Transfusion therapy linked with reduced neurovascular disease in sickle cell anemia
1. In children with sickle cell anemia and silent infarcts, the incidence of recurrent infarcts was significantly lower in the blood transfusion group compared to the observation group.
2. The rates of vaso-occlusive episodes, priapism, acute chest syndrome, and new avascular necrosis of the hip were lower in the transfusion group, while rates of transfusion reactions and elevated ferritin were higher.
Evidence Rating Level: 1 (Excellent)
Study Rundown: Recent research has found the presence of silent cerebral infarcts in a substantial number of children with sickle cell anemia. Children with these infarcts, defined by neuroimaging evidence of infarcts in the absence of clinically evident deficits, are at an increased risk for stroke, new or enlarged silent infarcts, poor academic achievement, and lower IQ compared to children with sickle cell anemia who do not have evidence of silent cerebral infarcts on MRI. The Silent Cerebral Infarct Multi-Center Clinical Trial (SIT) tested the hypothesis that among children with sickle cell anemia and neuroimaging evidence of silent brain infarcts, regular blood transfusions would lower the incidence of infarct recurrence.
In this study, children receiving regular blood transfusions had a significantly decreased incidence of infarct recurrence compared to children undergoing standard therapy (observation) over a median of 3 years of follow-up. However, there was no significant difference in cognitive outcomes between the intervention groups. The study also found significantly lower rates of other complications associated with sickle cell anemia (vaso-occlusive pain, acute chest syndrome, priapism, and new symptomatic avascular necrosis of the hip) in the transfusion group, with a concomitant increase in rates of transfusion reactions and elevated ferritin levels.
The greatest strength of this study is the use of a randomized design to address an important clinical question in the management of sickle cell anemia. Major drawbacks include the fact that assessment with IQ does not provide a sensitive account of cognitive function in specific domains (e.g. executive function, memory, or attention), and the fact that the extremely high rates of follow-up in the transfusion group may prove hard to reproduce in the community setting. This study lays the groundwork for future research investigating cognitive and functional outcomes over a longer period of time.
Click to read the study, published today in NEJM
Click to read the accompanying editorial in NEJM
Relevant Reading: Prevention of a First Stroke by Transfusions in Children with Sickle Cell Anemia and Abnormal Results on Transcranial Doppler Ultrasonography
In-Depth [randomized controlled trial]: This randomized, single-blind clinical trial assigned children, aged 5-15 years of age, with sickle cell anemia and evidence of silent cerebral infarcts on brain MRI to receive regular blood transfusions or standard care (observation). 196 children, with a mean age of 10 years, were followed for a median of 3 years. The primary outcome measure was recurrence of infarct or hemorrhage on neuroimaging, clinical evidence of permanent neurologic injury, or both. Children in the intervention group received a transfusion approximately every month to maintain a target hemoglobin concentration greater than 9.0g/dL and a target hemoglobin S concentration of 30% or less of total hemoglobin.
In an intention-to-treat analysis, the incidence of recurrent infarcts in the transfusion group was 0.41 times the incidence in the control group (95% confidence interval, 0.12 to 0.99; P=0.04); the absolute risk reduction was 8%, and the relative risk reduction was 58%. There was no significant improvement in cognitive outcomes in the transfusion group compared to the control group. Baseline factors significantly associated with infarct recurrence included younger age, history of recurrent headaches, and a higher steady-state reticulocyte count. There were significantly reduced rates of vaso-occlusive pain, acute chest syndrome, priapism, and new symptomatic avascular necrosis of the hip in the transfusion group (P=0.004, <0.001, 0.02, and 0.02 respectively). Notably, there was a significantly higher incidence of blood-transfusion reactions (52% were allergic, 32% were febrile nonhemolytic) and ferritin levels exceeding 1500ng/mL in the transfusion group.
More from this author: Letermovir safe, effective in CMV prophylaxis following stem-cell transplantation, Combination CPAP, weight loss for obstructive sleep apnea offer no added benefit, Tofacitinib superior to methotrexate monotherapy for rheumatoid arthritis, Gene mutation associated with antimalarial resistance across Southeast Asia, Moderate sodium intake optimal for cardiovascular health
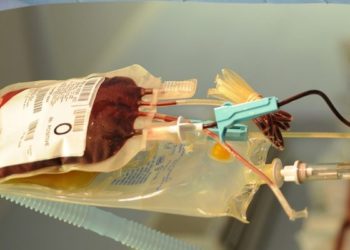
Image: PD
©2012-2014 2minutemedicine.com. All rights reserved. No works may be reproduced without expressed written consent from 2minutemedicine.com. Disclaimer: We present factual information directly from peer reviewed medical journals. No post should be construed as medical advice and is not intended as such by the authors, editors, staff or by 2minutemedicine.com. PLEASE SEE A HEALTHCARE PROVIDER IN YOUR AREA IF YOU SEEK MEDICAL ADVICE OF ANY SORT.