Increased maternal BMI linked to higher fetal, neonate, and infant mortality
Image: PD
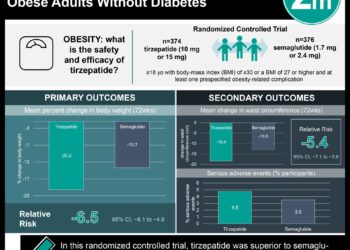
1. Maternal body mass index (BMI) was linked to the absolute risk of fetal, intrapartum, and postnatal complications.
2. Severely obese women had a 2 to 3 fold increased risk of adverse outcomes compared to women with moderate BMIs.
Evidence Rating Level: 1 (Excellent)
Study Rundown: While maternal body mass index (BMI) has previously been associated with the rate of pregnancy complications and fetal, neonatal, and infant death, the exact nature and strength of this relationship remains unknown. This study sought to elucidate this relationship and found a significantly increased relative risk of fetal death, stillbirth, perinatal death, neonatal death, and infant death per 5-unit elevation in BMI from the 20kg/ m2 reference point. Severely obese women had a 2 to 3 fold increased relative risk of adverse outcomes. This association may reflect increased rates of preeclampsia, type 2 diabetes, and congenital anomalies observed in this population, as well as obesity-related alterations in underlying biochemical mechanisms.
The strengths of this study hinge on the large combined sample size and thorough statistical analysis. Limitations presents themselves in the form of differing definitions and interval limits of outcomes. For example, stillbirth definitions ranged from fetal death at a minimum of 20 weeks to a minimum of 28 weeks. The effect of differences in maternal care must also be considered as studies were included from nations around the world. Nonetheless, the strength of this observed relationship may aid in shaping weight management strategies for women during pregnancy and will hopefully serve as an impetus for further research.
Click to read the study, published today in JAMA
Relevant Reading: 3.6 million neonatal deaths–what is progressing and what is not?
In-Depth [meta-analysis]: This metanalysis combined results from 38 cohort studies describing the association between maternal BMI and fetal death, miscarriage, stillbirth, and neonatal, postnatal, and infant death in terms of relative risk. The authors reported on relative risk at 5 BMI unit intervals with a BMI of 20 as the reference point. Relative risk per 5 unit BMI increase was significant for fetal death (RR 1.21,CI95 [1.09-1.35]), stillbirth (RR 1.24,CI95 [1.18-1.30]), perinatal death (RR 1.16,CI95 [1.00-1.35 ]), neonatal death (RR 1.15,CI95 [1.07-1.23 ]), and infant death (RR 1.18,CI95 [1.09-1.28 ]). Women with BMI of 40 had an outcome absolute risk of 0.69% to 2.7% versus the 0.20% to 0.76% outcome absolute risk observed in women with a BMI of 20.
More from this author: Tadalafil ineffective for erectile dysfunction following prostate radiotherapy, Age-adjusted D-dimer levels may rule out pulmonary embolism [ADJUST-PE trial], Warfarin beneficial in chronic kidney patients with atrial fibrillation, Radiofrequency catheter ablation effective as first-line therapy for atrial fibrillation [RAAFT-2 trial], Vitamin E associated with slower functional decline in Alzheimer disease [TEAM-AD Trial]
©2012-2014 2minutemedicine.com. All rights reserved. No works may be reproduced without expressed written consent from 2minutemedicine.com. Disclaimer: We present factual information directly from peer reviewed medical journals. No post should be construed as medical advice and is not intended as such by the authors, editors, staff or by 2minutemedicine.com. PLEASE SEE A HEALTHCARE PROVIDER IN YOUR AREA IF YOU SEEK MEDICAL ADVICE OF ANY SORT.