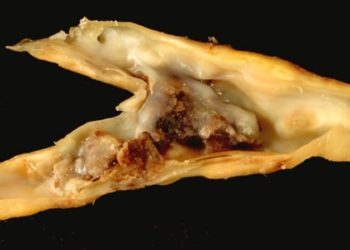
No long-term outcome differences between stenting versus surgery for carotid stenosis
1. There were no significant differences between stenting versus carotid endarterectomy (CEA) for patients with carotid stenosis (symptomatic or asymptomatic) with regards to the risk of periprocedural stroke, MI, or death and subsequent ipsilateral stroke.
Evidence Rating Level: 1 (Excellent)
Study Rundown: The Carotid Revascularization Endarterectomy versus Stenting Trial (CREST) had found no significant difference between stenting and surgery up to 4 years post procedure. This study investigated the differences in outcomes over a 10-year follow-up. CREST was a randomized, controlled trial that had recruited patients from 117 centers in the US and Canada. The study found no significant differences between the two groups in regards to the 10-year risk of any stroke, MI, or death during the periprocedural period or ipsilateral stroke thereafter. The rate of postprocedural ipsilateral stroke did not differ significantly if the patient was symptomatic, asymptomatic, had stenting or had CEA.
Click to read the study in NEJM
Relevant Reading: Stenting versus endarterectomy for treatment of carotid-artery stenosis
In-Depth [randomized controlled trial]: A total of 2502 patients were randomly assigned to undergo stenting or CEA in the CREST trial. The median follow-up was 7.4 years. There were no significant differences between the baseline clinical characteristics with the exception of dyslipidemia which was higher in the CEA group compared to the stenting group (85.8% vs 82.9% respectively; p=0.05). The primary endpoint included any stroke, MI or death during he periprocedural period or ipsilateral stroke thereafter for up to 10 years. There was no significant difference between the groups in the 10-year risk of primary composite end point (HR=1.10; 95% [CI], 0.83-1.44; p=0.51). The risk of periprocedural stroke or death and subsequent ipsilateral stroke was 37% higher in the stenting group compared to the CEA group (HR=1.37; 95% [CI], 1.01-1.86; p=0.04). During the postprocedural period, there were nominally, but not significantly, more major strokes among patients assigned to stenting than among those assigned to CEA (HR=1.91; 95% [CI], 0.71 to 5.10; p=0.20).
Image: CC/Wiki
©2016 2 Minute Medicine, Inc. All rights reserved. No works may be reproduced without expressed written consent from 2 Minute Medicine, Inc. Inquire about licensing here. No article should be construed as medical advice and is not intended as such by the authors or by 2 Minute Medicine, Inc.