Hemicraniectomy improved survival but not functional status in MCA strokes
Image: PD
1. At 6 months, patients who underwent hemicraniectomy scored better on the Rankin scale, as compared to those who underwent ICU conservative therapy.
2. Half of surviving patients at one year in both groups had a modified Rankin score of 4, indicating inability to walk or attend to bodily functions without assistance.
Evidence Rating: Level 1 (Excellent)
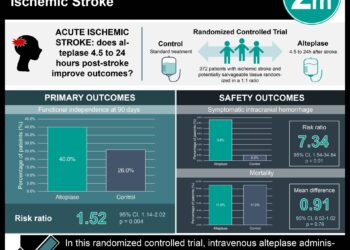
Study Rundown: This randomized controlled study compared decompressive hemicraniectomy versus conservative ICU therapy in patients over 61 years of age who had suffered a large unilateral middle cerebral artery (MCA) ischemic stroke. A previous pooled analysis of randomized control studies had shown a benefit of early hemicraniectomy, but had an upper age limit of 60 years. This study was stopped prematurely due to evidence of efficacy at the 6 month time point.
Hemicraniectomy was shown to improve the primary outcome (score of 0 to 4 on the modified Rankin scale at the 6 month time point). While survival improved in the surgery group, most survivors had substantial disability (half of surviving patients at one year in both groups had a score of 4, indicating inability to walk or attend to bodily functions without assistance; an additional one third in both groups had a score of 5, indicating bedridden, incontinent nature requiring constant attention). A majority of patients who underwent surgery indicated that they would still have given consent to the procedure (though a proportion of patients were unable to complete this questionnaire due to cognitive deficits).
Strengths of this study include the fact that it provides clinicians with evidence to inform the decision-making process surrounding possible surgical intervention in large MCA strokes, although these decisions must occur in a rapid manner. Great efforts were made to include comprehensive understanding of disability, including measurement of the outcome of depression. It was performed without commercial support.
Click to read the study, published today in NEJM
Click to read an accompanying editorial in NEJM
Relevant Reading: Early decompressive surgery in malignant middle cerebral artery infarction: a pooled analysis of three randomized controlled trials
In-Depth [randomized controlled study]: This study investigated the benefit of decompressive hemicraniectomy versus standard ICU care in 112 patients over 61 years of age with malignant middle-cerebral artery infarction. Eligibility criteria included: age 61 or older, clinical symptoms of acute unilateral MCA infarction less than 48 hours prior to initiation of treatment, score higher than 14 (right hemisphere stroke) or 19 (left hemisphere) on NIHSS scale (0 to 42, higher indicating more severe stroke), and imaging evidence of ischemia of at least two thirds of MCA territory. Patients were excluded who had preexisting evidence of functional impairment, contraindications to surgery, or an estimated life expectancy of less than 3 years. Patients were randomized to receive conservative treatment in the ICU (including osmotherapy, intubation/ventilation, hyperventilation, and buffer solutions) or surgical treatment (large hemicraniectomy and duroplasty).
The primary outcome was a score of 0 to 4 on the modified Rankin scale at 6 months (where lower scores indicate less disability); secondary end points included survival rate, NIHSS score, and measures of DALYs at 12 months following randomization. In the intention to treat analysis, the odds ratio of attaining the primary outcome was 2.91 (95% CI 1.06-7.49, P=0.04) favoring hemicraniectomy compared to ICU conservative therapy. No patients had a score of 0 to 2 on the modified Rankin scale (survival with no or slight disability); 7% of patients in the hemicraniectomy group versus 3% in the control group had a 3 (moderate disability); for score of 4 (moderately severe disability, requirement of help with most bodily needs), the rates were 32% and 15% respectively whereas for a score of 5 (severe disability), the rates were 28% versus 13%. Death occurred less frequently in the surgery group (33% vs 70%). The 12-month survival rate was 57% in the surgery group versus 25% in the control group. All secondary endpoints were significantly better in the hemicraniectomy group at 12 months. 88 serious adverse events were reported in the surgery group (highest cause: infection) versus 84 in the control group. The study was stopped midway due to demonstration of efficacy in reductions in death and severe disability after 6 months.
More from this author: Fecal occult-blood testing linked with reduction in colorectal-cancer mortality, High-flow nasal cannulae noninferior to nasal CPAP in very preterm infants after extubation, Dolutegravir regimen more effective than standard regimen in treatment of HIV-1, E. coli in mid-stream urine highly sensitive for cystitis, Oxantel pamoate results in higher cure rates of Trichuris trichiura in children
©2012-2014 2minutemedicine.com. All rights reserved. No works may be reproduced without expressed written consent from 2minutemedicine.com. Disclaimer: We present factual information directly from peer reviewed medical journals. No post should be construed as medical advice and is not intended as such by the authors, editors, staff or by 2minutemedicine.com. PLEASE SEE A HEALTHCARE PROVIDER IN YOUR AREA IF YOU SEEK MEDICAL ADVICE OF ANY SORT.