Chemotherapy-induced peripheral neuropathy linked to increased fall risk
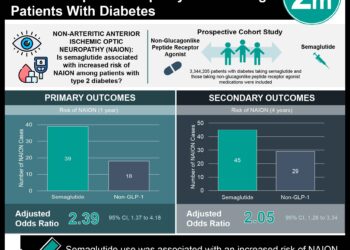
1. In a prospective study of patients receiving neurotoxic chemotherapy, those who suffered from symptoms of chemotherapy-induced peripheral neuropathy (CIPN) were more than twice as likely to have a fall or near fall during a two-month follow up.
2. The study had short term follow up and a small sample size that consisted of mostly women, which limited the generalizability of the results.
Evidence Rating Level: 2 (Good)
Study Rundown: Peripheral neuropathy is a common side effect of many common chemotherapeutic agents and results in long-term neuropathic pain and sensory loss. This prospective study was conducted to determine whether chemotherapy-induced peripheral neuropathy (CIPN) increases the risks for falls.
Of the cohort of patients receiving neurotoxic agents, about one-quarter experienced symptoms consistent with CIPN, based on an automated telephone symptom assessment system. Patients with symptoms consistent with CIPN were more than twice as likely to have a fall or near fall during the two-month study follow up period. These participants were more likely to seek medical attention for falls. While the prospective nature of the study was novel, there were several limitations. These included the small sample size, which was mostly women and Caucasian. Also, the study relied on self-reported symptoms, rather than objective measures of CIPN, which may affect the validity of the results. The CIPN patients also had significantly more telephone follow up than the asymptomatic patients, which could be a source for bias.
Click to read the study, published today in JAMA Neurology
Relevant Reading: Falls and functional impairments in cancer survivors with chemotherapy-induced peripheral neuropathy (CIPN): a University of Rochester CCOP study
In-Depth [prospective cohort]: This study enrolled a 116 participants with breast, ovarian, or lung cancer who received neurotoxic chemotherapy. The patient population was 94.0% female, 95.7% white, with 71.6% of patients having breast cancer, 19.8% having ovarian cancer, and 8.6% lung cancer. Patient’s symptoms were self-reported via an automated telephone-based assessment of symptoms for features consistent with CIPN and the occurrence and characteristics of falls or near falls. Patients were classified as ‘symptomatic’ if they had a CIPN symptom severity score of 3 or more for at least 10 days. Patients were followed for a mean of 62.2 days with non-CIPN patients having a mean (SD) of 44.6 (31.1) call assessments and CIPN patients having 68.1 (32.1) assessments (p < 0.001). There were 24 participants who reported a total of 74 events of falls or near falls.
Of the CIPN cohort, 34.3% of participants reported fall events compared to 15.4% of the participants without CIPN symptoms (HR 2.67; 95%CI 1.62-4.41). Rate of injury was not different between the groups, but CIPN patients were more likely to seek medical attention (18.8% vs. 9.5%, p = 0.01) and have head injuries (87.5% vs. 16.7%, p = 0.01). The characteristics of falls events did not differ between groups and were mostly on flat ground (83.8%) and secondary to loss of balance (59.5%) or feeling faint (27.0%).
Image: PD
©2016 2 Minute Medicine, Inc. All rights reserved. No works may be reproduced without expressed written consent from 2 Minute Medicine, Inc. Inquire about licensing here. No article should be construed as medical advice and is not intended as such by the authors or by 2 Minute Medicine, Inc.


![2 Minute Medicine: Pharma Roundup: Price Hikes, Breakthrough Approvals, Legal Showdowns, Biotech Expansion, and Europe’s Pricing Debate [May 12nd, 2025]](https://www.2minutemedicine.com/wp-content/uploads/2025/05/ChatGPT-Image-May-12-2025-at-10_22_23-AM-350x250.png)