2 Minute Medicine Rewind April 5, 2021
Post-COVID syndrome in individuals admitted to hospital with COVID-19: retrospective cohort study
1. Hospital readmission and all-cause mortality rates are 3.5 and 7.7 times higher in COVID-19 patients after discharge, than the general population.
2. In addition to respiratory illness, COVID-19 patients experienced higher rates of diagnosis of a major adverse cardiovascular event, diabetes, chronic kidney disease, and chronic liver disease.
Evidence Rating Level: 2 (Good)
Much of the research on post-COVID syndrome, or the long-term effects of COVID-19, have been focused on respiratory illness. However, there is growing evidence demonstrating effects on other organ systems and patterns of disease. To assess the epidemiology of post-COVID syndrome, the current study based in England identified the incidence of all-cause mortality, admission rates to the hospital, and organ specific impairment, after COVID-19 patients were discharged. This was compared to controls from the general population, matched by age, sex, ethnicity, comorbidities, and other personal and clinical characteristics. 47,780 COVID-19 patients were included in the study, 54.9% of whom were male, and with a mean (SD) age of 64.5 (19.2). For a mean follow-up of 140 days, the study found that 29.4% of COVID-19 patients were readmitted and 12.3% died following discharge, with an incidence of 766 readmissions (95% CI 753-779) and 320 deaths (312-328) per 1000 person years. Compared to the controls, these rates were 3.5 (95% CI 3.4-3.6) and 7.7 (7.2-8.3) times more respectively. In terms of organ specific impairment, 29.6% were diagnosed with respiratory illness, 4.9% with diabetes, 4.8% with an adverse cardiovascular event, 1.5% with chronic kidney disease, and 0.3% with chronic liver disease. COVID-19 patients were diagnosed with these conditions 6.0, 3.0, 2.8, 1.9, and 1.5 times more frequently than the matched controls respectively. Overall, this study showed that the long-term effects of COVID-19 affect numerous organ systems in the body, and COVID-19 patients are at greater risk of re-admissions and all-cause mortality than the general population.
1. Women patients with stroke were 10% less likely than male patients to achieve a door-to-computed tomography time (DTCT) within 25 minutes, the recommended time to prevent delayed treatments.
2. Black patients were 12% less likely, and Hispanic patients 7% more likely than white patients to achieve a DTCT within 25 minutes.
Evidence Rating Level: 2 (Good)
Stroke is a leading cause of morbidity and mortality, and there is a narrow time window for the gold standard treatment, intravenous tissue plasminogen activator, to be effective. The door-to-computed tomography time (DTCT) is an important indicator for timeliness of therapeutic interventions for stroke. It refers to the time from hospital arrival to brain CT imaging, which is ideally 25 minutes and under. Due to previous reports suggesting that there are disparities in stroke care amongst different sex and race-ethnic demographics, the current study investigated whether there are sex or race-ethnic disparities in DTCT. Data was collected from the Florida Stroke Registry, which included 93 Florida hospitals. The study population consisted of 63,265 records, 50% of whom were male, and with a mean (SD) age of 72 (14). The median DTCT was 22 minutes (interquartile range 32), and DTCT ≤ 25 was accomplished in 56% of patients. In terms of sex, the median DTCT was 21 minutes (IQR 34) and 23 minutes (IQR 36) in men and women respectively. For race, the median DTCT was lowest in White patients at 21 minutes (IQR 32), then Hispanic patients at 22 min. (IQR 32), followed by Black patients at 23 min. (IQR 37). As well, women patients and black patients with strokes were less likely to achieve DTCT ≤ 25 min. compared to male patients and white patients respectively (odds ratio 0.90, 95% CI 0.87-0.93; OR 0.88, 95% CI 0.84-0.94). Hispanic patients were more likely than white patients to achieve DTCT ≤ 25 min. (OR 1.07, 95% CI 1.01-1.14). Overall, this study demonstrated that discrepancies in DTCT for suspected stroke still exist between different sex and race-ethnic groups, with further research being pertinent for identifying the causes and reducing these disparities.
1. Tislelizumab, a monoclonal antibody and PD1/L1 inhibitor, when combined with chemotherapy, showed significantly prolonged progression free survival and higher objective response rate, compared with chemotherapy alone.
