Higher rates of hospitalization from COVID-19 in non-Hispanic black patients in Louisiana
1. Non-Hispanic black patients were shown to have higher rates of hospitalization and death from coronavirus disease 2019 (COVID-19) compared to non-Hispanic white patients in a single hospital system in Louisiana.
2. Non-Hispanic black patients did not have higher rates of in-hospital mortality compared to non-Hispanic white patients.
Evidence Rating Level: 2 (Good)
Study Rundown: Determining the clinical characteristics and outcomes of hospital patients with coronavirus disease 2019 (COVID-19) is essential for understanding the epidemiology of the disease. Data from United States patients suggests diabetes, cardiovascular disease, and chronic lung disease increase the risk for severe COVID-19-associated disease. Many reports on COVID-19 highlight age and sex-related differences in health outcomes, however, racial and ethnic differences in outcomes are not yet described in depth. As such, this study compared the clinical characteristics and hospital course COVID-19 cases among non-Hispanic black patients and non-Hispanic white patients in Louisiana. Clinical data was taken from the electronic medical records from the Ochsner Health System, which is the largest integrated-delivery health system in the state. The study determined non-Hispanic black patients had a higher rate of hospitalization and deaths from COVID-19 compared to non-Hispanic white patients. However, non-Hispanic black patients did not have a higher rate of in-hospital mortality compared to non-Hispanic white patients. This retrospective study was limited by analyzing the patient characteristics of only one integrated-delivery health system in Louisiana. Therefore, the generalizability of the study conclusions needed to be cautiously made for other health care settings where the patient population and hospital care expertise are different. Further, laboratory testing was not performed in all patients. Therefore, the clinical presentation of the study population may not be sufficiently represented in the study. Nonetheless, this study was strengthened by the addition of a large population of non-Hispanic black patients from the southern region of the United States to existing COVID-19 epidemiologic data. For physicians, these findings highlight the existing differences in the clinical course of COVID-19 based on race in patients.
Click to read the study in NEJM
Relevant Reading: Characteristics of and Important Lessons From the Coronavirus Disease 2019 (COVID-19) Outbreak in China
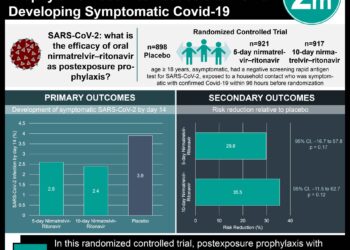
In-Depth [retrospective cohort]: This retrospective, observational, cohort study analyzed the clinical characteristics of 3481 patients in a single health system study consisted on 40 hospital and at least 100 health centers. Inclusion criteria included patients seen at an Ochsner Health facility between March 1 and April 11, 2020, a positive qualitative polymerase-chain reaction assay test, and in-hospital deaths were assessed through May 7, 2020. The exclusion criteria for the study included patients seen outside the Ochsner Health facility and an unconfirmed qualitative polymerase-chain reaction assay test for the virus. Clinical data were taken from electronic medical records, which included the following: demographics (age, sex, patient-reported race, and ethnic group), chronic conditions, and laboratory testing. Statistical analyses of the data were analyzed through unadjusted and multivariable models. The primary outcomes were hospitalization and in-hospital death. In adjusted analysis of factors associated with hospitalization, black race was associated with about twice the odds of hospital admissions as white race (odds ratio, 1.96; 95% confidence interval [CI], 1.62 to 2.37). Additionally, public insurance (Medicare or Medicaid), residence in a low-income area, and obesity were associated with higher odds of admission. The Cox proportional-hazards model for factors associated with in-hospital death determined age, presentation of elevated respiratory rate, and low lymphocyte counts were associated with increased in-hospital mortality; however, black race was not independently associated with risk of in-hospital death (hazard ratio, 0.89; 95% CI, 0.68 to 1.17). Of the 326 patients who died in the hospital, 230 (70.6%) were non-Hispanic black patients. Furthermore, a higher percentage of non-Hispanic black patients (73.9%) had been treated with mechanical ventilation compared to non-Hispanic white patients (36.5%).
Image: PD
©2020 2 Minute Medicine, Inc. All rights reserved. No works may be reproduced without expressed written consent from 2 Minute Medicine, Inc. Inquire about licensing here. No article should be construed as medical advice and is not intended as such by the authors or by 2 Minute Medicine, Inc.