Antenatal corticosteroid administration hours before delivery may be beneficial: The EPICE cohort
1. In this population-based cohort study, any antenatal corticosteroid (ANS) administration was associated with lower infant mortality than no ANS. The largest risk reduction was seen with ANS administered 24 hours to 7 days before delivery.
2. Simulation model analyses of infants who had not received ANS predicted decreases in mortality up to approximately 30% if infants had received ANS at least 3 hours before delivery.
Evidence Rating Level: 2 (Good)
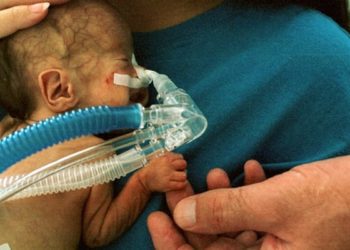
Study Rundown: Antenatal corticosteroid (ANS) administration in preterm infants is known to reduce morbidity and mortality, however ideal intervals between administration and birth are not known. This study aimed to explore the associations between ANS administration-to-birth interval and survival and morbidity among very preterm infants.
Any administration of ANS was associated with immediate, rapid and significant reduction in mortality compared to no AMS administration. The plateau risk reduction was seen with an administration-to-birth interval of 18 to 36 hours. Intervals exceeding 1 week were associated with increasing mortality, morbidity and neonatal brain injury. Simulation modeled analyses suggested that ANS administered 3 hours before delivery to infants who did not received ANS would decrease mortality by 26%. Strengths of this study included use of a population-based cohort, however use of statistical modeling for assessment of less than 24 hours administration intervals may not accurately depict outcomes and actual experimental or observational study is needed.
Click to read the study, published in JAMA Pediatrics
Relevant Reading: Relationship between the time interval from antenatal corticosteroid administration until preterm birth and the occurrence of respiratory morbidity
In-Depth [prospective cohort]: This population-based prospective cohort was conducted from 2011 to 2012 in 19 regions of 11 European countries using clinical data gathered from 4594 singleton infants with gestational ages 24-31 weeks. The exposure of interest was time from first injection of ANS to delivery which was divided into 4 categories: no ANS, first injection <24 hours, between 24 hours and 7 days or greater than 7 days. The outcomes of interest were in-hospital mortality, composite of mortality or severe morbidity (defined as intraventricular hemorrhage, cystic periventricular leukomalacia, surgical necrotizing enterocolitis and high grade retinopathy of prematurity), and severe neonatal brain injury (defined as intraventricular hemorrhage or cystic periventricular leukomalacia). Statistical analysis included modeling of association between ANS administration-to-birth intervals and the three outcomes using the 4 categories and also as a continuous variable in hours. Finally, a statistical model was applied to assess the effect of in-hospital mortality for infants who did not receive ANS, ANS <3 hours, 3 to 5 hours and 6 to 12 hours before delivery.
There were 4594 infants included in the cohort with a mean gestational age of 28.5 weeks. Any administration of ANS as compared to no ANS was associated with an immediate and rapid decline in mortality. The greatest risk reduction occurred with an administration interval of 18 to 36 hours of approximately 50%, according to statistical models using the exposure as a continuous variable. Results for the discrete exposure categories were as follows: <24 hours RR 0.6 (95%CI 0.5-0.7); 24 hours to 7 days RR 0.5 (95%CI 0.4-0.6), greater than 7 days RR 0.7 (95%CI 0.6-0.9). Similar decreases were seen for severe neonatal brain injury and the composite of infant mortality and morbidity. Intervals exceeding 1 week were associated with increasing mortality, morbidity and neonatal brain injury. Simulation modeled analyses suggested that ANS administered 3 hours before delivery to infants who did not received ANS would decrease mortality by 26%.
Image: CC/Flickr
©2017 2 Minute Medicine, Inc. All rights reserved. No works may be reproduced without expressed written consent from 2 Minute Medicine, Inc. Inquire about licensing here. No article should be construed as medical advice and is not intended as such by the authors or by 2 Minute Medicine, Inc.