Early ART therapy for HIV-1 linked to decreased transmission: The HPTN 052 trial
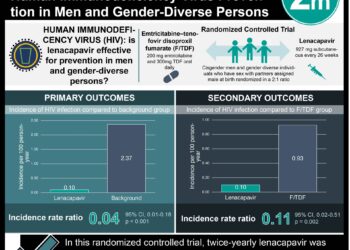
1. Individuals infected with HIV-1 who were randomized to receive antiretroviral therapy (ART) at trial enrollment had a 97% and 93% lower risk of transmitting the virus compared to those who were randomized to receive ART on a delayed basis (when CD4+ count fell below 25 or when there was AIDS-defining illness) at 1.7 and 5 years, respectively.
2. Eight cases of genetically linked viral transmission were linked either to failure of ART in index participant or to cases in which transmission occurred before virologic suppression had been achieved in the index participant.
Evidence Rating Level: 1 (Excellent)
Study Rundown: Despite advances in the prevention and therapy of HIV infection, more than 2 million new HIV-1 infections were reported worldwide in 2014. The interim analysis from the HIV Prevention Trials Network (HPTN) 052 trial established the benefit of early ART in preventing HIV-1 transmission in serodiscordant couples. The original study involved 1763 index participants diagnosed with HIV-1 and their sexual partners; in those randomized to the early-ART group, participants initiated ART at trial enrollment, while in the delayed group, ART was initiated when the CD4+ counts fell below 250 or when there was development of an AIDS-defining illness. Following the interim analysis results at a median follow-up period of 1.7 years, remaining participants in the trial were offered ART and followed to completion of 5 years of follow-up. In this extended analysis, there was a sustained, statistically and clinically significant reduction in the rate of genetically linked HIV-1 transmission between serodiscordant couples in the early versus delayed ART groups. Additionally, the authors found that there were no linked infections when virologic suppression had been achieved in the index participant.
Click to read the study, published today in NEJM
Relevant Reading: Prevention of HIV-1 infection with early antiretroviral therapy
In-Depth [randomized controlled trial]: This study reports the 5-year results from the HPTN trial, in which 886 HIV-positive participants started ART at enrollment, while 877 HIV-positive participants were randomized to a delayed treatment arm. Index participants were recruited at 13 sites in 9 countries and were determined to be HIV-positive. After the interim analysis showed that early ART prevented 96% of genetically linked infections, participants in the delayed treatment arm were offered treatment in order to maintain ethical equipoise; 83% and 96% of these participants were receiving ART at one year and trial completion, respectively. Across both groups, there were 78 partners with documented HIV infections during the course of the trial; viral linkage was established in 92% of these subjects. In the intention-to-treat analysis, early ART was associated with a 97% lower risk than delayed ART in the interim analysis (median follow-up 1.7 years) and 93% lower risk during the entire study period of 5 years. In a multivariate analysis, early ART was associated with a strongly decreased risk of transmission compared to delayed ART (HR 0.08, 95%CI 0.02-0.25); increased HIV-1 viral load, female gender of index participant, and lack of baseline condom use of 100% were all associated with an increased risk of transmission. In 8 cases of genetically linked partner infections, 4 occurred in cases in which transmission occurred before virologic suppression in the index partners, and the remaining 4 occurred after ART failed in the index participant.
Image: CC/Wiki
©2016 2 Minute Medicine, Inc. All rights reserved. No works may be reproduced without expressed written consent from 2 Minute Medicine, Inc. Inquire about licensing here. No article should be construed as medical advice and is not intended as such by the authors or by 2 Minute Medicine, Inc.