2 Minute Medicine Rewind August 18 – August 25, 2014
In this section, we highlight the key high-impact studies, updates, and analyses published in medicine during the past week.
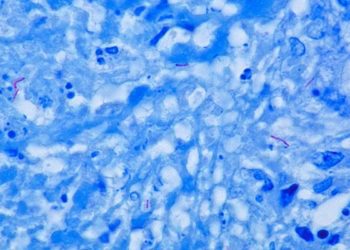
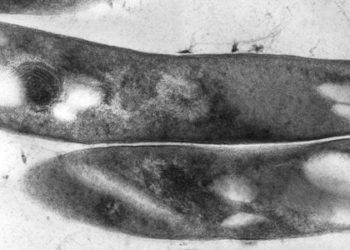
Multidrug-Resistant Tuberculosis and Culture Conversion with Bedaquiline
The incidence of tuberculosis in 2012 was estimated at 8.6 million according to the World Health Organization (WHO), and multidrug-resistant tuberculosis remains a challenge worldwide. Bedaquiline is the first drug inhibiting the mycobacterial ATP synthase to be approved for multidrug-resistant tuberculosis in 40 years. In this phase 2b multinational randomized controlled trial, 160 patients ages 18 to 65 with newly diagnosed, smear positive, multidrug-resistant pulmonary tuberculosis were assigned to receive either 400 mg of Bedaquiline daily for 2 weeks, followed by 200 mg three times weekly for 22 weeks, or placebo, with both groups also receiving a preferred five drug anti-tuberculosis background regiment. Patients were followed for 120 weeks, and time to culture conversion was studied as the primary endpoint. Time to culture conversion was 125 days in the placebo group and 83 days in the Bedaquiline group (hazard ratio in Bedaquiline group, 2.44, 95% CI: 1.57 to 3.80, p<0.001 by Cox regression analysis). Culture conversion rates were observed to be 79% in Bedaquiline group vs 58% in placebo group at 24 weeks (p=0.008) and 62% in Bedaquiline group vs 44% in placebo group at 120 weeks (p=0.04). Although the incidence of side effects in both groups was similar, the number of deaths in the two groups differed without a clear causal pattern (10 deaths in Bedaquiline group vs 2 deaths in the placebo group).The addition of Bedaquiline to the standard regiment, therefore, increases the probability of culture conversion and decreases time to culture conversion compared to placebo in multidrug-resistant tuberculosis; however, the increased number of deaths in Bedaquiline group calls for further investigation.
Newborn Screening for Severe Combined Immunodeficiency in 11 Screening Programs in the United States
The incidence of SCID has been estimated at 1 in 100,000 births. More than 80% of newborns with SCID lack family history of this condition, emphasizing the importance of early screening for the disease with benefits of early intervention. Furthermore, there is already an assay that has been developed, termed TREC, that can be used to detect T cell lymphopenias in newborns, and several states have already been implementing it. In this epidemiological and retrospective observational study, 10 states and Navajo Area Indian Health Service that have been conducting newborn screening for T cell lymphopenia submitted their data on 3030083 newborn infants screened for SCID. The infants diagnosed with the condition were classified, with incidence of the disease, its etiologies, and early interventions and survival rates recorded. Fifty two cases of typical SCID, leaky SCID and Omenn syndrome were detected and incidence rate for SCID was determined to be 1 in 58000 infants (95% CI: 1/46,000 – 1/80,000). The survival rates for infants with SCID following various interventions were the following: 87% following immune reconstitution, 92% following transplant, enzyme replacement, and/or gene therapy. Other interventions that were employed following the diagnosis of T cell lymphopenia included immunoglobulin infusions, preventative antibiotics and avoidance of live vaccines.
