial with the aim of preventing Ebola virus disease (EVD). An additional phase 2 sub-trial was carried out as part of evaluating safety and immunogenicity. In this phase 2 randomized controlled trial, 1500 patients were randomized to a chimpanzee adenovirus 3-based vaccine (ChAd3-EBO-Z), a recombinant vesicular stomatitis virus-based vaccine (rVSV∆G-ZEBOV-GP), or a saline placebo. Individuals with a history of EVD, a temperature of 38C or higher, and women who were pregnant or breast-feeding were excluded from participation. Researchers found that there was no significant difference in the rate of serious adverse advents during the first month for each vaccine in comparison to placebo (p=0.68), with most adverse events attributable to malaria. Notably, rates of malaria were lower in the ChAd3-EBO-Z group in comparison to placebo (p=0.03) at 12 months of follow up. Targeted symptoms such as headache, muscle pain, and fatigue were reported more often in each vaccine group than placebo at week 1 (p<0.001 for both comparisons), but this difference was not observed at 1 month of follow-up. Results for immunogenicity showed that antibody responses to EBOV glycoprotein at month 1 was 70.8% for ChAd3-EBO-Z group, 83.7% for rVSV∆G-ZEBOV-GP group, and 2.7% for placebo, (p<0.001 for both comparisons). At 12 months, this rate of antibody response was still higher in the vaccine groups (p<0.001) with the rate of antibody response occurring in 63.5% of the ChAd3-EBO-Z group, 79.5% for the rVSV∆G-ZEBOV-GP group, and 6.8% of the placebo group. Results from this trial suggest that both vaccines are able to elicit an immune response to EBOV surface glycoprotein that can be maintained for 12 months without severe safety concerns. Further studies are needed to assess whether long-term antibody changes result in decreased incidence of EVD.
Potential of Aqueous Humor as a Surrogate Tumor Biopsy for Retinoblastoma
Retinoblastoma (Rb), a primary pediatric ocular cancer, has a known genetic etiology. However, as biopsy is contraindicated due to the risk of tumor seeding, there is a lack of access to tumor DNA. This has important implications as researchers aim to characterize the relationship between tumor chromosomal changes and treatment response. In the past 5 years, the standard treatment for Rb has evolved to include withdrawal of aqueous humor (AH) before primary enucleation or intravitreal injection with chemotherapy to treat vitreous seeding. In this case series study, investigators isolated cell-free DNA (cfDNA) from 6 AH samples from 3 children with Rb with the aim of determining whether cell-free nucleic acids and proteins in AH can be used as a liquid biopsy of cell-free DNA (cfDNA) from Rb tumors. Researchers found that the 6 AH samples contained measurable concentrations of DNA, RNA, and microRNA, with higher levels measured in samples obtained after primary enucleation in comparison to intravitreal injection. For one child who underwent primary enucleation, comparison of the AH sample to a tumor biopsy sample showed that the chromosomal copy number gains and losses from the AH cfDNA correlated with the tumor DNA. In another child who underwent primary enucleation, a comparison of AH with a tumor biopsy showed some differences in the copy number variation profile, but it was noted that the tumor biopsy was from only one of many tumors in the eye. Multiple AH samples obtained from serial intravitreal injections for the third child yielded cfDNA that showed a complex set of chromosomal gains and losses that correlated with a tumor sample taken after treatment and a second enucleation. Overall, the results from the study show that AH contains measurable tumor-specific DNA with detectable chromosomal copy number variation, which holds promise for AH as a way of identifying gene changes at diagnosis or during treatment. As only 3 eyes were evaluated and one AH sample did not perfectly mimic the chromosomal changes of a tumor biopsy, however, findings need to be validated in more samples. As all 3 children evaluated had advanced disease, it will also be important to analyze AH samples from patients with smaller tumors.
