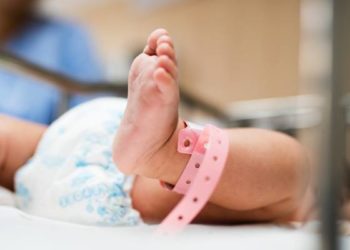
Delivery room thermal care interventions for hypothermia associated with improved outcomes
1. The majority of thermal care interventions used in the delivery room were associated with better core body temperature and decreased risk of moderate to severe hypothermia at admission or within the first 2 hours of life compared with routine care alone.
2. Use of a plastic bag or wrap with a plastic cap or with heated humidified gas was associated with lower risk of major brain injury and mortality compared to other interventions, demonstrated with low to moderate certainty of evidence.
Evidence Rating Level: 1 (Excellent)
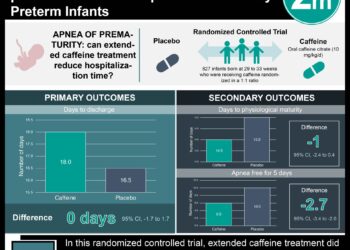
Study Rundown: Neonatal hypothermia is a serious condition with a well-established dose-response relationship to the risk of mortality, especially in preterm neonates. Thus, prevention of hypothermia in the delivery room is both a cost-effective and high-impact intervention to help reduce neonatal mortality. However, although several interventions for preventing hypothermia in the delivery room exist, no one specific intervention is considered superior to others. This network meta-analysis sought to compare the outcomes and safety of various delivery room thermal care interventions as well as to identify the intervention that could best reduce hypothermia and improve clinical outcomes for preterm neonates born at 36 weeks’ gestation or less. Primary outcomes consisted of core body temperature and incidence of moderate to severe hypothermia on admission or within the first 2 hours of life. Secondary outcomes included incidence of hyperthermia, major brain injury, and mortality before discharge. The study evaluated 9 thermal interventions including: 1) plastic bag or wrap covering the torso and limbs with the head uncovered or covered with a cloth cap, 2) plastic cap covering the head, 3) skin-to-skin contact, 4) thermal mattress, 5) plastic bag or wrap with a plastic cap, 6) plastic bag or wrap along with use of a thermal mattress, 7) plastic bag or wrap along with heated humidified gas for resuscitation or for initiating respiratory support in the delivery room, 8) plastic bag or wrap along with an incubator for transporting from the delivery room, and 9) routine care, including drying and covering the body with warm blankets, with or without a cloth cap. From 34 included trials involving 3,688 newborns, results demonstrated that most delivery room interventions were associated with improved core body temperature and decreased risk of hypothermia at admission or within the first 2 hours of life compared to routine care alone (low to moderate certainty of evidence). Additionally, the use of a plastic bag or wrap with heated humidified gas was associated with reduced risk of major brain injury (moderate evidence) and a plastic bag or wrap with a plastic cap was associated with lower risk of mortality (low evidence). One limitation of this study was that the variation among demographic and other characteristics between the trials including gestational age, varied delivery room practices, and underlying neonatal comorbidities and health profiles may have introduced intransitivity into the analysis.
Click to read the study in JAMA Pediatrics
Relevant Reading: Interventions to prevent hypothermia at birth in preterm and/or low birth weight infants
In-Depth [systematic review and meta-analysis]: This network meta-analysis screened 6,154 titles from MEDLINE, the Cochrane Central Register of Controlled Trials, Embase, and CINAHL databases from their inception to November 5, 2020. In total, the study used data from 34 randomized and quasi-randomized clinical trials that enrolled 3,688 neonates, comparing various thermal care interventions in the delivery room for the prevention of hypothermia in preterm neonates. Data extraction was completed in duplicate using a structured proforma and a network meta-analysis with Bayesian random-effects modelling was used for data synthesis. The study found that, when compared with routine care independently, plastic bag or wrap with a thermal mattress (mean difference [MD], 0.98°C; 95% credible interval [CrI], 0.60-1.36°C), plastic cap (MD, 0.83°C; 95%CrI, 0.28-1.38°C), plastic bag or wrap with heated humidified respiratory gas (MD, 0.76°C; 95%CrI, 0.38-1.15°C), plastic bag or wrap with a plastic cap (MD, 0.62°C; 95%CrI, 0.37-0.88°C), thermal mattress (MD, 0.62°C; 95%CrI, 0.33-0.93°C), and plastic bag or wrap (MD, 0.56°C; 95%CrI, 0.44-0.69°C) were all associated with increased core body temperatures post-delivery. However, certainty of evidence was moderate for 5 interventions and low for plastic bag or wrap with a thermal mattress. Finally, when compared with routine care alone, a plastic bag or wrap with heated humidified respiratory gas was associated with decreased risk of major brain injury (RR, 0.23; 95% CrI, 0.03- 0.67; moderate certainty of evidence) and a plastic bag or wrap with a plastic cap was associated with decreased risk of mortality (RR, 0.19; 95%CrI, 0.02-0.66; low certainty of evidence).
Image: PD
©2021 2 Minute Medicine, Inc. All rights reserved. No works may be reproduced without expressed written consent from 2 Minute Medicine, Inc. Inquire about licensing here. No article should be construed as medical advice and is not intended as such by the authors or by 2 Minute Medicine, Inc.