HIV infection may increase rate of HCV-related hepatic decompensation
Image: PD
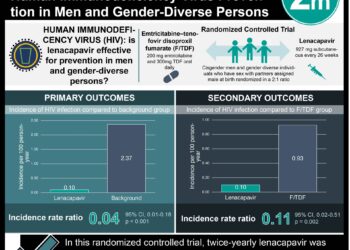
1. From a cohort study of patients infected with hepatitis C virus (HCV), those with concurrent human immunodeficiency virus (HIV) infection had a slightly higher rate of hepatic decompensation, particularly those with a lower CD4 count and higher HIV viral load.
Evidence Rating Level: 2 (Good)
Study Rundown: Concurrent HIV and HCV infection is common. Those patients affected by both viruses are known to have an increased rate of liver fibrosis compared to those who are HCV mono-infected. There have been few studies in the era of anti-retroviral therapy (ART) evaluating the risk and determinants of hepatic decompensation in co-infected patients. This retrospective cohort study compared patients co-infected with HIV and HCV with those mono-infected with HCV. The study results showed that the rate of hepatic decompensation was higher in co-infected patients (6.3% vs 5.0%). The higher rate of liver decompensation in co-infected patients persisted after adjustment for variables between study groups such as age, race, alcohol use and infection drug use (hazard ratio of 1.83). Rates of acites and bacterial peritonitis were not statistically significant between those co-infected and those mono-infected, although interestingly the rate of esophageal variceal hemorrhage was shown to be less common in co-infected patients. Among co-infected patients, those with higher HIV viral levels and those with lower CD4 counts had slightly higher incidence of hepatic decompensation. This study is limited primarily by its narrow population, which included largely male veterans. However, overall the study demonstrates the potential clinical value of ART in reducing rates of hepatic decompensation among HIV and HCV co-infected individuals.
Click to read the study, published today in the Annals of Internal Medicine
Relevant Reading: Liver fibrosis progression in human immunodeficiency virus and hepatitis C virus coinfected patients
In-Depth [retrospective cohort study]: Each HIV and HCV co-infected patient was matched with two HCV mono-infected controls, resulting in 4280 HIV/HCV co-infected patients and 6079 HCV-mono-infected patients included in the study. Data was collected between 1997-2010, and cohort analysis demonstrated two groups were largely similar, with the exception of higher HCV RNA levels in the co-infected patients. The rate of decompensation was 6.3% in co-infected patients, compared to 5.0% in mono-infected patients (p=0.004). Coinfected patients also had significantly lower rates of variceal hemorrhage (26.2% vs. 55.1%, p<0.001), and trended to have higher rates of ascites (83.4% vs. 77.4%, p = 0.07) and lower rates of spontaneous bacterial peritonitis (17.7% vs. 22.3%, p=0.171). The cumulative 10 year incidence of hepatic decompensation was only slightly affected by viral load, 0.076 in those with HIV viral level >1000 copies/mL compared to 0.069 for those with <1000. Similarly, those with a CD4 count <0.200×109 cells/L had an incidence of 0.081, compared to 0.69 among those with >0.200×109 cells/L. Many potential weaknesses of this study were addressed by demonstrating similar rates of hepatic decompensation among other patient databases, and it is strengthened by its large patient sample and 10-year long follow-up.
More from this author Peer-delivered education through social networking increases home-based HIV testing ACP recommends weight loss and CPAP for obstructive sleep apnea Lifestyle interventions can reduce type 2 diabetes among high-risk patients Home scoring system may prevent unnecessary pharyngitis clinic visits No evidence for the cognitive side-effects of statins Household firearm accessibility increases risk of suicide and homicide Transcatheter aortic valve replacement provides only minor benefit to quality of life No difference in statin-related myalgias compared to placebo in single-patient trials
©2012-2014 2minutemedicine.com. All rights reserved. No works may be reproduced without expressed written consent from 2minutemedicine.com. Disclaimer: We present factual information directly from peer reviewed medical journals. No post should be construed as medical advice and is not intended as such by the authors, editors, staff or by 2minutemedicine.com. PLEASE SEE A HEALTHCARE PROVIDER IN YOUR AREA IF YOU SEEK MEDICAL ADVICE OF ANY SORT.