Patient Basics: Glaucoma
Originally published by Harvard Health.
What Is It?
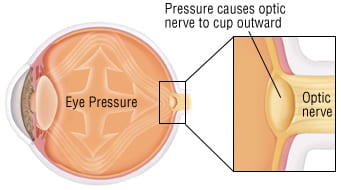
Glaucoma is a common eye condition in which vision is lost because of damage to the optic nerve. The optic nerve carries information about vision from the eye to the brain. In most cases, the optic nerve is damaged when the pressure of fluid inside the front part of the eye rises. However, glaucoma-related eye damage can occur even when the fluid pressure is normal.
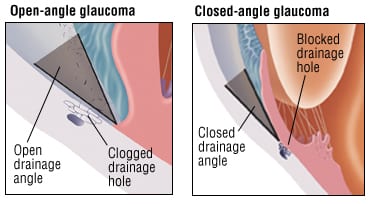
In the most common form of glaucoma, called primary open angle glaucoma, fluid circulates freely in the eye and the pressure tends to rise slowly over time. Gradual loss of vision is usually the only symptom.
A less common form of the disease, called acute or angle closure glaucoma, develops suddenly and usually causes eye pain and redness. In this form of glaucoma, pressures rise quickly because normal fluid flow within the eye becomes blocked. This happens when a structure called the angle (where the iris and cornea meet) closes.
Experts are uncertain why either form of glaucoma damages the optic nerve.
In addition to open angle and angle closure glaucoma, there are rarer forms of the illness. They may be related to eye defects that develop before birth (congenital glaucoma) or to eye injuries, eye tumors or medical problems such as diabetes. In some cases, medications, such as corticosteroids, also can trigger glaucoma.
Glaucoma is a leading cause of blindness in the United States. It currently affects as many as 2.5 million Americans. Up to half of people with glaucoma don’t know that they have the condition. Glaucoma tends to run in families. It is five times more common in African-Americans than in Caucasians. The risk of glaucoma also increases with age in people of all ethnic backgrounds.
Symptoms
Although open angle glaucoma and acute glaucoma both cause blindness, their symptoms are very different.
- Open angle glaucoma — In this form of glaucoma, vision is lost painlessly and so gradually that most people do not realize they have a problem until substantial damage has occurred. Peripheral vision (at the edges) is usually lost first, especially the field of vision near your nose. As larger areas of your peripheral vision fade, you may develop tunnel vision — vision that has narrowed so you see only what is directly in front of you, like looking through a railroad tunnel. If glaucoma is not treated, even this narrowed vision disappears into blindness. Once gone, areas of lost vision cannot be restored.
- Acute glaucoma (closed angle glaucoma) — Symptoms of acute glaucoma occur suddenly and can include blurred vision, pain and redness in the eye, severe headache, halos around lights at night, a haziness in the cornea (the clear front portion of the eye in front of the pupil), nausea and vomiting, and extreme weakness.
Diagnosis
In most cases, open angle glaucoma is diagnosed by a doctor during a routine eye examination. When looking at the back of the eye (fundus) using a special telescope, he or she may notice changes in the appearance of the optic nerve. If glaucoma is suspected, your doctor will confirm the diagnosis with one or more additional tests:
- Tonometry measures the pressure within the eye. This may be done by pressing an instrument against your eyeball, or by blowing a puff of air against your eye. Your eye pressure is measured in millimeters of mercury, commonly abbreviated as “mmHg.” Normal eye pressure is between 8 mmHg and 22 mmHg.
- Visual-field testing is the best way to find early signs of loss of peripheral vision. Most often, visual fields are checked using an automated machine. You look straight ahead into the machine and press a button when you see a blinking light. The machine then draws a picture of where you are able to see the blinking lights.
- OCT. This technique uses a LASER beam to actually measure the thickness of the nerve fibers in the retina. Glaucoma causes loss of these nerve fibers.
Your doctor will not diagnose glaucoma unless your optic nerve shows evidence of damage. However, some people will be found to have elevated eye pressure but no evidence of optic nerve damage. In this case, you may be told that you are a “glaucoma suspect” or have “pre-glaucoma,” but do not yet have the disease. It is important to remember that not everyone with elevated pressures will develop glaucoma, and that not everyone with glaucoma has elevated eye pressures.
Angle closure glaucoma usually is diagnosed in a person who has developed a red, swollen eye and difficulties with vision. The eye pressure is usually quite high. Some people may be told by their eye doctor that they are at risk of angle closure glaucoma because their angle looks narrow.
Expected Duration
Glaucoma is a lifelong illness, but proper treatment can prevent loss of vision.
Prevention
In most people, glaucoma cannot be prevented. However, regular screening may help to identify people either with early stages of the disease or elevated eye pressures. Screening should be done by someone who is trained to recognize glaucoma, usually an ophthalmologist or optometrist.
There is no consensus about who should be screened for glaucoma. African Americans over age 40 have the highest risk of developing glaucoma. Family history of glaucoma and older age also increase your risk of the disease.
Medicare covers glaucoma screening for people with diabetes, a family history of glaucoma, or African-Americans who are age 50 and older.
Treatment
In the United States, treatment of open angle glaucoma usually begins with prescription eye drops. These medicines lower pressure inside the eye.
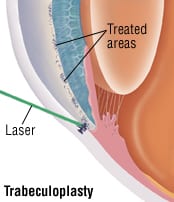
As an alternative to medication or when medication fails to control glaucoma, laser surgery can be done. This surgery is called laser trabeculoplasty. Eye surgeons perform this procedure in the office or eye clinic. A high intensity beam of light is carefully aimed at openings in the eye’s drainage system. The laser widens the openings to increase fluid drainage from the eye.
Laser surgery may not lower eye pressure to acceptable levels. You may need to continue glaucoma eye drops after laser surgery.
If both medication and laser surgery are unsuccessful, conventional eye surgery may be necessary to make a new opening for fluid to leave the eye. Eye surgeons perform this procedure in the operating room. Intravenous medication is given to help you relax. Numbing medication is applied on and around the eye. The surgeon creates a new opening to improve fluid drainage from the eye.
With both types of glaucoma surgery, eye pressure almost always decreases. But the pressure might not be low enough. You may need repeat surgery and/or need to continue long term use of glaucoma eye drops.
If you have been diagnosed with glaucoma, be sure to follow up regularly with your eye doctor. It is also important that you use your medication as directed. Many people do not follow through with treatment because they feel fine and do not notice the gradual loss of their vision. However, it is important to remember that glaucoma treatment prevents further damage to your eye, but will not restore vision that has already been lost.
Acute glaucoma must be recognized and treated within 24 hours to prevent loss of vision. Treatment usually begins with laser treatment to make a new opening in the iris that allows fluid to drain. This often cures the problem, but it sometimes is necessary to use eye drops long-term or to perform additional surgery.
When To Call A Professional
Call your doctor immediately if you notice any sudden loss of your vision, especially if you also have any pain or redness in the eye. Acute glaucoma is a sight-threatening medical emergency that requires immediate treatment to prevent blindness.
Prognosis
The outlook depends on the type of glaucoma:
- Open angle glaucoma — Proper treatment greatly reduces the risk of vision loss in people with open angle glaucoma. However, if glaucoma remains untreated, permanent blindness can occur.
- Acute glaucoma — If an episode of acute glaucoma is treated early, vision in the affected eye may return to a level that is almost the same as what it was before the episode began. If acute glaucoma is neglected, you can become blind in the affected eye within two days or less.
Additional Info
National Eye Institute
2020 Vision Place
Bethesda, MD 20892-3655
Phone: (301) 496-5248
http://www.nei.nih.gov/