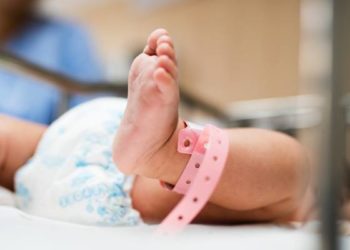
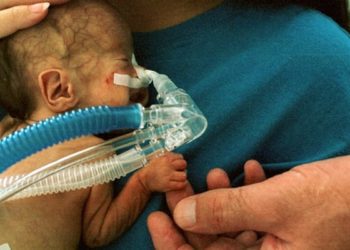
Neonatal deaths in premature infants correlate with gestational age at birth
1. A cohort study of nearly 1000 infants born preterm found that mortality risk decreased with increased gestational age and number of days of life, in a fashion comparable to postmenstrual age.
2. Common causes of neonatal mortality were respiratory distress/failure, pulmonary hemorrhage, necrotizing enterocolitis, intracranial hemorrhage, sepsis and sudden unexplained death.
Evidence Rating Level: 2 (Good)
Study Rundown: Recent advances in neonatal and obstetrical care have increased the likelihood of viability for preterm infants born as early as 22-24 weeks of gestation in some cases. However, risk of death remains high for these infants as the physiological compromise of premature birth can have long term consequences on growth and development. The present study sought to understand maternal and fetal risk factors for neonatal morbidity, common causes of death and the role of life-sustaining interventions in improving mortality rates. 941 infants born between 24 and 28 weeks gestation were included in this study108 infants (11%) died within the initial hospitalization period following birth. Of these, infants born at a lesser gestational age (GA) were more likely to die (i.e., 38% of deaths were of infants born at 24 weeks GA). Survival curves demonstrated that the longer an infant stayed alive, the lower their risk of subsequent death was, and that this mortality risk was akin to postmenstrual age. For example, an infant born at 24 weeks GA who survived 14 days would have approximately the same mortality risk as an infant born at 27 weeks GA. Preterm labor and receipt of prenatal corticosteroids were associated with a lower risk of death in neonates. Significant risk factors for infant mortality included the following: weight below 10th percentile for GA, APGAR score less than 5 at 5 minutes and an assessment of sickliness or serious adverse events by the neonatologist. This retrospective cohort study by Juul et al found that risk of death is higher in infants born at a lower GA, and decreases with each day survived in a fashion nearly analogous to survival in postmenopausal age. The findings of this study are strengthened by the large sample size and the thoroughness of the prospectively collected data. Limitations of this study include some selection bias (i.e., only patients from large, tertiary centers were included, parental consent was needed to enroll) which limits the applicability of these findings. Additionally, the nonrandomized nature of this trial makes it impossible to control for confounding factors.
Click here to read this study in JAMA Network Open
Relevant Reading: Sex difference in mortality for premature and low birth weight neonates: a systematic review
In-Depth [retrospective cohort study]: The data for this study were derived from that gathered from the Preterm Erythropoietin Neuroprotection Trial. These data were originally prospectively collected with the intent of describing risk factors for and circumstances of neonatal death for infants born prematurely. Data from 30 neonatal intensive care units across several American cities were collected for infants born between December 13, 2013 and September 26, 2016. Postnatal morbidities were defined to include the following: bronchopulmonary dysplasia, intracranial hemorrhage, periventricular leukomalacia, culture-positive sepsis, necrotizing enterocolitis, patent ductus arteriosus or retinopathy of prematurity. GA of infants who died within the initial hospitalization period at birth were as follows: 38% at 24 weeks GA, 30% at 25 weeks GA, 19% at 26 weeks GA, 14% at 27 weeks GA. Most infants who died in the neonatal period were likely to die within 10 days (50%). The following factors did not significantly correlate with risk of infant death: self-reported maternal ethnicity, race, education, prenatal care, maternal obstetrical risk factors or maternal drug or alcohol use. The protective odds ratio for death in patients who had, versus had not, gone into preterm labor was 0.91 (95% confidence interval 0.87-0.96). The odds ratio for mortality in infants who had received steroids was 0.90 (95% confidence interval 0.82-0.99) compared to those who had not. Risk factors for mortality were low birth weight (hazard ratio 2.11, 95% confidence interval 1.38-3.22) and low APGAR score at 5 minutes (2.19, 1.48-3.24). The withdrawal of life-sustaining care was documented in a median of 40% of neonatal deaths, most commonly in deaths due to hemorrhage (83%), respiratory failure (79%) and necrotizing enterocolitis (69%). The primary indication for withdrawal of life sustaining care was so that prolonged suffering could be avoided and the neonate could die peacefully, held by their parent(s).
Image: PD
©2022 2 Minute Medicine, Inc. All rights reserved. No works may be reproduced without expressed written consent from 2 Minute Medicine, Inc. Inquire about licensing here. No article should be construed as medical advice and is not intended as such by the authors or by 2 Minute Medicine, Inc.