The OVIVA trial: oral antibiotics noninferior to intravenous antibiotics for bone and joint infections
1. Patients with bone and joint infections treated with 6 weeks of oral or intravenous antibiotic therapy had similar rates of treatment failure after 1 year.
2. Serious adverse events occurred at similar rates for patients in the oral and intravenous antibiotic groups.
Evidence Rating Level: 1 (Excellent)
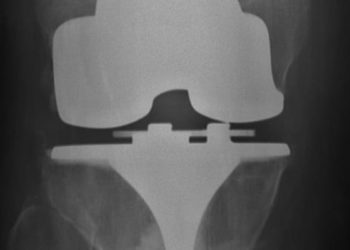
Study Rundown: Bone and joint infections are typically treated with surgical washout and a prolonged course of intravenous antibiotic therapy. Use of intravenous antibiotics has been a long-held standard of care which has significant drawbacks compared to oral treatment, though a thorough comparison has not been conducted recently. The Oral versus Intravenous Antibiotics for Bone and Joint Infection (OVIVA) trial sought to compare oral and intravenous antibiotics for patients with orthopaedic infections. Patients were randomized to oral or intravenous antibiotics after 1 week of starting antibiotic therapy. There was no significant difference in the primary outcome of treatment failure at 1 year between the oral and intravenous antibiotic groups. Incidence of serious adverse events was also similar between treatment groups.
This large randomized trial provides strong support to challenge a widely and long held conclusion that intravenous antibiotics are superior to oral antibiotics for treating orthopaedic infections. Its strengths include strong patient follow-up and inclusion of patients with multiple bacterial pathogens who were therefore treated with multiple kinds of antibiotics. Subgroup analysis of specific types of antibiotics was not performed, which may have provided useful information as to which kinds of infections were best treated with oral versus intravenous antibiotics.
Click to read the study in NEJM
Click to read an accompanying editorial in NEJM
Relevant Reading: Comparative effectiveness of intravenous vs oral antibiotics for postdischarge treatment of acute osteomyelitis in children
In-Depth [randomized controlled trial]: This multicenter, open-label, randomized controlled trial enrolled patients between 2010 and 2015. Eligible participants had osteomyelitis, a native infected joint, or an infected prosthetic/orthopaedic fixation device. If patients were surgically treated, randomization to oral or intravenous groups occurred within 7 days of surgery. Patients were treated for 6 weeks after randomization, and extended antibiotic treatment was also possible if clinically warranted. If no surgery was required, randomization occurred within 7 days of beginning antibiotics. Choice of antibiotics was left to the guidance of treating physicians. Participants in the oral (n=466) and intravenous (n=443) groups were followed for 1 year to assess for the primary outcome of treatment failure, which showed oral therapy to be noninferior to intravenous therapy (13.2% vs 14.6% failure for oral and intravenous groups, respectfully; difference in risk, -1.4%; 95% confidence interval [CI], -5.6 to 2.9). Intention-to-treat and per-protocol analysis supported the conclusion of oral therapy as noninferior. Patients in the intravenous group more commonly discontinued their treatment. Patients in the intravenous group also experienced longer hospital stays and had significantly more complications with intravenous catheters. Serious adverse events occurred at similar rates in the two groups (26.2% and 27.7% for oral and intravenous groups, respectively; P=0.58). Incidence of C. difficile diarrhea was similar in the two groups.
Image: PD
©2019 2 Minute Medicine, Inc. All rights reserved. No works may be reproduced without expressed written consent from 2 Minute Medicine, Inc. Inquire about licensing here. No article should be construed as medical advice and is not intended as such by the authors or by 2 Minute Medicine, Inc


![ABCD2 Score: Predicting Early Stroke Risk After Transient Ischemic Attack (TIA) [Classics Series]](https://www.2minutemedicine.com/wp-content/uploads/2013/05/web-cover-classics-with-logo-medicine-BW-small-jpg-350x250.jpg)