2 Minute Medicine Rewind December 31-January 6, 2013
Image: PD/Tau Protein Alzheimer Disease
In this section, we will highlight the key high-impact studies, updates, and analyses published in medicine during the past week.
Romosozumab in Postmenopausal Women with Low Bone Mineral Density
Current osteoporosis medications increase bone mineral density and prevent the progression of structural damage but may not restore bone structure. Stimulation of bone formation is necessary to achieve improvements in bone mass, architecture, and strength. The monoclonal antibody romosozumab binds to sclerostin, osteocyte-derived inhibitor of osteoblast activity, and increases bone formation. In this Phase 2 randomized control trial, 419 postmenopausal women with low bone mineral density were assigned to receive subcutaneous romosozumab monthly or every 3 months, subcutaneous placebo, oral alendronate or subcutaneous teriparatide. All dose levels of romosozumab were associated with significant increases in bone mineral density at the lumbar spine (an increase of 11.3% with the 210-mg monthly dose, as compared with a decrease of 0.1% with placebo and increases of 4.1% with alendronate and 7.1% with teriparatide) as well as at the total hip and femoral neck. In addition, all patients receiving romosozumab sustained decreases in serum β-CTX, a bone-resorption marker. Given adverse events were similar in all groups, these results support further evaluation of romosozumab as a treatment for patients with osteoporosis.
Stenting and Medical Therapy for Atherosclerotic Renal-Artery Stenosis
Renal-artery stenosis has a prevalence of 1 to 5% of people with hypertension and as high as 7% for the general population over 65 years of age. Although past trials studying treatment with renal-artery angioplasty failed to show a benefit with respect to blood pressure or kidney function, no studies have directly assessed clinical outcomes. In this randomized control trial, 947 patients with atherosclerotic renal-artery stenosis and either systolic hypertension (on two or more antihypertensive drugs) or chronic kidney disease were assigned to medical therapy plus renal-artery stenting or medical therapy alone. The rate of occurrence of adverse cardiovascular and renal events did not differ significantly (35.1% with stenting and medical therapy and 35.8% with medical therapy alone; hazard ratio with stenting, 0.94; 95% confidence interval 0.76 to 1.17; P=0.58), nor did all-cause mortality. Thus, although there was a modest decrease in blood pressure in the stent group, renal-artery stenting does not offer significant benefit with respect to the prevention of clinical events at this time.
Effect of Vitamin E and Memantine on Functional Decline in Alzheimer Disease
Vitamin E and memantine have been shown to have beneficial effects in moderately severe Alzheimer disease (AD), but there is limited evidence in mild to moderate AD. In this randomized control trial, 613 veterans with mild to moderate AD (MMSE score between 12 and 26 currently taking an AChEI) received either alpha tocopherol, memantine, the combination, or placebo. Alzheimer’s Disease Cooperative Study/Activities of Daily Living (ADCS-ADL) Inventory scores declined by 3.15 units (95% CI, 0.92 to 5.39; adjusted P = .03) less in the alpha tocopherol group compared, a delay in clinical progression of 19% per year compared with the placebo group. There were no significant differences in the groups receiving memantine alone or memantine plus alpha tocopherol. Thus, these findings suggest benefit of alpha tocopherol in mild to moderate AD.
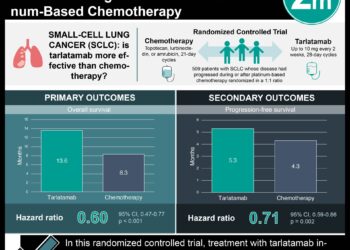
The incidence of lung cancer continues to be extremely high with an estimate of 228 000 new cases and about 160 000 deaths in the United States in 2013. In this comparative modeling study, 5 independent models were used to analyze data from the National Lung Screening Trial (NLST) and the Prostate, Lung, Colorectal, and Ovarian Cancer Screening (PLCO) trial. All models accounted for the individual’s age-specific smoking-related risk for lung cancer, date and stage of lung cancer diagnosis, the corresponding lung cancer mortality, and the individual’s life expectancy in the presence and absence of screening. The most advantageous strategy was annual CT screening for individuals ages 55 through 80 years with 30 or more pack-years’ exposure to smoking with less than 15 years since quitting. This strategy would lead to 575 screenings examinations per lung cancer death averted, a 14% (range, 8.2% to 23.5%) reduction in lung cancer mortality, 497 lung cancer deaths averted, and 5250 life-years gained per the 100 000-member cohort. Harms would include 67 550 false-positive test results, 910 biopsies or surgeries for benign lesions, and 190 overdiagnosed cases of cancer.
Thus, the USPSTF now recommends annual screening for lung cancer with low-dose computed tomography in adults aged 55 to 80 years who have a 30 pack-year smoking history and currently smoke or have quit within the past 15 years. Screening should be discontinued once a person has not smoked for 15 years or develops a health problem that substantially limits life expectancy or the ability or willingness to have curative lung surgery. (B recommendation)
The LINC Randomized Trial
Early recognition of cardiac arrest, effective cardiopulmonary resuscitation (CPR) and defibrillation, and postresuscitation care are all important factors in the survival rate after a cardiac arrest. The effectiveness of manual chest compressions depends on the endurance and skills of rescuers, and manual compressions provide only approximately 30% of normal cardiac output. Mechanical chest compression devices have therefore been developed to improve CPR, but whether these devices offer a clinical advantage has yet to be thoroughly studied. In this randomized clinical trial, 2589 patients with out-of-hospital cardiac arrest were randomized to receive either mechanical chest compressions combined with defibrillation during ongoing compressions or to manual CPR. Four-hour survival was achieved in 23.6% of patients with mechanical CPR and 23.7% of patients with manual CPR (risk difference, –0.05%; 95% CI, –3.3% to 3.2%; P > .99). There was also no significant difference in survival and neurological outcomes at hospital discharge, 1 month and 6 months. Thus, mechanical CPR does not result in improved effectiveness and clinical outcomes compared with manual CPR.
By Annick Aubin-Pouliot and David Ouyang
©2012-2014 2minutemedicine.com. All rights reserved. No works may be reproduced without written consent from 2minutemedicine.com. Disclaimer: We present factual information directly from peer reviewed medical journals. No post should be construed as medical advice and is not intended as such by the authors or by 2minutemedicine.com. PLEASE SEE A HEALTHCARE PROVIDER IN YOUR AREA IF YOU SEEK MEDICAL ADVICE OF ANY SORT. Content is produced in accordance with fair use copyrights solely and strictly for the purpose of teaching, news and criticism. No benefit, monetary or otherwise, is realized by any participants or the owner of this domain.