Post-operative pain similar in robotic and conventional laparoscopy for gynecologic procedures
1. No difference in post-operative pain or its effect on quality of life was observed when comparing robotic laparoscopy with conventional laparoscopy for gynecologic procedures.
2. Robotic-assisted surgeries were significantly longer than conventional laparoscopic surgeries.
Evidence Rating Level: 2 (Good)
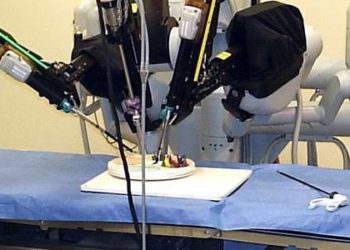
Study Rundown: Robotic-assisted laparoscopic gynecologic surgery has become increasingly popular. The technique can be used to treat various gynecologic conditions, including cervical and uterine cancer, endometriosis, pelvic organ prolapse and uterine fibroids. Robotic operations permit three-dimensional visualization and improved dexterity by incorporating a “wrist” component, which straight stick laparoscopy tools lack. Purportedly, as compared to conventional laparoscopy, robotic-assisted surgery results in shorter hospitalization and recovery times and decreased post-operative pain. While the theoretical benefits of the robotic approach are many, the technology is expensive and several studies have not shown benefits in duration of hospitalization or recovery, pain or risk of complications. The present work is the first to study pain and its impact on quality of life across different gynecologic surgeries. The authors found no differences in pain or analgesic use between the robotic and conventional arms, but detected more post-operative problems with sleep among patients in the robotic group.
A key limitation of these findings is the difference in the proportion of major procedures between the two groups – 61% in the robotic-assisted group, 34% in the conventional laparoscopy group. Other limitations of the study include the lack of randomization, small sample size, and lack of specific inclusion criteria. Larger studies exploring post-operative pain and cost-effectiveness for different procedures are needed to better understand the role of robotic-assisted surgeries for gynecologic conditions.
Click to read the study in AJOG
Relevant Reading: Robotic-assisted laparoscopic hysterectomy vs. traditional laparoscopic hysterectomy: five meta-analyses
In-Depth [prospective cohort study]: This study evaluated the relationship between pain and laparoscopic surgical approach among women who had robotic-assisted surgeries (n=56) and those who had conventional laparoscopic surgeries (n=55) for both benign and malignant gynecologic conditions. The primary outcome was pain, while secondary outcomes were analgesic use and impact of pain on quality of life. Pain was assessed at 3 specific time points using the Brief Pain Inventory-Short Form.
In the robotic surgery group, 61% of women underwent major procedures compared to only 36% of women in the conventional laparoscopic surgery group. Major surgeries were ones that required hysterectomy and/or lymph node dissection. Robotic-assisted procedures were significantly longer than conventional ones (p<0.001). No difference in pain levels were noted pre-operatively, immediately post-operatively or delayed post-operatively between the two groups. There was also no difference in the type or route of administration of pain medications. Patients who underwent robotic-assisted surgeries reported that pain had a greater impact on their sleep (p=0.03).
Image: PD
More from this author: Intrahepatic cholestasis of pregnancy linked to poor outcomes, Severe acne linked to endometriosis, Postpartum pelvic floor muscles may have limited value, Vitamin D not effective in reducing recurrent bacterial vaginosis, Cervical length may predict preterm delivery
©2012-2014 2minutemedicine.com. All rights reserved. No works may be reproduced without expressed written consent from 2minutemedicine.com. Disclaimer: We present factual information directly from peer reviewed medical journals. No post should be construed as medical advice and is not intended as such by the authors, editors, staff or by 2minutemedicine.com. PLEASE SEE A HEALTHCARE PROVIDER IN YOUR AREA IF YOU SEEK MEDICAL ADVICE OF ANY SORT.