2 Minute Medicine Rewind January 14, 2019
Individuals that drive while under the influence of alcohol are at an increased risk of being involved in traffic accidents, contributing to the morbidity and mortality of the individual and others. In this observational natural experiment in Scotland, the effects of lowering the legal driving limit from a blood alcohol content (BAC) of 0.08 grams per deciliter to 0.05 grams per deciliter were examined. Specifically, investigators evaluated the impact of this legislation on alcohol consumption and traffic accidents, using those in England and Wales, where laws did not change, as a control group. Using market research of on-trade (bars and restaurants) and off-trade alcohol consumption (grocery and convenience stores), as well as police reports and automated traffic counters, both alcohol consumption and traffic accident rates were estimated. Researchers found no significant difference in accident rates in Scotland before and after the change in legal limit (RR 1.01, 95% CI 0.94 to 1.08, p=0.77). Compared to England and Wales, the rate of accidents in Scotland was significantly higher after the lowering of the BAC limit (RR 1.07, 95% CI 1.02 to 1.13, p=0.007). Additionally, there was no significant change in per-capita off-trade sales (-0.3%, 95% CI -1.7 to 1.1, p=0.71). However, there was a significant decrease in per-capita on-trade sales estimates (-0.7%, 95% CI -0.8 to -0.5%, p<0.0001). Investigators concluded that lowering the legal driving limit for BAC did not lead to a reduction in traffic accidents, but did lead to a slight reduction in consumption of alcohol in bars and restaurants.
Secondary progressive multiple sclerosis (SPMS) is the second most common type of multiple sclerosis, a demyelinating syndrome of the central nervous system. Previous studies have suggested that B-cells have a prominent role in the pathogenesis of MS. Rituximab, a monoclonal CD20 antibody, may affect the B-cell population within the central nervous system (CNS) through depletion of the peripheral B-cell compartment. The purpose of this cohort study of 88 patients with SPMS was to analyze disability progression in patients with SPMS treated with rituximab compared with matched control patients never treated with rituximab. Disability was measured using the Expanded Disability Status Scale (EDSS) score. Researchers found that after a mean follow-up of 3.5 years for patients treated with rituximab and 4.8 years in the control group, patients who had received rituximab had significantly lower EDSS scores with a mean difference of -0.52 (95% CI -0.79 to -0.26, p<0.001). Additionally, the time to progression of disability was prolonged in the group treated with rituximab (HR 0.49, 95% CI 0.26 to 0.33, p=0.03). Investigators therefore concluded that rituximab therapy for SPMS resulted in lower EDSS scores and delayed disability progression, as compared to matched patients who did not receive rituximab therapy.
Hormone replacement therapy (HRT), often prescribed to women during menopause, has been shown to increase the risk for venous thromboembolism (VTE). However, the effects of different types of HRT preparations on the risk of VTE have not been thoroughly investigated. This case-control study enrolled women between the ages of 40 and 79 years living in the United Kingdom who had a diagnosis of VTE (n=80,396), as well as controls who had no such diagnosis (n=391,494) to assess the association between risk of VTE and the use of different types of HRT. Researchers found that 7.2% of patients with a VTE had been exposed to HRT, as compared to 5.5% of controls. Oral HRT was associated with a significant increase in risk for VTE (OR 1.58, 95% CI 1.52 to 1.64) compared to individuals with no exposure, with results remaining significant upon stratifying patients that received estrogen-only preparations (OR 1.40, 95% CI 1.32 to 1.48) and combined preparations (OR 1.73, 95% CI 1.65 to 1.81). Of note, estradiol had a significantly lower risk than both equine estrogen (OR 0.85, 95% CI 0.76 to 0.95) and combined preparations (OR 0.83, 95% CI 0.76 to 0.91). The lowest risk for VTE of any of the oral preparations, when compared with no HRT, was found with the use of estradiol with dydrogesterone (OR 1.18, 95% CI 0.98 to 1.42). The highest risk was associated with medroxyprogesterone acetate (OR 2.10, 95% CI 1.92 to 2.31). Transdermal therapy did not increase the risk for VTE, as compared to no HRT (OR 0.93, 95% CI 0.87 to 1.01). Investigators therefore concluded that there were differences among HRT preparations in terms of VTE risk. Transdermal preparations were associated with no increased risk of this phenomenon.
Carotid endarterectomy (CEA) is an effective tool for revascularization in patients with carotid artery stenosis. However, in the setting of asymptomatic stenosis, careful risk-benefit analysis is needed in determining whether the long-term benefits of revascularization outweigh the short-term risks of the procedure. In this cohort study, 2325 veterans age 65 years and older that received both carotid imaging and CEA in the Veterans Administration (2005-2009) were followed up and analyzed to develop a tool that allows for patient selection in those with asymptomatic carotid stenosis. Researchers found that the 5-year mortality rate after CEA was 29.5% in this cohort. A risk prediction tool, the Carotid Mortality Index (CMI), using 23 variables was developed and evaluated. Additionally, a simpler tool with only four variables, congestive heart failure, chronic kidney disease, any cancer in the past 5 years, and chronic obstructive pulmonary disease, was evaluated. The area under the curve (AUC), a measure of discrimination, was used to assess the models. The CMI had an optimism-corrected AUC of 0.687 while the simpler model had a result of 0.657. Both had acceptable calibration curves, another measure of discrimination. Investigators therefore concluded that both of these tools could be used to improve selection of patients for CEAs in those with asymptomatic carotid stenosis.
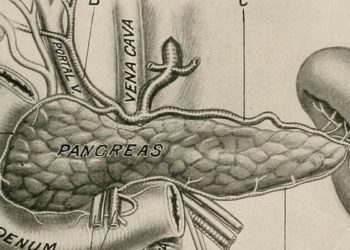
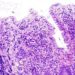
Ampullary adenocarcinoma, arising at the ampulla of Vater in the duodenum, is a gastrointestinal malignancy often treated with surgical resection with curative intent. However, the histopathologic characteristics of the resected tumor that may help predict the course of the disease are unknown. This retrospective cohort study enrolled patients who underwent pancreatoduodenectomy with curative intent for ampullary adenocarcinoma (n=887) to define histopathologic characteristics that independently predict overall survival and disease-free survival in this patient population. The median overall survival was 64 months. Researchers found that independent predictors of overall survival included adjuvant chemotherapy, which improved overall survival (HR 0.69, 95% CI 0.48 to 0.97), N-stage (HR 3.30, 95% CI 2.09 to 5.21) and perineural invasion (HR 1.50, 95% CI 1.01 to 2.23) were also both independently associated with lower overall survival. N-stage was also an independent adverse predictor for disease-free survival (HR 2.65, 95% CI 1.65 to 4.27), while other variables were not independently associated. Investigators therefore concluded that certain histopathologic characteristics help predict survival after the resection of ampullary adenocarcinoma with curative intent.
Image: PD
©2019 2 Minute Medicine, Inc. All rights reserved. No works may be reproduced without expressed written consent from 2 Minute Medicine, Inc. Inquire about licensing here. No article should be construed as medical advice and is not intended as such by the authors or by 2 Minute Medicine, Inc.


![2 Minute Medicine: Pharma Roundup: Price Hikes, Breakthrough Approvals, Legal Showdowns, Biotech Expansion, and Europe’s Pricing Debate [May 12nd, 2025]](https://www.2minutemedicine.com/wp-content/uploads/2025/05/ChatGPT-Image-May-12-2025-at-10_22_23-AM-350x250.png)