In diabetics, coronary bypass surgery and percutaneous coronary intervention similar
Image: PD
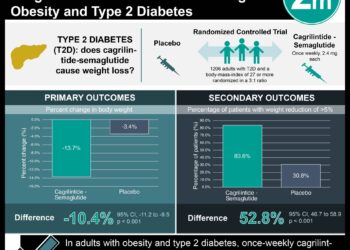
1. In patients with diabetes mellitus, coronary artery bypass graft (CABG) surgery yielded lower rates of death and myocardial infarction, but higher rates of stroke when compared to percutaneous coronary intervention (PCI).
2. Health-status and quality of life differences between the two groups were equivocal five years post intervention.
Evidence Rating Level: 1 (Excellent)
Study Rundown: This study, a follow-up to the FREEDOM (Future Revascularization Evaluation in Patients With Diabetes Mellitus: Optimal Management of Multi-vessel Disease) trial, analyzed differences in health-status and quality of life following a coronary artery bypass graft (CABG) surgery or percutaneous coronary intervention (PCI) with drug eluting stents in diabetic patients with multi-vessel coronary artery disease. Previous studies comparing surgery and stenting found that the CABG cohort fared better and reported lower rates of angina during long-term follow-up. The Seattle Angina Questionnaire (SAQ) and the Rose Dyspnea Scale (RDS) were used to measure health-status as measured by angina frequency, physical limitations, and quality of life as well as dyspnea level. Patients who underwent a CABG surgery reported lower health-status immediately following the procedure but a higher health-status at two years when compared to patients who received a PCI with a drug eluting stent. Interestingly, at five years follow-up, differences in health-status were not significant. Strengths of the study are that it is randomized and included a large cohort of patients. The study is limited by its lack of generalizability and is only applicable to diabetic patients with multi-vessel disease.
Click to read the study, published today in JAMA
Relevant Reading: Strategies for Multi-vessel Revascularization in Patients with Diabetes
In-Depth [randomized clinical trial]: This study included 1,900 patients from the FREEDOM trial who were randomized to receive either CABG surgery or PCI. Follow-up via the SAQ and RDS was maintained on 935 CABG patients and 945 PCI patients at 1 month, 6 months, 12 months, and then annually. Compared to patients who had been stented, physical limitations were higher in the surgery cohort at 1 month (-8.1,CI95% [-9.9 to -6.3]) and 6 months (-2.3,CI95% [-3.8 to -0.9]), but shifted in favor of CABG at 12 months (2.0,CI95% [0.4 to 3.6]) and 2 years (4.4,CI95% [2.7 to 6.1]) follow-up. Angina frequency (1.3, CI95% [0.3 to 2.2]) and quality of life scores (2.2, CI95% [0.7 to 3.8]) were better for CABG patients at 2 years follow-up. Beyond 2 years, differences no longer remained consistent between the two groups. In terms of mortality, CABG surgery showed less mortality at 6 and 12 months but beyond which there was no difference between CABG and PCI.
By Ravi Shah and Brittany Hasty
More from this author: Medicaid beneficiaries among most frequent visitors to the emergency department, “Polypill” improves outcomes in cardiovascular disease, Androgen deprivation therapy increases risk of acute kidney injury in patients with prostate cancer, Urine albumin excretion in black adults linked to higher risk of coronary heart disease,
© 2013 2minutemedicine.com. All rights reserved. No works may be reproduced without written consent from 2minutemedicine.com. Disclaimer: We present factual information directly from peer reviewed medical journals. No post should be construed as medical advice and is not intended as such by the authors or by 2minutemedicine.com. PLEASE SEE A HEALTHCARE PROVIDER IN YOUR AREA IF YOU SEEK MEDICAL ADVICE OF ANY SORT. Content is produced in accordance with fair use copyrights solely and strictly for the purpose of teaching, news and criticism. No benefit, monetary or otherwise, is realized by any participants or the owner of this domain.