Aspirin vs warfarin in atherosclerotic intracranial stenosis [Classics Series]
Image: PD
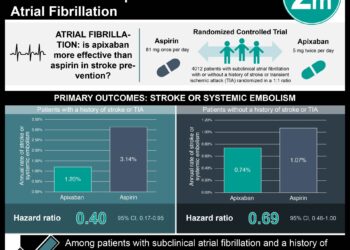
1. There was no difference between warfarin and aspirin in preventing recurrent stroke in patients with significant atherosclerotic intracranial stenosis.
2. Warfarin was associated with a significantly higher incidence of major hemorrhage compared to the aspirin group.
Original Date of Publication: March 31, 2005
Study Rundown: This trial randomized patients who were recently diagnosed with a stroke due to intracranial atherosclerotic stenosis to prophylactic treatment with either high-dose aspirin or warfarin. The trial was stopped early because the warfarin treatment group had a much higher incidence of major hemorrhages compared to the aspirin treatment group. There was no significant difference in the rate of stroke recurrence between the two groups.
In summary, this study demonstrated that aspirin should be used for secondary prophylaxis in patients who suffered an ischemic stroke due to significant atherosclerotic intracranial stenosis. Warfarin is associated with increased risk of major hemorrhage and does not provide added benefit over aspirin in preventing a second stroke.
Click to read the study in NEJM
In-Depth [randomized, controlled study]: Originally published in 2005 in NEJM, this trial enrolled 569 patients with intracranial stenosis from 59 sites in North America. In order to participate, patients had to have experienced a transient ischemic attack (TIA) or non-disabling stroke within 90 days prior to enrollment that was attributed to 50-90% stenosis of a major intracranial artery. Patients were excluded if they had any evidence of 50-90% stenosis of the extracranial carotid artery, evidence or history of atrial fibrillation, or other non-atherosclerotic causes of intracranial artery stenosis. Patients were randomized to receive 5 mg of warfarin daily or 650 mg of aspirin twice daily. A non-blinded investigator made dosage changes based on side effects and INR value. The rest of the investigating team and the patients were blinded to the treatment arms. The primary endpoint was occurrence of ischemic or hemorrhagic stroke or death from any vascular cause. Study follow-up was expected to be 36 months, however the trial was stopped early due to a significant increase of adverse events in the warfarin group. The warfarin group experienced significantly more major hemorrhages than the aspirin group (HR 0.39 95%CI 0.18-0.84) after a mean of 1.8 years of follow-up. There was no significant difference in primary endpoint outcomes between the two groups (HR 1.04, 95%CI 0.73-1.48).
By Milana Bogorodskaya and Andrew Cheung, M.D.
© 2013 2minutemedicine.com. All rights reserved. No works may be reproduced without expressed written consent from 2minutemedicine.com. Disclaimer: We present factual information directly from peer reviewed medical journals. No post should be construed as medical advice and is not intended as such by the authors, editors, staff or by 2minutemedicine.com. PLEASE SEE A HEALTHCARE PROVIDER IN YOUR AREA IF YOU SEEK MEDICAL ADVICE OF ANY SORT.