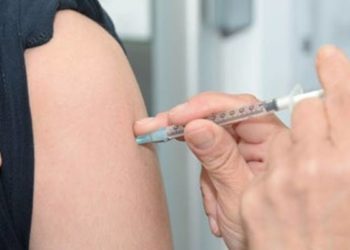
Low rotavirus vaccination coverage associated with ongoing disease transmission
1. Low coverage locations, those with <40% rotavirus vaccination rates, had the highest detection rates of rotavirus disease compared with medium coverage (>40% and <80% vaccination rate) and high coverage (greater than 80% vaccination rate) practice locations.
2. Patients from low coverage locations had 3.3 times the detection rate of rotavirus associated acute gastroenteritis compared to patients from high coverage locations.
Evidence Rating Level: 1 (Excellent)
Study Rundown: Since the introduction of the rotavirus vaccine in 2006, vaccination rates have slowly increased up to 67% in 2011 with an estimated 60-89% reduction in rotavirus associated acute gastroenteritis (AGE). Vaccination rates, however, remain low compared to those of other vaccines recommended for the same age. This study quantifies and emphasizes the effects of vaccination on reduction of rotavirus associated AGE. Children from one Texas emergency room presenting with laboratory-confirmed rotavirus AGE were asked their rotavirus vaccination status and location of their practice. Patients with non-rotavirus AGE and acute respiratory infection (ARI) served as controls. Low coverage locations had a <40% vaccination rate and were associated with the highest proportion of patients with rotavirus AGE. These patients were 3.3 times more likely to be affected by rotavirus AGE compared to high coverage locations (>80% vaccination rate). This study is limited in generalizability as it was conducted at a single site, but is strengthened by its randomized design. These findings support the need for additional efforts to educate practitioners and parents on the benefits of rotavirus vaccination and the timely administration of this vaccine to avoid nadirs of unvaccinated children that maintain disease transmission.
Click to read the study, published today in Pediatrics
Relevant Reading: Cost-effectiveness and potential impact of rotavirus vaccination in the United States
Study Author, Ms. Leila C. Sahni, MPHT, talks to 2 Minute Medicine: Texas Children’s Hospital Immunization Project, Houston, Texas.
“The results of our study provide further support for the benefits of rotavirus vaccines. We found that children who were cared for by pediatricians with low rotavirus vaccine coverage in their patients were more likely to have acute gastroenteritis caused by rotavirus than children from practices with higher coverage. Because of the narrow age range during which the rotavirus vaccine series can be initiated (first dose must be administered between 6 weeks and 14 weeks 6 days), it is extremely important that physicians recommend this vaccine at the 2-month visit for all eligible infants.”
In-Depth [case-control]: This study was conducted at the Texas Children’s Hospital (TCH) emergency department using active surveillance of children <5 years of age presenting with AGE during 2 rotavirus seasons, November, 2009 to June, 2010 and November, 2010 to June, 2011. Children were divided into rotavirus positive cases (n=100) and rotavirus negative AGE (n=725) or ARI controls (n=670). Information about vaccine administration dates and location was culled from the medical records of cases and controls. Locations were divided into low (<40% vaccination rates), moderate (>40% to <80%), and high (>80%) coverage areas. Under these categories, 4 locations (5.9%) were low, 22 (32.3%) were medium and 42 (61.8%) were high coverage. Thirty-one percent of rotavirus AGE patients came from low coverage locations while 13.1% and 9.6% came from medium and high coverage locations, respectively. Overall, children from low coverage areas were 3.3 times more likely to have had rotavirus AGE compared to children from high coverage areas (95% CI 2.4-4.4).
More from this author: E-cigarettes may lead to cigarette smoking in lower-risk teens, Childhood influenza burdens healthcare despite reported increases in vaccination, Laundry detergent pods a poisoning risk to young children, Colleges can support students with chronic medical conditions, Active sexting among teens related to sexual activity
Image: PD
©2014 2 Minute Medicine, Inc. All rights reserved. No works may be reproduced without expressed written consent from 2 Minute Medicine, Inc. No article should be construed as medical advice and is not intended as such by the authors, editors, staff or by 2 Minute Medicine, Inc.