2 Minute Medicine Rewind June 17, 2019
Suicide in older adults living in or transitioning to residential long-term care, 2003 to 2015
It is estimated that by the year 2050, 1 in 5 individuals will be 65 years or older. In addition to the growing number of seniors in North America, the rate of suicide has also risen considerably, particularly in this patient population. As such, there is a need to identify clinically meaningful predictors of suicide and better understand the settings in which suicidal behavior takes place as a means of creating ‘points of engagement’ for risk reduction. In this cross-sectional study, researchers analyzed data from the National Violent Death Reporting System (NVDRS), to estimate the number of suicides associated with residential long-term care (LTC) in adults age 55 years and older. Among 47,759 deaths in individuals age 55 years and older (median age 64 years, 77.6% male), 1073 suicides or undetermined deaths were associated with LTC. Specifically, this included 428 suicide deaths among older adults living in an LTC facility, 449 suicide deaths among older adults transitioning into or out of LTC, and160 suicide deaths otherwise associated with LTC. Researchers found that deaths that occurred in LTC were more likely to be among women. In addition, decedents in undergoing transition either in or out of LTC were more likely to have endorsed suicidal ideation and more likely to have a physical health issue cited as a contributing to this, relative to those living in LTC. Individuals whose death was otherwise associated with LTC were also more likely to be in a relationship, endorse depressed mood, and have had a recent crisis as a contributing factor. There was no significant change in the number of suicides associated with LTC over time (p=0.85). This study therefore shows that seniors transitioning into or out of LTC may represent a vulnerable patient population with respect to suicide risk. This has important implications as more can be done to support the mental health of seniors living in LTC.
For patients with end-stage renal disease, the type of hemodialysis access selected has a direct effect on complication rates and associated healthcare costs. Typically, morbidity and mortality is lower with arteriovenous fistula (AVF) as compared to arteriovenous graft (AVG), or central venous catheter use; as such, clinical practice guidelines for hemodialysis access recommend the use of AVF whenever feasible. In this cohort study, Medicare Carrier clams (2016-2017) for all patients undergoing initial permanent hemodialysis access placement (n=85,320) were used to explore contemporary rates of AVF versus AVG use and determine physician characteristics associated with high AVG use. Researchers found that 77.9% of patients undergoing first-time hemodialysis placement had an AVF, compared to 22.1% of patients receiving an AVG. Among the 2397 surgeons who performed more than 10 procedures per year, the median surgeon level AVG use rate was 18.2%; however there were 498 surgeons (20.8%) who had an AVG use rate exceeding 34%. Upon adjusting for patient characteristics, surgeon factors that were independently associated with AVG use included more than 30 years of clinical practice when compared to surgeons with 21-30 years of clinical practice (OR 0.85, 95% CI 0.75 to 0.96), metropolitan setting (OR 1.25, 95% CI 1.02 to 1.54) and vascular surgery specialty (OR 0.77, 95% CI 0.69 to 0.86) versus general surgery specialty. This study therefore shows that as many as 20% of surgeons have an AVG use rate above recommended best practice guidelines. Sharing benchmarked performance data with surgeons may be an actionable next step in shifting towards AVF with respect to hemodialysis access surgery.