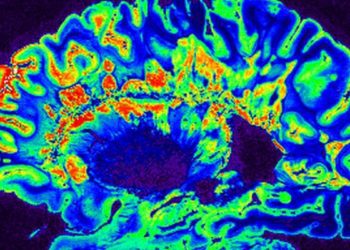
Patients with multiple sclerosis (MS) exhibit autoimmune responses to unknown central nervous system antigens, causing oligodendrocyte damage, demyelination of neurons, and neurological dysfunction. Current treatments for MS are aimed at attenuating the autoimmune response or suppressing inflammatory injury. However, there are no available treatments for remyelination or repair of myelin-related injury. Clemastine fumarate, an over-the-counter first generation antihistamine, has been identified as a possible myelination therapy as it has been found to induce oligodendrocyte differentiation and myelination in vitro and in animal models. In this randomized crossover trial, 50 patients with MS were randomized to receive clemastine fumarate for 3 months and then placebo for 2 months or vice-versa to analyze the efficacy and safety of clemastine fumarate as a treatment for patients with MS. The primary outcome was measured in terms of shortening of P100 latency delay on full-field, pattern-reversal, visual-evoked cortical potentials (VEP), an electrophysiological test used to evaluate optic nerve disease, where a disease state is associated with a longer latency delay of the P100 component. Researchers found that patients in both groups had a shortening of P100 latency while on clemastine, with a reduction of latency delay of 1.7 ms/eye (95% CI 0.5 to 2.0, p=0.0048). For patients who received clemastine first, this shortening was sustained even switched to placebo. In terms of function, patients on active treatment also showed an improvement in low-contrast letter acuity, although this was not statistically significant (p=0.085). In terms of adverse outcomes, there was a significant increase in the rate of worsening of fatigue for both groups (p=0.017) while on clemastine. Overall, this study shows that clemastine fumarate exhibits some efficacy for remyelination in patients with MS. Further studies are needed to assess and optimize the use of clemastine as a therapeutic and investigate long-term effects of remyelination.
Glecaprevir and Pibrentasvir in Patients with HCV and Severe Renal Impairment
Patients with both chronic kidney disease (CKD) and chronic hepatitis C virus (HCV) infection are at an increased risk of progression to end-stage renal disease, compensated cirrhosis, and hepatocellular carcinoma compared to patients with CKD alone. In addition, treating patients with CKD and HCV remains a challenge as many antiviral agents are contraindicated in patients with poor renal clearance. New treatments are needed to replace interferon, which is associated with many adverse events but is the only currently approved treatment for HCV in patients with CKD. Previous studies have shown that glecaprevir and pibrentasvir are two compounds that have HCV antiviral activity with minimal renal excretion. In this open-label phase 3 trial, 104 patients with HCV genotype 1-6 and stage 4 or 5 CKD were administered glecaprevir and pibrentasvir for 12 weeks in order to evaluate the efficacy of treatment with this combination of agents. Researchers found that at the end of 12 weeks, 98% of patients had a sustained virologic response (95% CI 95% to 100%). In terms of safety, 24% of patients experienced a serious adverse event, however these were considered non-drug related. Evaluation of plasma samples from 6 patients before and after hemodialysis showed that plasma levels of both compounds were not impacted greatly by hemodialysis. This study therefore shows that a combination therapy consisting of glecaprevir and pibrentasvir can be used to effectively treat HCV genotypes 1-6 in patients with CKD.
Insulin pumps have been increasingly used by patients with type 1 diabetes. Several studies, however, have reported an increased risk of ketoacidosis in patients using pumps, bringing into question the safety of insulin pumps. At the same time, some studies have shown that insulin pump therapy may decrease the frequency of severe hypoglycemia when compared to injection therapy. In this population-based cohort study, investigators compared 14,119 patients with type 1 diabetes who used insulin pumps to 16,460 patients who used insulin injections in order to study the effect on the rate of severe hypoglycemia and diabetic ketoacidosis during the most recent year of treatment. In order to have similar baseline characteristics for the two treatment groups, propensity score matching was conducted with a one-to-one matching process, which matched 9,814 patients using insulin pump therapy to 9,814 patients on injection therapy. Researchers found that in the matched cohort, the incidence of severe hypoglycemia was significantly lower with pump therapy compared to injection therapy in terms of events per 100 patient-years (difference -4.42, 95% CI -6.15 to -2.69, p<0.001). Pump therapy was also associated with fewer cases of diabetic ketoacidosis (difference -0.63, 95% CI -1.24 to -0.02, p=0.04), severe ketoacidosis (difference -0.50, 95% CI -0.99 to -0.02, p=0.04), and hypoglycemic coma (difference -0.66, 95% CI -1.24 to -0.08, p=0.02). An analysis of secondary outcomes related to metabolic control also showed that insulin pump therapy was associated with significantly lower HbA1c levels (difference -0.18, 95% CI -0.22 to -0.13, p<0.001) and lower total daily dose of insulin (difference -0.14, 95% CI -0.15 to -0.13, p<0.001) compared to insulin injection p<0.001). Results from this study therefore suggest that insulin pump therapy may be safer and more effective than injection therapy for individuals with type 1 diabetes, with lower risks of severe hypoglycemia and diabetic ketoacidosis, along with better glycemic control.
Image: PD
©2017 2 Minute Medicine, Inc. All rights reserved. No works may be reproduced without expressed written consent from 2 Minute Medicine, Inc. Inquire about licensing here. No article should be construed as medical advice and is not intended as such by the authors or by 2 Minute Medicine, Inc.