2 Minute Medicine Rewind October 5 – October 11, 2015
Acetaminophen for Fever in Critically Ill Patients with Suspected Infection
Acetaminophen is a commonly used anti-pyretic in patients admitted to the hospital, including those admitted to an intensive care unit (ICU) with potential infection/sepsis. The benefits and potential risks of treatment of fever in ICU patients have been debated for quite some time. Recent research, including a randomized controlled trial involving the physical cooling of ventilated patients with septic shock, has supported the use of acetaminophen in ICU patients with fever. On the other hand, it is well known that fever enhances immune-cell function and inhibits antimicrobial growth and so, some feel as though fever should not necessarily be treated. In this randomized controlled trial, investigators assigned 700 ICU patients with fever and known/suspected infection to receive either 1 gram of IV acetaminophen or placebo every 6 hours until ICU discharge, resolution of fever, or cessation of antimicrobial therapy. Primary outcome was ICU-free days from time of randomization to day 28. It was found that the number of ICU-free days did not significantly differ between the two groups (23 days vs. 22 days for the acetaminophen group vs. the placebo group; absolute difference of 0 days; 96.2% CI, 0 – 1, p=0.07). This study suggests that the routine use of acetaminophen to treat fever in critically ill patients does not affect the number of ICU-free days.
Urinary Tract Infection During Pregnancy, Angiogenic Factor Profiles , and Risk of Preeclampsia
Preeclampsia affects approximately 5% of pregnant women worldwide. Research into preeclampsia thus far has focused primarily on modifiable risk factors, as well as the risk of recurrence of preeclampsia in subsequent pregnancies. The pathophysiology of preeclampsia continues to be poorly understood, but it is hypothesized that the development of preeclampsia becomes more likely as the level of systemic inflammation rises. In this prospective cohort, investigators recruited and followed 2,607 pregnant women over the age of 18 throughout their pregnancies in order to study the potential relationship between systemic inflammation, urinary tract infections (UTI), and preeclampsia. Of the 2,607 women involved in the study, 129 were diagnosed with a UTI and 235 women diagnosed with preeclampsia. It was found that women with UTI’s in pregnancy had higher rates of PE compared to women who did not have a UTI throughout their pregnancy (31.1% vs. 7.8%, p<0.001). After controlling for confounding variables, UTI was associated with an odds ratio for PE of 3.2 (95% CI 2.0 – 5.1). Women who developed UTI during the first or third trimester were most likely to be diagnosed with PE (OR 2.9, 95% CI 1.8 – 4.6). These findings add to the body of literature highlighting risks for the development of preeclampsia and may provide evidence for the need for early detection and treatment of UTI’s during pregnancy. Future research should focus on how these findings may guide screening and treatment guidelines for UTI’s in pregnant women who may be at risk for preeclampsia.
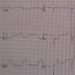
Chest pain is responsible for many emergency departments visits and is a common cause of hospital admission worldwide due to the inability to efficiently rule out acute coronary syndrome (ACS). Current guidelines recommend serial troponin tests, cardiac monitoring and repeat EKG’s in suspected myocardial infarction (MI). In this prospective cohort study, investigators studied the plasma troponin concentrations using a high-sensitivity cardiac troponin I assay in 6,304 patients with chest pain and suspected ACS. Primary outcome was a composite of myocardial infarction or cardiac death at 30 days. Researchers established negative predictive values (NPV) for the primary outcome across a range of troponin concentrations starting at 1 ng/L. Patients presenting with ST-segment elevation myocardial infarction (STEMI) and troponin concentrations > 99th percentile were excluded from the analysis. Troponin concentrations were < 5 ng/L in 2,311 (61%) of 3,799 patients without an MI, with a NPV of 99.6% (95% CI 99.3 – 99.8). In independent validation cohorts, troponin concentrations were < 5 ng/L in 594 (56%) of 1061 patients, with a NPV of 99.4% (95% CI 98.8 – 99.9). At 1 year follow up, patients with troponin concentrations < 5 ng/L had a lower risk of both MI and cardiac death, when compared to those with a troponin concentration of > 5 ng/L (0.6% vs 3.3%; aHR 0.41, 95% CI 0.21 – 0.80; p<0.0001). These findings suggest that patients presenting to emergency departments with chest pain and troponin concentrations < 5 ng/L are at low risk of cardiac events and could be discharged from hospital. Future research into the safety and efficacy of this approach will need to be done before suggesting this approach be used to guide need for hospital admission amongst patients presenting to emergency departments with chest pain and suspected ACS.
Hypothermia for Intracranial Hypertension after Traumatic Brain Injury
Traumatic brain injury (TBI) is a most common cause of permanent disability in young-middle aged adults. Hypothermia is sometimes used to treat elevated intracranial pressures (ICP) in patients presenting with TBI in some intensive care units (ICU) worldwide, however the effect of hypothermia in overall outcomes in patients with TBI and elevated ICP has not been extensively evaluated for its effect on morbidity and mortality. In this randomized controlled trial studying the effect of hypothermia in patients with TBI and an ICP of > 20 mm Hg, 195 participants were randomly assigned to receive hypothermia plus standard care (experimental group), and 192 patients were assigned to receive standard care alone (control group). Favorable outcomes (identified as a GOS-E score of 5 – 8 at 6 months) occurred in 25.7% of patients in the hypothermia group and 36.5% of the control group (p=0.03). The risk of death also favored the control group (34.9% vs. 26.6% for hypothermia vs. standard care; HR 1.45; 95% CI 1.01 – 2.10, p=0.047). Hypothermia did successfully lower the ICP in patients with TBI however care did not result in outcomes better than standard care alone. Due to safety concerns and the suggested outcome that hypothermia may actually be harmful to patients in the experimental group, this trial was stopped early, introducing risk of bias and reducing the external validity of this study. This study suggests that hypothermia does not improve functional recovery in patients with TBI and elevated ICP. More research is needed in order to guide and standardize treatment protocols for patients with TBI and elevated ICP worldwide.
Immunocompromised patients admitted to intensive care units (ICU) with respiratory failure continue to have high mortality rates ranging from 40% – 90%. The risks, as well as increased morbidity, associated with invasive mechanical ventilation are well documented. Effectively managing respiratory failure without intubation may decrease mortality rates amongst critically ill, immunocompromised patients. In this randomized controlled trial, investigators randomly assigned 374 critically ill, immunocompromised patients with acute respiratory failure to receive either early noninvasive ventilation (n=191) or oxygen therapy alone (n=183). Primary outcome was all-cause mortality within 28 days after randomization. By day 28 after randomization, 24.1% of patients in the noninvasive ventilation group had died, compared to 27.3% of patients in the oxygen group (absolute difference – 3.2, 95% CI -12.1 – 5.6, p=0.47). This study suggests that early noninvasive ventilation does not reduce rates of all cause mortality, when compared to oxygen therapy alone in critically ill, immunocompromised patients with acute respiratory failure. One major limitation of this study is that researchers were expecting a mortality rate of 35% in the oxygen group alone. The finding of a lower than expected mortality rate with oxygen therapy alone limits the power of this study to detect any significant between-group difference on mortality.
Image: PD
©2015 2 Minute Medicine, Inc. All rights reserved. No works may be reproduced without expressed written consent from 2 Minute Medicine, Inc. Inquire about licensing here. No article should be construed as medical advice and is not intended as such by the authors or by 2 Minute Medicine, Inc.




![Adverse pregnancy outcomes associated with thrombophilias [Classics Series]](https://www.2minutemedicine.com/wp-content/uploads/2015/07/Classics-2-Minute-Medicine-e1436017941513-75x75.png)