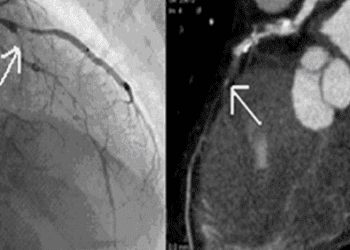
Computed tomography angiography (CTA) is being increasingly used in evaluating patients with suspected coronary artery disease (CAD) and possible angina. It is currently unclear, however, which patient subgroups in which CTA demonstrates the highest diagnostic clinical performance. In this meta-analysis, individual patient data (n=5332) from 64 prospective diagnostic accuracy studies was used to determine whether CTA should be performed in patients with any clinical probability of CAD, and whether the diagnostic performance of this test differs between patient subgroups. For a pretest probability range of 7% to 67%, the treat threshold of more than 50% and the no-treat threshold of less than 15% post-test probability were obtained using CTA. Researchers found that at a pretest probability of 7%, the positive predictive value of CTA was 50.9% (95% CI 43.3% to 57.7%) and the negative predictive value of CTA was 97.8% (95% CI 96.4% to 98.7%). The corresponding values at a pretest probability of 67% were 82.7% (95% CI 78.3% to 86.2%) and 85.0% (95% CI 80.2% to 88.9%), respectively. The sensitivity of CTA was 95.2% (95% CI 92.6% to 96.9%) while the specificity was 79.2% (95% CI 74.9% to 82.9%). The area under the receiver-operating-characteristic (ROC) curve for CTA was 0.897 (95% CI 0.889 to 0.906). Importantly, the diagnostic performance of CTA was slightly lower in patients older than 75, with an area under the ROC curve of 0.864 (95% CI 0.834 to 0.894) when compared to all other age groups (p=0.018). The diagnostic performance of CTA was also slightly lower in women (p<0.001). The diagnostic performance was not significantly influenced by angina pectoris type. This study therefore shows that the diagnosis of obstructive CAD using coronary CTA in patients with stable chest pain was most accurate when the clinical pretest probability was between 7% and 67%. The performance of CTA was not influenced by angina pectoris type and was slightly lower in older patients and in women.
Child deaths due to diarrhea and malaria are not uncommon in many low- and middle-income countries. In resource-poor settings, community health workers (CHWs) have been instrumental in the delivery of a wide range of interventions, including nutritional, neonatal health, and maternal health interventions. The impact of CHW programs focused on preventing infectious diseases in children, however, through behavior change communication, has not been well studied. In Ghana, community health volunteers (CHVs) are trained for less than 6 weeks and are tasked with providing health education, birth and death registration, disease surveillance, and minor illness treatment. In this cluster-randomized trial, 40 communities in the Volta Region, Ghana, were randomly allocated to an intervention or control arm to examine the effect of CHVs on child diarrhea and fever prevalence in rural Ghana. Over the course of the study period, 1,956 children were recruited and followed up. Researchers found that CHV home visits had no significant effect on diarrhea or fever prevalence after a follow-up of 12 months, where the prevalence of diarrhea and fever was 7.0% and 18.4%, respectively, in the control communities, versus 4.5% and 14.7%, respectively, in the intervention communities. This study therefore shows that CHV home visits have no significant impact on the prevalence of child diarrhea or fever. Of note, this trial may have been underpowered to detect small to moderate effects in both the intervention and control group.
Previous studies have suggested that certain hormonal contraceptive methods, including intramuscular depot medroxyprogesterone acetate (DMPA-IM), may increase women’s susceptibility to HIV acquisition. In this randomized, open-label trial, 7829 women living in areas of high HIV incidence in Africa were randomly assigned to receive DMPA-IM (n=2609), a copper intrauterine device (IUD) (n=2607) or levonorgestrel implant (n=2613) to compare these contraceptive methods. The primary endpoint was incident HIV infection in the modified intention-to-treat population, including all randomised participants who were HIV negative at enrollment and who contributed at least one HIV test. Researchers found that 397 HIV infections occurred (incidence 3.81 per 100 woman-years, 95% CI 3.45 to 4.21). Of these, 143 occurred in the DMPA-IM group (incidence 4.19 per 100 woman-years, 95% CI 3.54 to 4.94), 138 in the copper IUD group (incidence 3.94 per 100 woman-years, 95% CI 3.31 to 4.66), and 116 in the LNG implant group (incidence 3.31 per 100 woman-years, 95% CI 2.74 to 3.98). Based on the modified intention-to-treat analysis, there was no significant difference in HIV risk among the methods evaluated. This study shows, however, that the incidence of HIV in this population of women seeking contraception is high, thus underlining the need for integration of HIV prevention within contraceptive services for African women.
Image: PD
©2019 2 Minute Medicine, Inc. All rights reserved. No works may be reproduced without expressed written consent from 2 Minute Medicine, Inc. Inquire about licensing here. No article should be construed as medical advice and is not intended as such by the authors or by 2 Minute Medicine, Inc.