Effect of Oximetry on Hospitalization in Bronchiolitis: A Randomized Clinical Trial
Bronchiolitis is the leading cause of infant hospitalizations in the United States, costing over 1 billion dollars per year. Recent theories have proposed that the use of pulse oximetry might be contributing to the trend of increased hospitalizations for bronchiolitis, despite no clear evidence for oxygen saturation cutoff values that would definitively predict outcomes in this condition. This double blind randomized parallel group trial conducted in Toronto, Canada, enrolled 213 infants ages 4 weeks to 12 months with mild to moderate bronchiolitis and true oxygen saturations of 88% or higher and examined whether infants whose oxygen saturations were artificially increased by 3 points experienced significantly different rates of hospitalizations within 72 hours. The secondary variables studies in this trial included use of supplemental oxygen in the emergency room, level of physician agreement with discharge from the emergency department, length of the emergency department stay, and unscheduled visits for bronchiolitis within 72 hours. The difference in hospitalizations between the two groups was 16% (95% CI: 3.6 to 28.4, p=0.005). None of the differences in the secondary variables between the two groups were significant. This study thus suggests that high value might be placed on oxygen saturations in patients with bronchiolitis when determining whether an admission to the hospital is needed and that its use might need to be reevaluated in the future.
Oral GS-5806 Activity in a Respiratory Syncytial Virus Challenge Study
RSV infections is the most common reason for infant hospitalizations and also presents a high outpatient burden. At this time, the standard of care for bronchiolitis is supportive, and a safe and effective RSV therapy is needed. This study evaluated the efficacy of a new oral RSV-entry inhibitor GS-5806. In this double-blind, placebo-controlled study, 144 healthy adults received a challenge strain of RSV intranasally and were assigned into different cohorts receiving either placebo pill or different regiments of GS-5806 to study the area under the curve for the viral load, assessed after the administration of the first dose of medication through the 12th day after inoculation, as well as mucus weight and symptom scores. Cohorts 1-4 received the first 50 mg dose of GS-5806 and then 25 mg doses daily for the next 4 days, cohort 5 received the first 50 mg dose followed by 25 mg doses for the next 2 days, cohort 6 received one 100 mg dose, and cohort 7 received a first 10 mg dose followed by 5 mg daily for the next 4 days. In cohorts 1-4, treatment with GS-5806 resulted in lower viral load (adjusted mean, 250.7 vs 757.7 log plaque forming unit equivalents x hours per milliliter, p<0.001), lower total mucus weight (6.9 vs 15.1, p=0.03) and lower area under the curve for the change in symptom scores from baseline (-20.2 vs 204.9 x hours, p=0.005). The differences in these measures between treatment groups and placebo were also significant in cohorts 5-7. None of the subjects experienced a severe adverse effect.
Controlled Trial of Transfusion for Silent Cerebral Infarcts in Sickle Cell Anemia
Sickle cell anemia affects approximately 100,000 people in the US, and silent cerebral infarcts (with evidence of infarct on imaging, but no deficits on a neurologic exam) appear to be the most common neurologic injury in this population. At this time, the most efficacious treatment for patients with prior silent cerebral infarcts is unclear, but preliminary data indicates that regular blood transfusions might be helpful in preventing further cerebrovascular events. In this randomized single blind trial, 196 children ages 5 to 15 years, with sickle cell anemia and with prior history of silent cerebral infarcts but no history of strokes resulting in neurological deficits, were assigned to transfusion group, receiving regular blood transfusions, or standard care group, and the rate of occurrence of stroke or a new or enlarged silent cerebral infarct was evaluated. In the transfusion group, one patient had a stroke, 5 had new or enlarged silent infarcts. In the observation group, 7 patients had strokes and 7 had new or enlarged silent cerebral infarcts. The incidence of recurrent infarcts was established to be 2 and 4.8 events per 100 years at risk in transfusion and observation groups, respectively, with the incidence rate ratio of 0.41 (95% CI: 0.12 to 0.99, p=0.04). Thus, this study showed that regular blood transfusion therapy might be a beneficial intervention in children with sickle cell who might be predisposed to cerebrovascular events.
Image: PD
©2012-2014 2minutemedicine.com. All rights reserved. No works may be reproduced without written consent from 2minutemedicine.com. Disclaimer: We present factual information directly from peer reviewed medical journals. No post should be construed as medical advice and is not intended as such by the authors or by 2minutemedicine.com. PLEASE SEE A HEALTHCARE PROVIDER IN YOUR AREA IF YOU SEEK MEDICAL ADVICE OF ANY SORT.