Transcatheter aortic valve replacement provides only minor benefit to quality of life
Image: PD/CDC/Aortic Stenosis
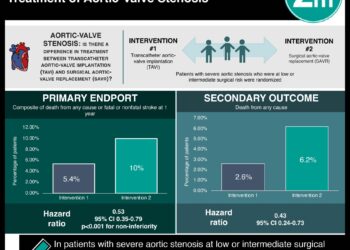
1. According to this systemic review, transcatheter aortic valve replacement (TAVR) is associated with a decrease in New York Heart Association (NYHA) functional class, but only a minor improvement in quality of life (QOL).
Evidence Rating Level: 1 (Excellent)
Study Rundown: Surgical aortic valve replacement (SAVR) is the gold standard for treatment of symptomatic aortic stenosis (AS), and has been shown to both decrease mortality and improve quality of life. Recently transcatheter aortic valve replacement (TAVR) has become an alternative for patients who are not surgical candidates. TAVR has been shown to have comparable mortality benefit to SAVR. However, the benefit of TAVR on quality of life (QOL) and functional status is still in question. This systematic review looked at the effects of TAVR on the clinical markers of disease and QOL. The reviewed studies showed a trend in decreasing in New York Heart Association (NYHA) class among those patients treated with TAVR, although many individual studies showed only a mild improvement when compared to conservative treatment. TAVR patients only showed a minor improvement in QOL, with a modest reduction as measured by Short Form 12/36 Health survey physical component summary (SF-PCS), and an even smaller change in mental component summary (MCS) scores. Furthermore, most of the studies included did not have independent comparison group receiving an alternative treatment, which may result in an overestimation of improvement from TAVR. The main limitation of this study is the heterogeneity in the studies selected, as well as the few number of total studies reviewed.
Click to read the study, in the Annals of Internal Medicine
Relevant Reading: Quality of life among patients with severe aortic stenosis
In-Depth [systematic review]: The authors included 60 observational studies and 2 randomized, controlled trials in their systematic review. The overall quality of the included studies was low, with a high risk of bias and many studies lacking independent conservative treatment arms and assessors of functional outcomes. Among patients given TAVR, there was an average improvement of about 1 NYHA class at all lengths of follow-up, from 6 months to 36 months, although 8 studies showed no statistically significant improvement from TAVR. Together, the decrease in NYHA class from TAVR was comparable to those who underwent SAVR. However, there were large proportions of patients who did not improve, evident in two individual studies showing 21% and 30% of patients with either no change or worsening functional status. There were also improvements of quality of life comparable to SAVR, but only slightly better than conservative treatment. The mean changes to SF-PCS scores showed improvement with TAVR, but with high heterogeneity, shown with a range of 4.9 and 26.9 points at 12 months. Changes to MCS scores were also variable, with a range of 1.0 to 8.9 points at 12 months. Among all TAVR patients, the risk of all-cause mortality and re-hospitalization remained high, with a pooled risk of 20% and 17%, respectively, at 12-23 months and 31% and 25% past 24 months. Overall, the effect of TAVR on reducing NYHA class is present but variable, but the improvement in quality of life is generally modest.
More from this author: USPTF recommends tobacco counseling for adolescents by primary care physicians Peer-delivered education through social networking increases home-based HIV testing ACP recommends weight loss and CPAP for obstructive sleep apnea Lifestyle interventions can reduce type 2 diabetes among high-risk patients Home scoring system may prevent unnecessary pharyngitis clinic visits No evidence for the cognitive side-effects of statins Household firearm accessibility increases risk of suicide and homicide
© 2012-2014 2minutemedicine.com. All rights reserved. No works may be reproduced without expressed written consent from 2minutemedicine.com. Disclaimer: We present factual information directly from peer reviewed medical journals. No post should be construed as medical advice and is not intended as such by the authors, editors, staff or by 2minutemedicine.com. PLEASE SEE A HEALTHCARE PROVIDER IN YOUR AREA IF YOU SEEK MEDICAL ADVICE OF ANY SORT.