Withholding and withdrawing care viewed as different among Asian intensivists
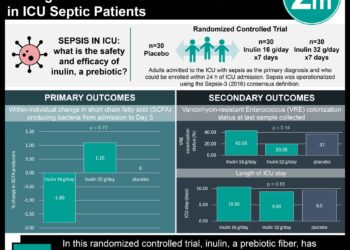
1. This survey of Asian intensive care unit physicians’ attitudes towards end of life care showed that, for patients who had little chance of a meaningful recovery, more than two-thirds of physicians withheld life sustaining treatment, but less than one-quarter withdrew such care.
2. Three-quarters of the responding physicians felt that there was an ethical difference between withholding medical care compared to withdrawing care in end of life situations.
Evidence Rating Level: 2 (Good)
Study Rundown: Significant work has been done on the attitudes of physicians in Western countries about end of life care in intensive care units (ICUs). Specifically, physicians in North America, by and large, feel that withholding and withdrawing care are appropriate and ethical depending on the clinical situation. However, not much is known about the attitudes of ICU physicians in Asian countries, where about 50% of ICU care is carried out in the world. This survey, which consisted of attitudes held by ICU physicians from 16 Asian countries regarding this issue, showed that for patients who had little chance of a meaningful recovery, more than two-thirds of physicians withheld life sustaining treatment, but less than one-quarter withdrew such care. This was likely because, amongst the respondents, three-quarters of the physicians felt that there was an ethical difference between withholding medical care compared to withdrawing care in end of life situations.
The strength of the study was including a wide group of countries in Asia, in terms of varying religious preferences, values, and beliefs, since all of those are major contributors to discussing end of life care. A weakness of the study is not having a more standardized way of picking ICUs, since there is wide variability in level of care and acuity of patients in different ICUs.
Click to read the study, published today in JAMA Internal Medicine
Click to read an invited commentary in JAMA Internal Medicine
Relevant Reading: Guidelines for withholding and withdrawing therapy in the ICU: impact on decision-making process and interdisciplinary collaboration
In-Depth [survey]: The study design consisted of questionnaires about attitudes regarding end of life care in ICUs in countries in Asia. The countries represented were Bangladesh, China, Hong Kong, India, Indonesia, Iran, Japan, Malaysia, Pakistan, Philippines, Saudi Arabia, Singapore, South Korea, Taiwan, Thailand, and Vietnam. The survey included questions that covered the domains of decision-making, communication, implementation and process, symptom management, legal or organizational guidance, ethical and legal aspects of care, religious and cultural influences, conflict resolution, and documentation.
Ultimately, 466 ICUs and 1,465 physicians were represented in the final results. The results showed that, in situations where meaningful recovery could not be expected, 70.2% of ICU physicians withheld life-sustaining treatments, but only 20.7% withdrew such level of care. In a similar light, 74.5% of respondents believed that withholding care was ethically different than withdrawing care. Physicians were more likely to refuse to implement do-not-resuscitate orders if they did not value family or surrogates’ requests (adjusted OR 1.67, p=0.006), if they were uncomfortable discussing end of life care (aOR 1.92, p<0.001), who feared legal risk (aOR 1.92, p=0.002), or if they were in low- to middle-income economies (aOR 2.73, p<0.001).
More from this author: Cardiac mortality paradoxically lower during times of national cardiology conferences, Active smoking cessation intervention may provide tangible results [Project CLIQ], Reperfusion therapy may be suboptimal for STEMIs requiring transfers, Statin therapy does not prevent osteoporotic fractures [JUPITER trial], Basic life support associated with greater survival in cardiac arrest
Image: PD
©2015 2 Minute Medicine, Inc. All rights reserved. No works may be reproduced without expressed written consent from 2 Minute Medicine, Inc. No article should be construed as medical advice and is not intended as such by the authors, editors, staff or by 2 Minute Medicine, Inc.