#VisualAbstract: Treatment Effect of Omalizumab on Severe Pediatric Atopic Dermatitis
1. In treatment-resistant childhood atopic dermatitis, omalizumab significantly reduced the severity of dermatitis and improved quality of life compared to placebo.
Evidence Rating Level: 1 (Excellent)
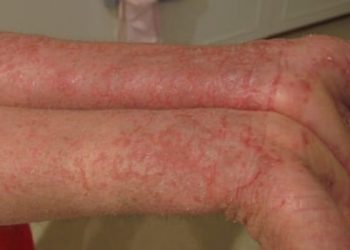
Anti-IgE medications such as omalizumab are well-tolerated in patients with severe asthma and atopy; however, no large randomized trials have examined its efficacy in children experiencing treatment-resistant atopic dermatitis. The objective of this double-blind, placebo-controlled study was to examine the effectiveness of omalizumab in treating severe atopic dermatitis in children, with the objective Scoring Atopic Dermatitis (SCORAD) index 24 weeks post-treatment initiation as the primary outcome of interest. Sixty-two participants aged 4 to 19 years (mean [SD] age = 10.3 [4.2] years) were recruited following initial screenings, which required a SCORAD index of 40 or greater and resistance to standard treatment. Participants were randomly assigned to placebo (n = 32) or omalizumab (n = 30) for 24 weeks, with dosage being based on participants’ initial body weight and total IgE (30-1,500 IU/mL). Assessments were conducted at 24 weeks as well as 48-week follow-ups, including the SCORAD, Children’s Dermatology Life Quality Index/Dermatology Life Quality Index (CDLQI/DLQI), and the Pediatric Allergic Disease Quality of Life Questionnaire (PADQLQ). Following 24 weeks, adjusted SCORAD indices demonstrated an average reduction of 6.9 points between groups, with the omalizumab group showing significantly greater improvement (95% CI -12.2 to -1.5, p=0.1). Mean changes in CDLQI/DLQI scores (-3.5; 95% CI -6.4 to -0.5) and PADQLQ scores (-0.5; 95% CI -0.9 to 0.0) both favored the omalizumab group. These differences were significant despite lower potent topical corticosteroid use in the treatment group. Overall, study findings suggested that omalizumab significantly reduced atopic dermatitis severity, improved quality of life and potential topical corticosteroid-sparing in children with atopy, severe eczema and high total IgE levels with treatment-resistant disease.
Click to read the study in JAMA Pediatrics
©2019 2 Minute Medicine, Inc. All rights reserved. No works may be reproduced without expressed written consent from 2 Minute Medicine, Inc. Inquire about licensing here. No article should be construed as medical advice and is not intended as such by the authors or by 2 Minute Medicine, Inc.