Evidence Rating Level: 1 (Excellent)
Squamous non-small-cell lung cancers (sq-NSCLCs) are often diagnosed at a later stage, leading to poor prognosis and difficult disease management. However, there has been promise shown when combining chemotherapy with monoclonal antibody treatments that block programmed cell death receptor 1 and its ligand (PD-1/L1 inhibitors). The sole approved treatment for advanced sq-NSCLC is a PD-1/L1 inhibitor (pembrolizumab) and standard chemo. This led to research into the potential of tislelizumab, a monoclonal antibody of the same class. Early trials showed that combining tislelizumab with platinum-based therapy was well tolerated, demonstrated antitumour activity, and had an 80% or 67% objective response rate, depending on the chemo regimen used. This current study was a phase 3 trial examining the efficacy and safety of tislelizumab plus chemotherapy for advanced sq-NSCLC. The study population consisted of 360 patients (median [range] age of 62 [34-74] years; 91.7% male) with stage IIIb or IV sq-NSCLC. They were randomized roughly equally into 3 arms: Arm A consisted of tislelizumab plus paclitaxel and carboplatin, Arm B consisted of tislelizumab plus nab-paclitaxel and carboplatin, and Arm C consisted of paclitaxel and carboplatin (no tislelizumab). These regimens were administered intravenously every 3 weeks, and the outcomes investigated were progression-free survival (PFS), objective response rate (ORR), and duration of response (DoR), all assessed by an independent review committee. After a median follow-up of 8.6 months, the PFS was 7.6 months in Arms A and B, compared to 5.5 months in Arm C (hazard ratio 0.524, 95% CI 0.370-0.742, p < 0.001 for Arm A vs C; HR 0.478, 95% CI 0.336-0.679, p < 0.001 for Arm B vs C). The arms with tislelizumab experienced higher ORRs and longer DOR, which were 72.5% and 8.2 months in Arm A, 74.8% and 8.6 months in Arm B, and 49.% and 4.2 months in Arm C. In terms of adverse events, discontinuation due to treatment was found in 12.5% of Arm A, 29.7% of Arm B, and 15.4% of Arm C. The adverse events found were consistent with known adverse events of chemotherapy. Overall, this study demonstrated that tislelizumab combined with chemotherapy significantly reduced the risk for progression or death in advanced squamous non-small-cell lung cancer patients.
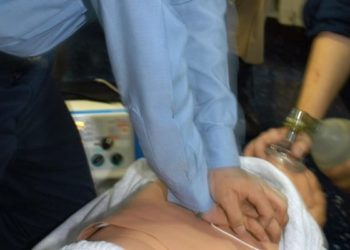
1. In comatose patients in the ICU, polyethylene eye covers were superior to artificial teardrops and normal saline eye drops for the reduction in incidence and severity of ocular surface diseases.
Evidence Rating Level: 1 (Excellent)
For patients who are critically ill or comatose, eye care is often not considered a high priority due to the other life-threatening conditions that are present. However, Ocular Surface Disease (OSD) is a common complication in these patients, and insufficient eye care can lead to more severe issues such as corneal abrasions, ulcerations, perforations, and potentially loss of vision. Besides eyedrops, moisturizing polyethylene eye covers have some evidence supporting its feasibility, although its efficacy required further investigation. The current study compared the efficacy of polyethylene eye covers, versus artificial teardrops and normal saline drops, in reducing the incidence and severity of OCD for comatose patients. The study was based out of three intensive care units in Iran, involving 79 patients: 25 patients were randomized into Group A, receiving artificial teardrops in the left eye and normal saline in the right; 29 patients were in Group B, receiving polyethylene cover in the left and normal saline in the right; and 25 patients were in Group C, receiving polyethylene cover in the left and artificial teardrops in the right. The study found OSDs in 41.14% of the 158 eyes observed. When comparing the incidence of OSDs in Group A, the artificial drops were significantly more effective at preventing OSDs (p = 0.002). For Groups B and C, polyethylene covers were significantly more effective compared to normal saline and artificial drops (p = 0.001 and 0.008 respectively). In addition, the polyethylene eye covers were superior in reducing the OSD severity (p < 0.001). Overall, this study demonstrated the efficacy of polyethylene eye covers in lowering the incidence and severity of OSDs in comatose patients, compared to normal saline and artificial tear eye drops.
Ponesimod compared with Teriflunomide in patients with relapsing multiple sclerosis
1. Ponesimod was superior to teriflunomide for relapsing multiple sclerosis, in terms of reducing relapse rates, unique active lesions on MRI, and fatigue symptoms.
Evidence Rating Level: 1 (Excellent)
Multiple sclerosis (MS) is an autoimmune, chronic disease where demyelination and loss of axons manifest in relapses and recurrent attacks, leading to impaired neurological function. More investigations into MS treatments that are safe, effective, and convenient are still needed. The current double-blind, randomized controlled trial examined the efficacy, safety, and tolerability of two oral treatments that have been approved for recurrent MS: Ponesimod, a selective sphingosine-1-phosphate receptor modulator, and teriflunomide, a pyrimidine synthesis inhibitor. The study population consisted of 1133 patients across 28 countries, 64.9% female with a median (range) age of 37.0 (18-55) years. In terms of relapses, there were 242 relapses in the ponesimod group and 344 for teriflunomide, with ponesimod reducing the annualized relapse rate (ARR) by 30.5% (mean ARR 0.202 vs 0.290; rate ratio 0.695, 99% CLs 0.536-0.902; p < 0.001). Furthermore, a symptom score assessing fatigue in MS patients (the FSIQ-RMS) showed lower levels of fatigue at week 108 for ponesimod (mean difference -3.57, 95% CLs -5.83 to -1.32, p = 0.002). Ponesimod also reduced the mean number of combined unique active lesions per year by 56%, as assessed on MRI (1.405 vs 3.164; rate ratio 0.444, 95% CLs 0.346-0.542; p < 0.001). However, the difference in 12-week and 24-week confirmed disability accumulation risk estimates were found to be not significantly different. Overall, this study demonstrated the superiority of ponesimod to teriflunomide in terms of efficacy in reducing relapses and tolerability of symptoms.
Image: PD
©2021 2 Minute Medicine, Inc. All rights reserved. No works may be reproduced without expressed written consent from 2 Minute Medicine, Inc. Inquire about licensing here. No article should be construed as medical advice and is not intended as such by the authors or by 2 Minute Medicine, Inc.