Parents define children’s oncology-related palliation and pain relief [Pediatrics Classics Series]
Image: PD
1. When interviews with parents who lost children to cancer were compared to patient hospital records, researchers found that many children experienced substantial suffering toward the end of life with poorly managed symptoms.
2. There was significant discordance between parent and physician reports of patient discomfort, with parents being significantly more likely to report patient symptoms than physicians.
Original Date of Publication: February 2000
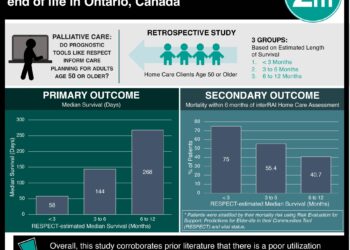
Study Rundown: In 2000, cancer was, and continues to be, a leading cause of mortality among children. While researchers previously investigated the quality of end-of-life care among adult oncology patients, no study explored palliative care for children. This study was the first to delve into the state of pediatric end-of-life care through interviews with parents who had lost children to cancer and retrospective chart analysis of these patients’ care. Results showed that many children received aggressive care at the end of their lives with nearly half dying in the hospital and many passing in the intensive care unit. In addition, 89% of children experienced substantial suffering in their last month of life, most of which went unresolved despite treatment attempts. Parents were significantly more likely to report a child’s experiencing fatigue, poor appetite, constipation, and diarrhea when compared to physician impressions in the medical records of these children. Parents were also significantly more likely to report their child to be in pain if they believed the child’s oncologist to be less involved in direct end-of-life care. These findings suggested that care providers may not be optimally treating these patients due a lack of recognized patient discomfort. Also, results showed that earlier discussions of hospice care were significantly associated with parental descriptions of children as calm in the last month of life. This study was limited by use of parental report and chart review. However, its findings had many implications for patient care. By encouraging early, direct discussions between physicians and patient families regarding symptoms, discomfort, and goals of care, researchers recognize that patients’ quality of life might improve as a patient progressed toward the end of life. Now, palliative care is better defined as care of the whole patient, involving an interdisciplinary team that is, ideally, introduced to patients and their families at the time of serious diagnosis. If effectively initiated, palliative care has the ability to not only improve satisfaction with care, but quality of life as well.
Click to read the study in The New England Journal of Medicine
In-Depth [retrospective study]: A total of 103 parents (91% white, 86% female) of children who had died of cancer during 1990-1997 were interviewed by researchers based out of a large, tertiary children’s hospital. The interview information was then combined with data obtained from chart reviews. In interviews, parents were asked to assess many aspects of his or her child’s end-of-life care including, but not limited to, physical symptoms and suffering during the last month of life, treatment of these symptoms, and the perception of physician involvement at the end of life. Several questions included grading on a Likert scale. Chart review was then completed to collect demographic data along with treatments administered, cancer care course, symptoms in the last month of life, cause and place of death, medical interventions close to the time of death, and discussions regarding end-of-life planning such as hospice and do not resuscitate orders (DNR).
Interviewed parents had children who died of leukemia or lymphoma (n = 50, 49%), brain tumors (n = 23, 22%), or other solid tumors (n = 30, 29%). Eighty-one children died from progressive disease, 21 died from treatment-related complications, with 1 child’s records unavailable for review. On chart review, physicians discussed hospice care with two thirds of children with progressive disease. Sixty-six percent of children had DNR orders in their charts. Nearly half, 49%, of patients died in the hospital and, of those, 45% passed away in the intensive care unit. From parental interview, nearly 100% of patients had at least 1 symptom toward the end of life with fatigue, pain, dyspnea, and poor appetite being the most common. Eighty-nine percent of children had “a great deal” of suffering as a result of 1 or more symptoms. Pain and dyspnea were the most commonly treated symptoms (76% and 65%, respectively), but few patients experienced relief from treatment (27% and 16%, respectively). During the last month of life, 21% of children were described by parents as being afraid. With regard to end-of-life discussions, the length of time between hospice care discussions and death were significantly longer for children whose parents found them to be calm during most of the last month of life (p = 0.01). Based upon parental report, lack of oncologist involvement in end-of-life care was associated with significantly more pain in the last month of a child’s life (OR = 2.6, 95% CI). In comparing parental interview to chart review, parents reported fatigue (p < 0.001), poor appetite (p < 0.001), constipation (p < 0.001) and diarrhea (p < 0.05) in their children significantly more often than physicians.
© 2012-2014 2minutemedicine.com. All rights reserved. No works may be reproduced without expressed written consent from 2minutemedicine.com. Disclaimer: We present factual information directly from peer reviewed medical journals. No post should be construed as medical advice and is not intended as such by the authors, editors, staff or by 2minutemedicine.com. PLEASE SEE A HEALTHCARE PROVIDER IN YOUR AREA IF YOU SEEK MEDICAL ADVICE OF ANY SORT.