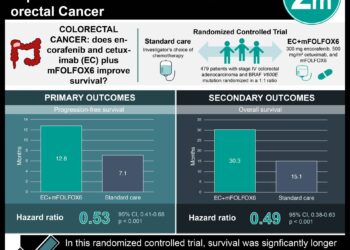
No difference in survival after laparoscopic versus open liver resection for colorectal metastases
1. The rates of 5-year overall survival were found to differ by less than a percentage point between patients in the laparoscopic group and those in the open group.
2. Recurrence-free survival at 5 years was over 5% higher in the open group, but this difference was statistically insignificant as well.
Evidence Rating Level: 1 (Excellent)
Study Rundown: Colorectal cancer (CRC) is the second leading cause of cancer death worldwide. Roughly half of patients with CRC eventually develop liver metastases, which are increasingly responsive to curative resection thanks to advances in diagnostics, oncologic treatment, and surgical techniques. Laparoscopic liver surgery is minimally invasive and has been shown in numerous retrospective studies as well as the randomized controlled OSLO-COMET trial to improve short-term outcomes relative to open surgery, but the long-term effects of each approach were unclear. In this OSLO-COMET extension study, no differences in recurrence-free survival or overall survival were detected between patients in the laparoscopic group and patients in the open group at 5 years. Median recurrence-free survival was also similar between groups. However, given the limited sample size, the possibility of small to moderate differences in survival in either direction could not be excluded. This study was conducted at a single high-volume surgical center, which minimized case-to-case variation, but this design also limited generalizability to other, non-expert settings. Future multicenter randomized controlled trials may reveal more insight regarding noninferiority and other specific secondary endpoints.
Click here to read the study in Annals of Internal Medicine
Relevant Reading: Laparoscopic Versus Open Resection for Colorectal Liver Metastases: The OSLO-COMET Randomized Controlled Trial
In-Depth [randomized controlled trial]: Between February 2012 and February 2016, 280 patients with colorectal liver metastases were assigned using block randomization to receive either laparoscopic or open parenchyma-sparing liver resection (fewer than 3 consecutive liver segments). Patients who required formal hemihepatectomy, vessel or bile duct reconstruction, or ablation were excluded. Survival analysis was performed in January 2020, and median overall survival was 80 months (95% CI, 63 to 97 months) in the laparoscopic surgery group and 70 months (95% CI, 48 to 92 months) in the open surgery group (hazard ratio [HR], 0.93; 95% CI, 0.67 to 1.30). Overall survival rates for 1, 3, and 5 years were 94%, 71%, and 54%, respectively, in the laparoscopic group and 93%, 71%, and 55% in the open group (between-group difference at 5 years, 0.5 percentage point; 95% CI, −11.3 to 12.3 percentage points). Median recurrence-free survival was 17 months (95% CI, 10 to 23 months) in the laparoscopic group and 16 months (95% CI, 8 to 24 months) in the open group (HR, 1.09; 95% CI, 0.80 to 1.49; P = 0.57); the 5-year recurrence-free survival rate was slightly higher in the open surgery group (36% vs. 30%; 95% CI, −6.7 to 18.7 percentage points). A total of 60 patients required repeat surgery for recurrent liver metastases.
Image: PD
©2020 2 Minute Medicine, Inc. All rights reserved. No works may be reproduced without expressed written consent from 2 Minute Medicine, Inc. Inquire about licensing here. No article should be construed as medical advice and is not intended as such by the authors or by 2 Minute Medicine, Inc.


![2MM: AI Roundup- AI Cancer Test, Smarter Hospitals, Faster Drug Discovery, and Mental Health Tech [May 2nd, 2025]](https://www.2minutemedicine.com/wp-content/uploads/2025/05/Untitled-design-350x250.png)