Isoniazid for tuberculosis control ineffective in high-risk clusters
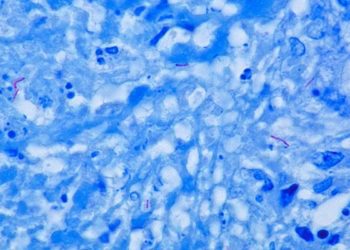
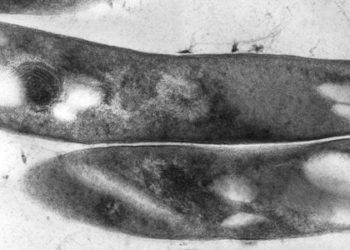
Image: PD/ Colonies of Mycobacteria organisms
1. Treatment for active tuberculosis (TB) and isoniazid preventive therapy for those at risk did not reduce the overall incidence or prevalence of TB among workers in South African gold mines.
2. Isoniazid may be effective at lowering the incidence of TB during treatment; however, there was a rapid loss of protection once treatment was completed.
Evidence Rating Level: 1 (Excellent)
Study Rundown: Tuberculosis (TB) remains one of the major contributors toward adult deaths. HIV infection, occupational exposure, and close work or living conditions increase the risk of acquiring TB. This study was one of the first to examine a community-level intervention in preventing TB in a high-risk group. The primary endpoint of this study was the incidence of TB up to 12 months after stopping isoniazid. Overall, clusters randomized to the intervention group had a lower incidence of TB during treatment; however, this effect was no longer observed by the time the primary endpoint was measured.
Limitations of this study included variable compliance and retention between the numerous clusters. Further, TB is an airborne pathogen and given that patients could choose to enroll at different times, there was a low proportion of miners taking isoniazid simultaneously in each cluster. Lastly, while most characteristics were well-controlled for between the two groups, HIV status was self-reported in this study and this may have inadvertently biased the results. Nevertheless, this study elucidated the need for a more effective way to manage latent TB in order to minimize the risk of future activation.
Click to read the study in NEJM
Click to read an accompanying editorial in NEJM
In-Depth [cluster-randomized controlled trial]: This study involved fifteen clusters of workers (n=78,744) from three gold-mining companies in South Africa. Workers were assigned to a cluster based on their employer and location. Each cluster was then randomized to either intervention or no intervention. The intervention consisted of TB screening and referral for treatment if active TB was diagnosed. Nine months of isoniazid preventive therapy was offered to those who were not diagnosed with active TB. The majority of participants were male (97.6%). At 12 months after the intervention ended, the incidence of TB in the intervention and control clusters was 3.02 and 2.95 per 100 person-years, respectively (adjusted rate ratio, 0.96; 95% CI, 0.76 to 1.21; P=0.71). During the initial 9-month follow-up period, the incidence of TB was significantly lower among the intervention clusters than the control clusters; however, the incidence was similar in the two groups following this period.
By Jonathan Liu, MD and Adrienne Cheung
More from this author: SSRI use during pregnancy not linked to increased risk of autism Combo antifungal therapy most effective treatment for cryptococcal meningitis, Rhinovirus, genes may interact to increase risk of childhood asthma, Functional MRI map for physical pain identified Glutamine and antioxidant supplementation provide no benefit for critically-ill patients New Hepatitis C virus (HCV) treatment effective
© 2012-2014 2minutemedicine.com. All rights reserved. No works may be reproduced without expressed written consent from 2minutemedicine.com. Disclaimer: We present factual information directly from peer reviewed medical journals. No post should be construed as medical advice and is not intended as such by the authors, editors, staff or by 2minutemedicine.com. PLEASE SEE A HEALTHCARE PROVIDER IN YOUR AREA IF YOU SEEK MEDICAL ADVICE OF ANY SORT.